Imbokodo Trial Shows HIV Vaccine Candidate Isn't Effective Enough
HIV vaccines have remained elusive in part because the virus has a powerful ability to mutate, and there are so many strains in circulation. In one clinical study, the Thai trial or RV144, an HIV vaccine provided some protection. But so far, most candidate HIV vaccines have typically been able to cause the formation of antibodies, but they haven't stopped the virus from causing infection upon exposure.
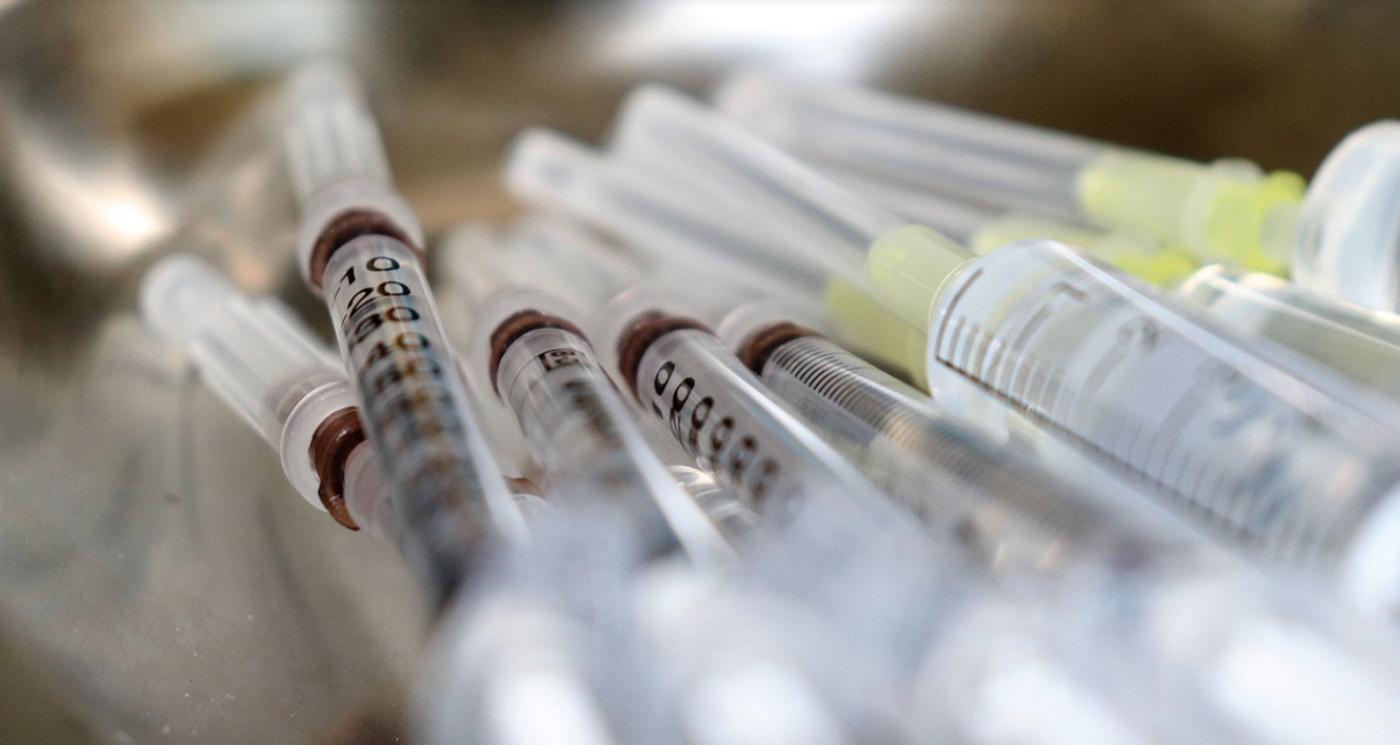
The “Imbokodo” clinical trial of a promising HIV vaccine candidate has had disappointing results. While the vaccine seems to be well-tolerated and safe to use, it did not prevent HIV infection in more than about 25 percent of people. The Phase 2b study was conducted in sub-Saharan Africa beginning in November 2017 and had enrolled 2,637 women participants between the ages of 18 and 35. Women are at much higher risk of HIV infection in this region.
During trials like this one, people receive the vaccine or placebo and then go about their lives. The researchers determine how effective the vaccine is by comparing how many people are infected with the virus in the two groups after a certain period of time. If no one in the vaccinated group becomes infected while people in the placebo group do, the vaccine is effective. In the case of this trial, the participants were evaluated from one month after the third vaccine dose, which was month seven, until month 24. There were no adverse effects from the vaccine. But during the trial, 63 volunteers who got the placebo and 51 participants who got the vaccine ended up acquiring an HIV infection.
The researchers are going to continue to follow up on the volunteers. The participants that tested positive for HIV have been offered medical treatment.
The vaccine that was tested in the Imbokodo trial, also called HVTN 705/HPX2008, is based on different pieces of many HIV viruses that are meant to stimulate an immune response. This so-called mosaic vaccine uses immune-stimulating antigens that are derived from different HIV genes from different strains of the virus. This vaccine also used an engineered strain of common cold virus that does not make people sick to deliver the mosaic antigens. Previous research suggested that this quadrivalent vaccine was able to induce an immune response.
Four doses of the experimental vaccine were given to the volunteers over one year, and the last two doses were also administered with a protein made by HIV, which is meant to boost the immune response, called an adjuvant. Participants were also given prophylactic HIV medication to prevent infection. Nonetheless, HIV infections occurred.
“The development of a safe and effective vaccine to prevent HIV infection has proven to be a formidable scientific challenge,” said NIAID Director Anthony S. Fauci, M.D. “Although this is certainly not the study outcome for which we had hoped, we must apply the knowledge learned from the Imbokodo trial and continue our efforts to find a vaccine that will be protective against HIV.”
An international team of researchers worked to develop this vaccine and roll out the trial. An independent review of this work and the trial has concluded that another Phase 3 study of an HIV vaccine called Mosaico (HVTN 706/HPX3002) will be going ahead. That study will be assessing vaccine efficacy in transgender populations and men in the Americas and Europe, and is expected to end in 2024.
Sources: Nature Medicine, NIH/National Institute of Allergy and Infectious Diseases (NIAID)