The Centers for Disease Control and Prevention estimates that every day, roughly one of 25 hospital patients carries at least one healthcare-associated infection. Those types of infections are referred to as nosocomial infections, and they are a serious and preventable problem. While the rate of their occurrence decreased in the past few years, there were still over 700,000 various infections that happened in acute care centers in the United States in 2011.
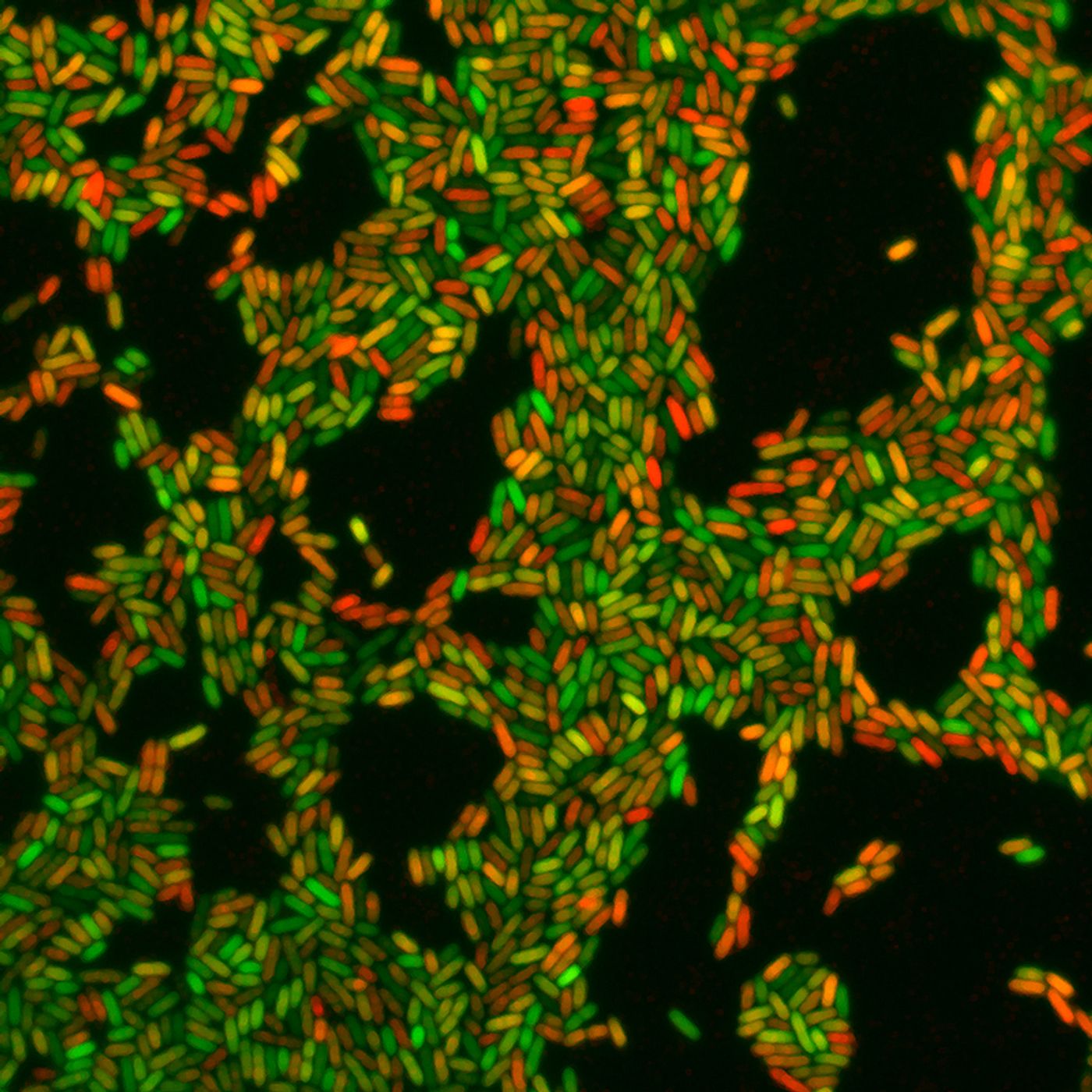
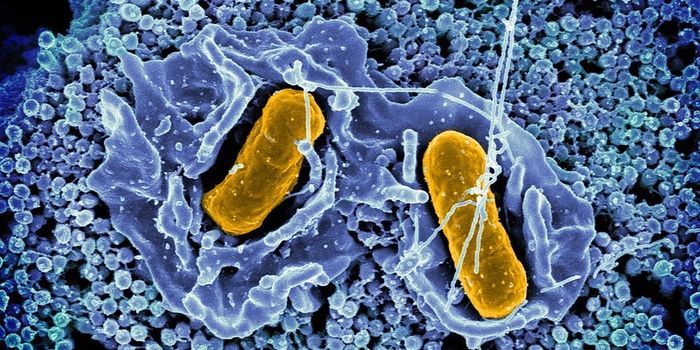
For nosocomial infections, about ten percent were caused by the pathogenic bacterium Pseudomonas aeruginosa, which often results in pneumonia. The microbe causes a range of illnesses but is the primary cause of chronic lung infections in patients with vulnerable immune systems. P. aeruginosa is also resistant to a multitude of antibiotics.
Reporting in Nature Microbiology, researchers at the Biozentrum of the University of Basel have found that calcium moves P. aeruginosa infections from an acute to a chronic state. Additionally, they’ve learned why the pathogen is more difficult to treat once it becomes chronic.
When pneumonia is in the early, acute phase, it produces molecules that help it establish an infection – virulence factors – which allow it colonize a host while evading and suppressing the host’s immune system. Those virulence factors are no longer produced once the infection switches to the chronic stage. The growth rate of the bacterium then slows and it begins to produce a protective matrix. The research team, led by Professor Urs Jenal, an infection biologist at the Biozentrum of the University of Basel, has reported that calcium initiates the virulence to switch from acute to chronic.
"In Pseudomonas a central signaling pathway senses environmental information and ultimately determines whether the pathogen will undergo the acute to chronic virulence switch," explained Jenal. "Although the components of this pathway are well-known, none of the external signals modulating the switch are defined."
The investigators discovered that the bacterial cell envelope carries a receptor that monitors the calcium level in the environment and communicates the information to the cell. Elevated calcium levels result in a switch to a chronic program. After chronic virulence sets in, the bacteria use a biofilm structure to protect themselves and slow down growth. The reduction in their growth rate allows them to tolerate drug treatments, making them persistent.
The scientists also assayed clinical samples of cystic fibrosis patients, who often develop chronic and lifelong lung infections caused by P. aeruginosa, resulting in permanent damage to their lung tissue.
"Most of the isolates from airways of CF patients have retained their calcium sensitivity," said Jenal. "We believe that this allows these bacteria to constantly adapt their virulence in response to the often changing conditions in the airways. One of the characteristics of cystic fibrosis is deregulated calcium homeostasis. We assume that elevated calcium levels in patients promote the switch from an acute to a chronic state of infection. This is of advantage for the pathogen, as it may ensure its long-term survival in the respiratory tract. At the same time, treatment of chronically infected patients becomes more challenging."
The video above has more information about P. aeruginosa. If you'd like to know more about nosocomial infections, check out the short video below from the CDC.
Sources:
CDC,
Phys.org via
University of Basel,
Nature Microbiology