Dysbiosis refers to an imbalance in the microbiome associated with the loss of good microbes that promote health, and an increase in the amount of pathogenic bacteria. It’s been postulated that serious illness correlates with such a dysbiosis, which induces susceptibility to hospital-acquired infections that can lead to sepsis and organ failure. As such, an understanding of how the microbiome is affected by hospital admission is critical.
A
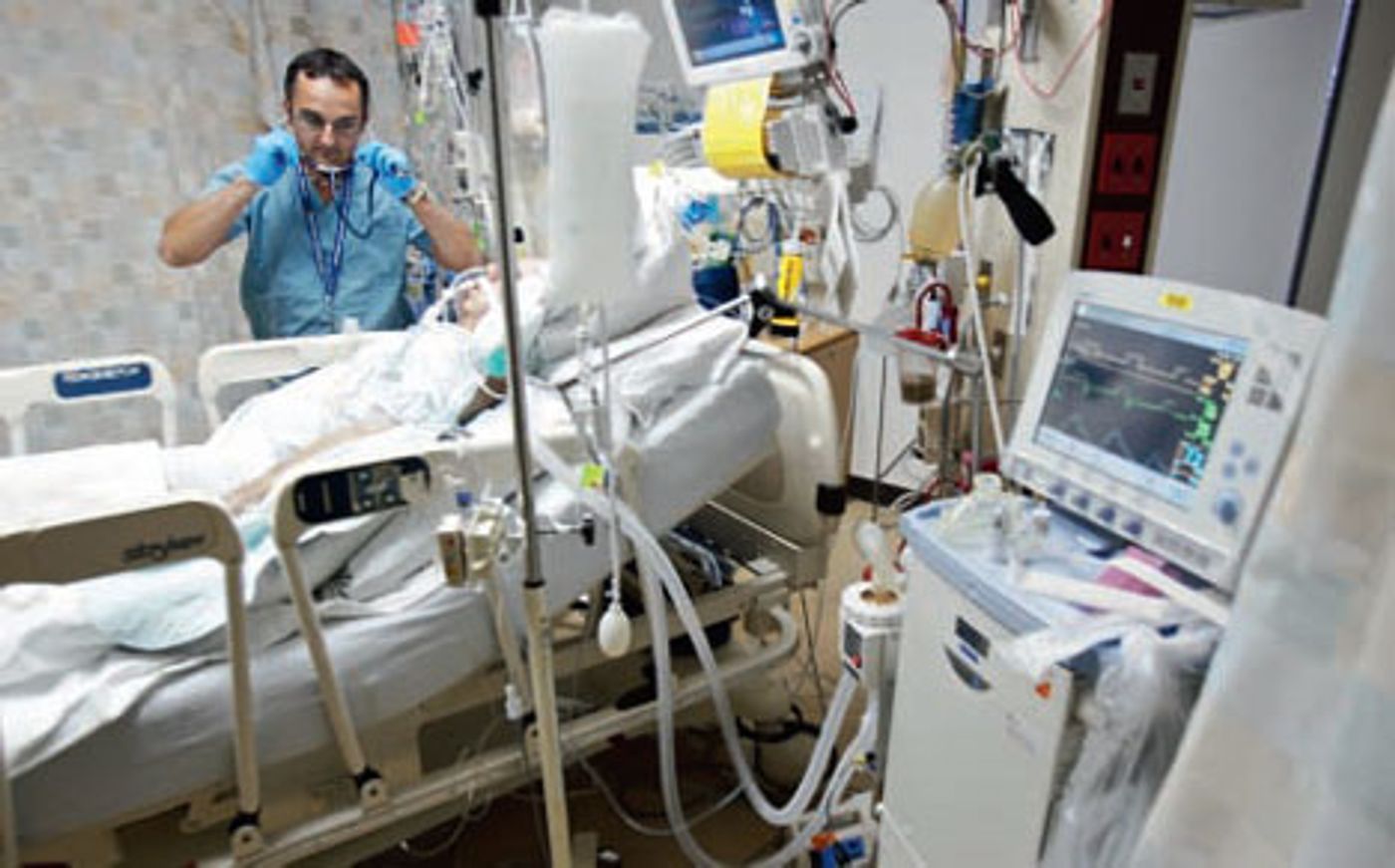
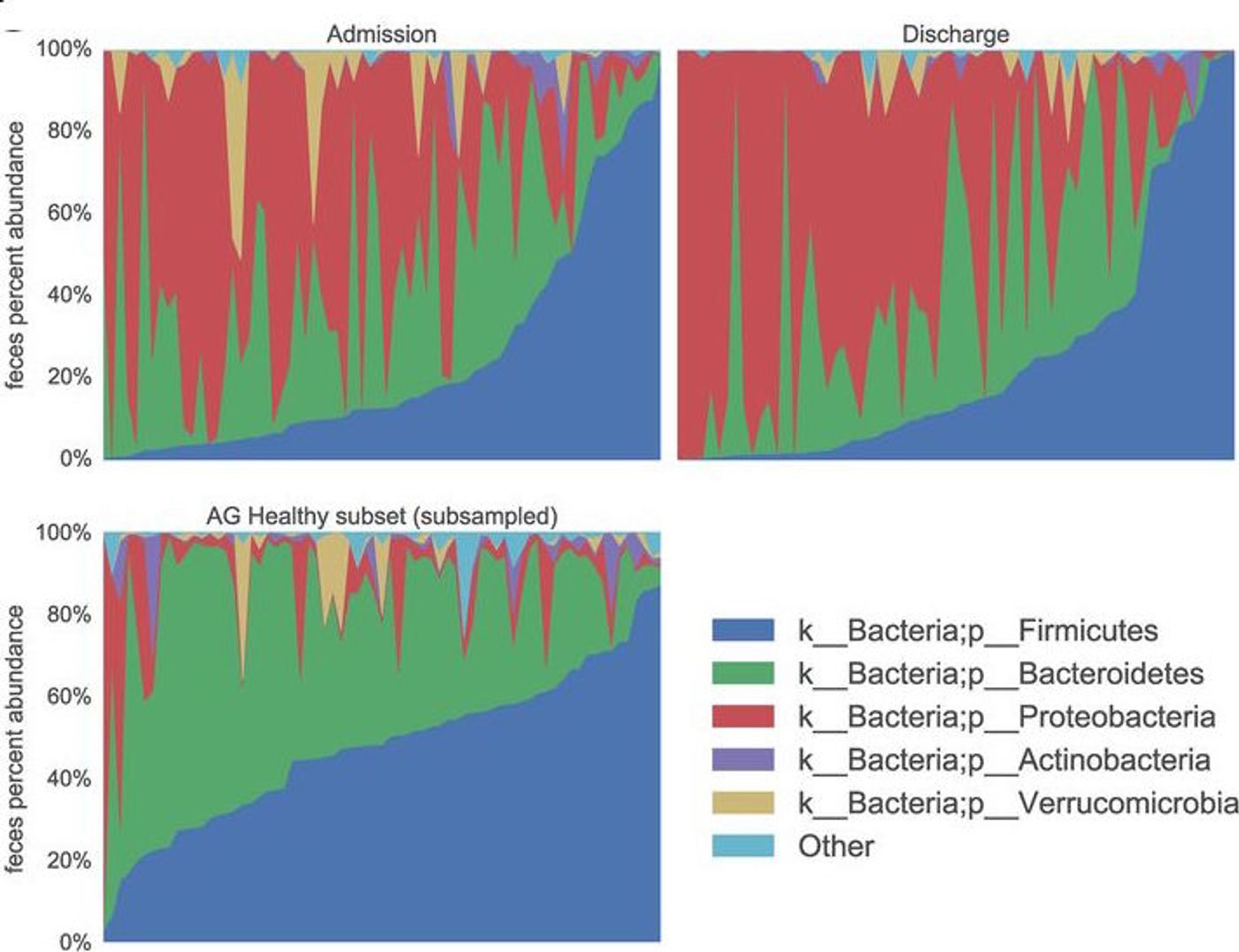
new study published in the journal mSphere outlines research that compared the microbiome of healthy people to that of those admitted to the ICU. It found dramatic differences, with dysbiosis occurring in the gut, mouth and skin microbiomes of ICU patients. That bacterial imbalance only got worse along with the length of the hospital stay. The ICU patients lost the commensal, good bacteria, and displayed larger counts of bacteria taxa that have pathogenic strains. This would likely cause a vulnerability to infection that under such circumstances would only be dangerous to the patient.
"The results were what we feared them to be," said study leader Paul Wischmeyer, an anesthesiologist at the University of Colorado School of Medicine. "We saw a massive depletion of normal, health-promoting species."
Exactly what constitutes a healthy gut microbiome is still not well defined. This work however, should help characterize what we would expect one to look like.
While other studies have analyzed the microbiome of individuals or small sets of critically ill patients, this study used oral, skin and stool samples from 115 patients in ICUs across four hospitals in both the United States and Canada. There were two sets of samples taken; one at 48 hours after admission and again after spending 10 days in the ICU, or at discharge.
The researchers also looked at what the sources of the bacteria were using a tool called SourceTracker. (Which you can check out
here.) What they found was unexpected, for example, at admission one adult fecal sample resembled that of a decomposing corpse. "That happened in more people than we would like to have seen," Wischmeyer commented.
Of the samples taken, fecal and oral samples were more similar to each other at admission than they were at discharge, which the researchers suggest is because the time spent in the hospital disrupts the microbial communities.
The speed of change in the patients’ microbiomes surprised Wischmeyer. "We saw the rapid rise of organisms clearly associated with disease," he explained. "In some cases, those organisms became 95 percent of the entire gut flora - all made up of one pathogenic taxa - within days of admission to the ICU. That was really striking."
The investigators say their study has indicated the microbiome could be monitored in critical care patients, and would be a helpful tool in aiding their treatment and recovery. Wischmeyer hopes to find treatments (such as fecal transplants) that would be suitable for patients with dysbiosis.
The video above is a recent interview with John Alverdy, MD, Professor of Surgery at The University of Chicago that discusses what hospital stays can do to the microbiome. Click on the details of the video for the time of various highlights.
Sources:
AAAS/Eurekalert! via
American Society for Microbiology,
mSphere