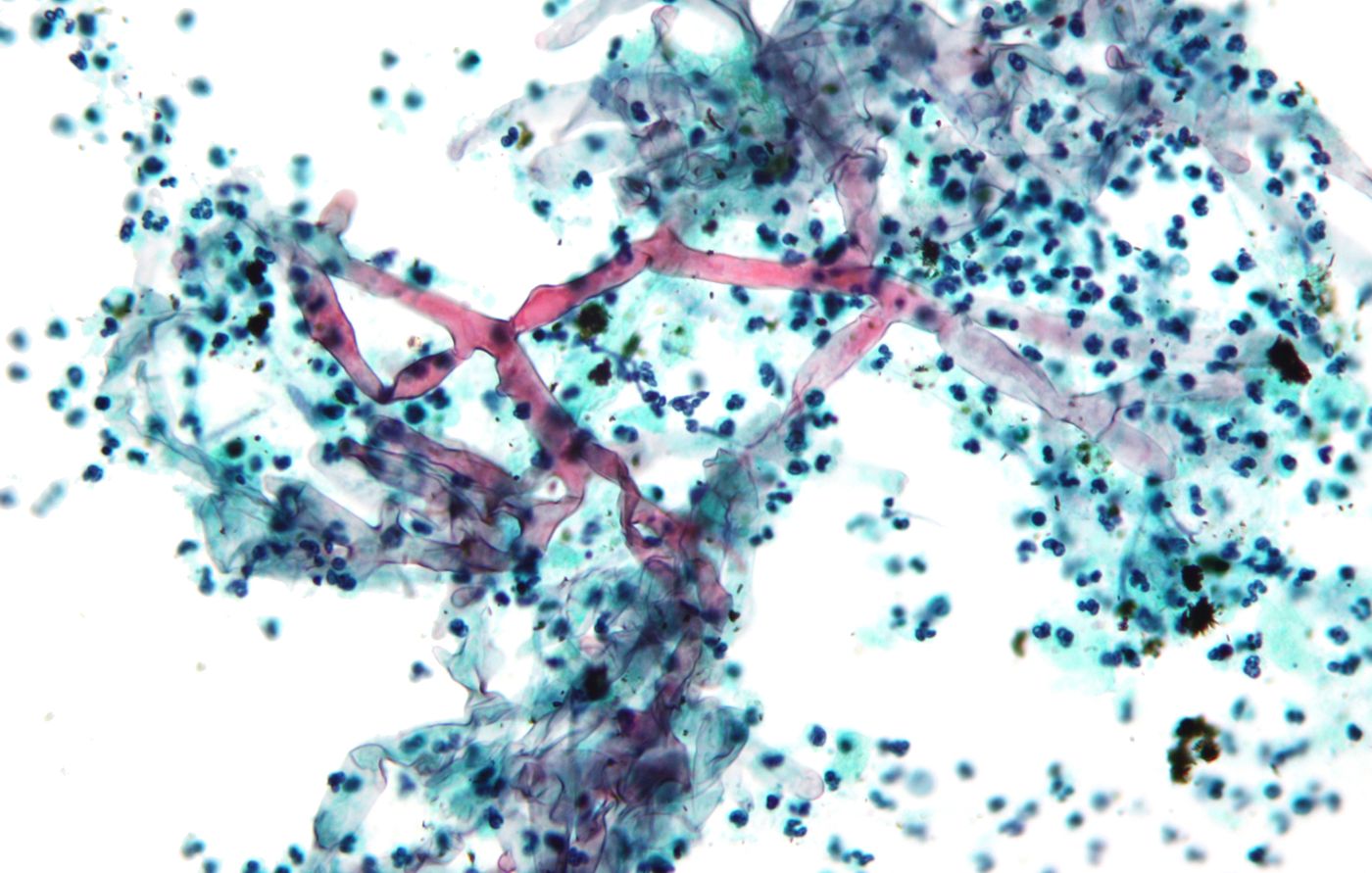
Fungal infections, often thought of as minor issues that are easily treatable, can actually be deadly for vulnerable people such as hospital patients. Some estimates suggest that tens of thousands of people die every year under such circumstances. Recent work in the field indicates that soldiers that had been wounded in Iraq and Afghanistan were sometimes killed by untreatable infections that originated from fungal microbes that penetrated deep into their tissues.
New work done by researchers at the University of Maryland School of Medicine has given us some new insights into one of these infectious microbes, Mucorales fungi, which is able to cause fatal infections. That infection is called mucormycosis (though it was previously called zygomycosis). It is a rare but serious illness and can result in a variety of symptoms depending on where on or in the body the infection is occurring.
The fungus typically attacks the cells of people with weakened immune systems, such as people with diabetes, anyone who has undergone a recent transplant or who has wounds. Other than the wounded soldiers, doctors have seen the fungal infection in some patients that were injured in the powerful 2004 tsunami in Indonesia as well as the tornadoes that devastated Joplin, Missouri, in 2011.
The
new study, published in the journal Nature Communications, characterized several important features of the Mucorales fungus that could aid researchers in the development of treatments. Currently, there is no way to treat these fungal infections.
"I think this work is going to provide a significant resource for future fungal research," said Vincent Bruno, Assistant Professor of Microbiology and Immunology at the University of Maryland School of Medicine, a research scientist at the Institute for Genome Sciences (IGS), and a co-author of the study. "Now we can dig into the data to find new targets for treatment."
Dr. Bruno and his colleagues compared the genes of 25 species of Mucorales fungus out of 50 to 100 total. Their data allowed them to find several cellular pathways that mucormycosis uses to grow in a patient. Apparently, these fungi are less able to invade human cells after a protein called platelet-derived growth factor receptor (PGDFR) is inhibited. That molecule is normally involved in cell growth.
It was also observed that all of the mucormycosis-causing fungi that were tested carried several copies of a gene that’s been implicated in host invasion.
Although these types of infections are thought to be rare, Dr. Bruno suggests they are probably underreported and frequently overlooked, meaning they could be far more common than previously realized.
"There are no vaccines or effective therapies available today to halt the highly fatal mucormycosis infection," said Ashraf S. Ibrahim, a scientist at a nonprofit independent biomedical research institute in Los Angeles – LA BioMed and another author of the work. "There is an urgent need for additional research to develop strategies to protect patients with weakened immune systems."
Dr. Bruno and Dr. Ibrahim now want to target PGDFR as a potential treatment. They may even be existing drugs that have already been approved by the FDA that can inhibit PGDFR effectively. If so, the path to a treatment for these fungal infections could be straightforward. Check out the video below to learn more about Mucor fungi and mucormycosis.
Sources:
CDC,
AAAS/Eurekalert! via
University of Maryland,
Nature Communications