Phase 2 Trial Shows Good Bacteria Can Stamp Out Bad Bacteria
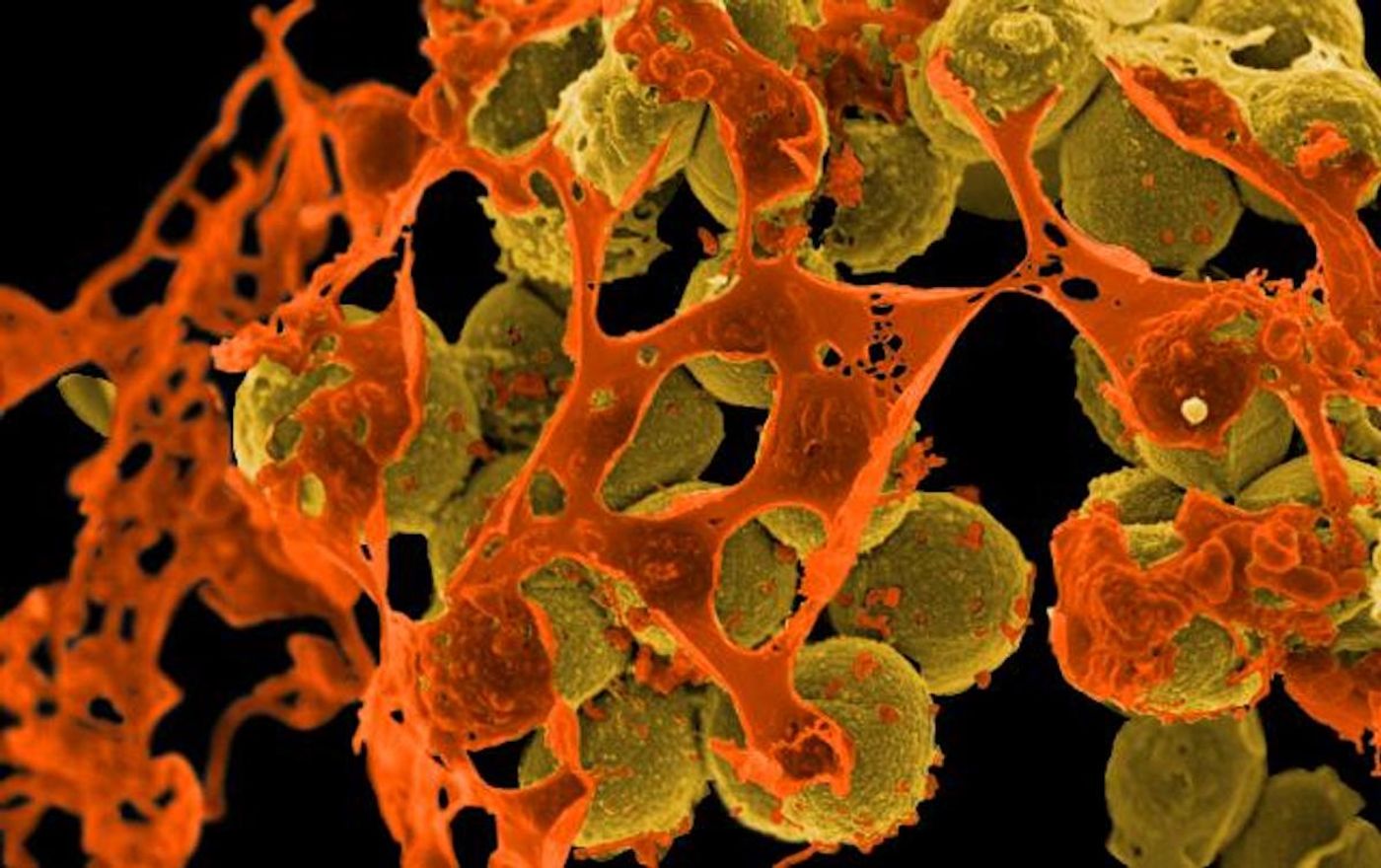
We share the world and our bodies with bacteria. Many of those microbes are harmless or even beneficial, while some can pose a threat to our health. Staphylococcus aureus is one microbe that may often be found on or around humans without posing a problem, while some strains of the bacterium, including methicillin-resistant S. aureus, or MRSA can cause serious infections in the skin, lungs, or blood.
Eliminating harmful strains of S. aureus can pose a major challenge; doing so may require large amounts of antibiotics that wipe out many other microbes, for example. Some topical antibiotics can get rid of S. aureus skin infections, but infections in other areas can be much harder to remove. Probiotics, or other live microbes may be a promising option.
Bacillus bacteria can be taken orally as spores, which withstand the rough trip through the human stomach to eventually colonize the intestine. There, Bacillus can thrive and tamp down the growth of potentially pathogenic microbes.
Scientists have completed a Phase 2 clinical trial of probiotics, finding that Bacillus subtilis significantly decreased the growth of S. aureus in human volunteers without disrupting the gut microbiome. The findings have been reported in The Lancet Microbe. This study also revealed that hybrid peptide-lipid molecules produced by bacteria, lipopeptides called fengycins, can disrupt S. aureus and halt its proliferation.
In this trial, 115 healthy people who naturally carried S. aureus at the start of the study were split in two groups; 55 individuals took the B. subtilis probiotic once a day for four weeks; while a placebo was given to 60 people. After four weeks, the researchers found that S. aureus levels had decreased by 96.8 percent in the stool samples and 65.4 percent in nose samples of the people who took probiotics, while there were no changes in S. aureus levels in the placebo group.
“The probiotic we use does not kill S. aureus, but it specifically and strongly diminishes its capacity to colonize,” said study leader Michael Otto, Ph.D., an NIH senior investigator at the National Institute of Allergy and Infectious Diseases (NIAID). “We think we can target the bad S. aureus while leaving the composition of the microbiota intact.”
The work also showed that there tends to be far more S. aureus bacteria in the gut compared to the the nose. However, staph infection prevention is often focused on the nose, so this research has suggested that gut S. aureus levels may be more relevant.
“Our results suggest a way to safely and effectively reduce the total number of colonizing S. aureus and also call for a categorical rethinking of what we learned in textbooks about S. aureus colonization of the human body,” said Otto.
The investigators are planning to repeat this work with a larger group of study volunteers to confirm the findings and learn more.
Sources: National Institutes of Health (NIH), The Lancet Microbe