A Virus is Used to Cure Patient's Persistent Antibiotic-Resistant Infection
Antibiotic-resistant infections pose a serious threat to human health, which is expected to get worse. Bacterial infections can be particularly deadly when they form a biofilm, a slimy and tenacious community of microbes that can grow on surfaces including surgical implants. Biofilms are also often especially resistant to antibiotics, and many can withstand multiple drugs. Persister cells can also grow within a biofilm; they can lie dormant until the threat from antibiotics passes, then regrow again when the coast is clear.
While efforts are being made to develop new antibiotics, researchers, and in some cases, clinicians, have begun to consider an alternative, called bacteriophages, which are viruses that infect bacteria, and can destroy bacterial cells. Before the discovery of antibiotics, scientists knew bacteriophages could be a way to eliminate bacteria, but with the development of antimicrobial drugs, they were not needed. Now that many antibiotics have begun to fail to treat some infections, there is renewed interest in bacteriophages as a therapeutic.
There have been several instances in which clinicians reached a dead end in their treatment approach, and bacteriophages were applied successfully. Researchers and clinicians have now reported another case like that in Nature Communications.
A 30-year-old woman was catastrophically injured in a suicide bombing that occurred at the Brussels Airport on March 22, 2016. To treat the traumatic injuries, doctors had to perform a variety of procedures including a partial leg amputation. To reduce bacterial infection, the patient also took several different courses of antibiotics for over 700 days, which had nasty side effects.
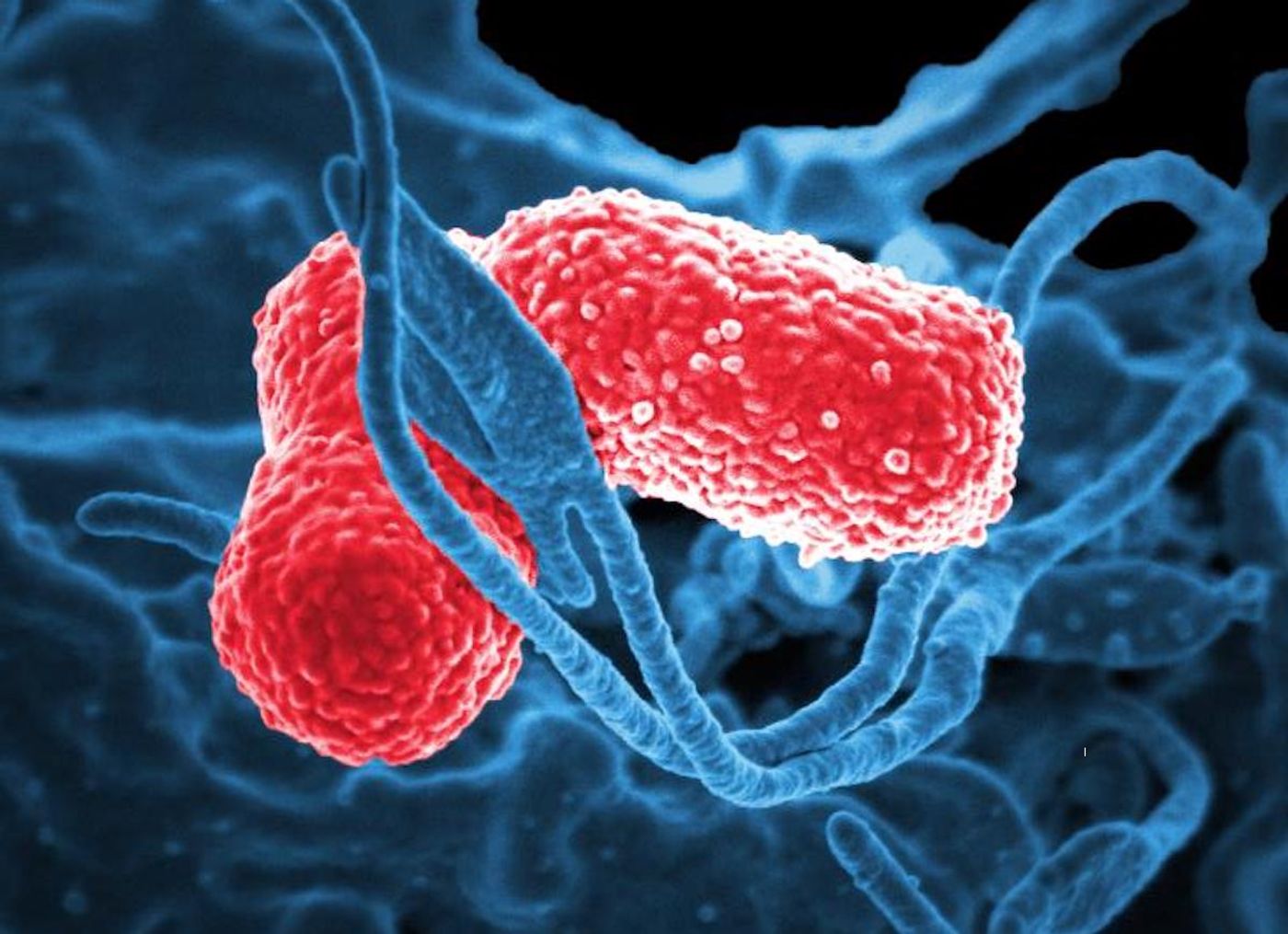
Ultimately, the antibiotics were not working on their own, and the patient had to be treated with bacteriophages that had been selectively grown. This was done by combining a bacteriophage selected from a library of known bacteriophages, and growing it with the microbes that were causing the patient's infection. In this case, Klebsiella pneumoniae were to blame. As the bacteriophage infected the K. pneumoniae cells from the patient, it picked up new mutations that made it even better at destroying the pathogenic bacteria. The most efficient bacteriophages were identified in growth cultures, and then they were isolated. This evolved bacteriophage was used as a treatment, combined with more antibiotics. When applied directly to the patient's infection during a surgical procedure, followed by delivery through a catheter, the infection was finally eliminated entirely.
Infections that affect fractures are known to be problematic because of multi-drug resistance. When fracture-related infections (FRI) are caused by MDR bacteria, clinicians are posed with a serious challenge. Patients often have to take high doses of antibiotics, which can cause problems of their own and don't always work.
This study suggests that bacteriophages might be applied in more cases like this in the future, and that they can work well against MDR pathogens when used in combination with antibiotics.
Three years after this treatment, the patient has reportedly regained mobility with the aid of crutches, and is able to get around on a bicycle.
Sources: Live Science, Nature Communications