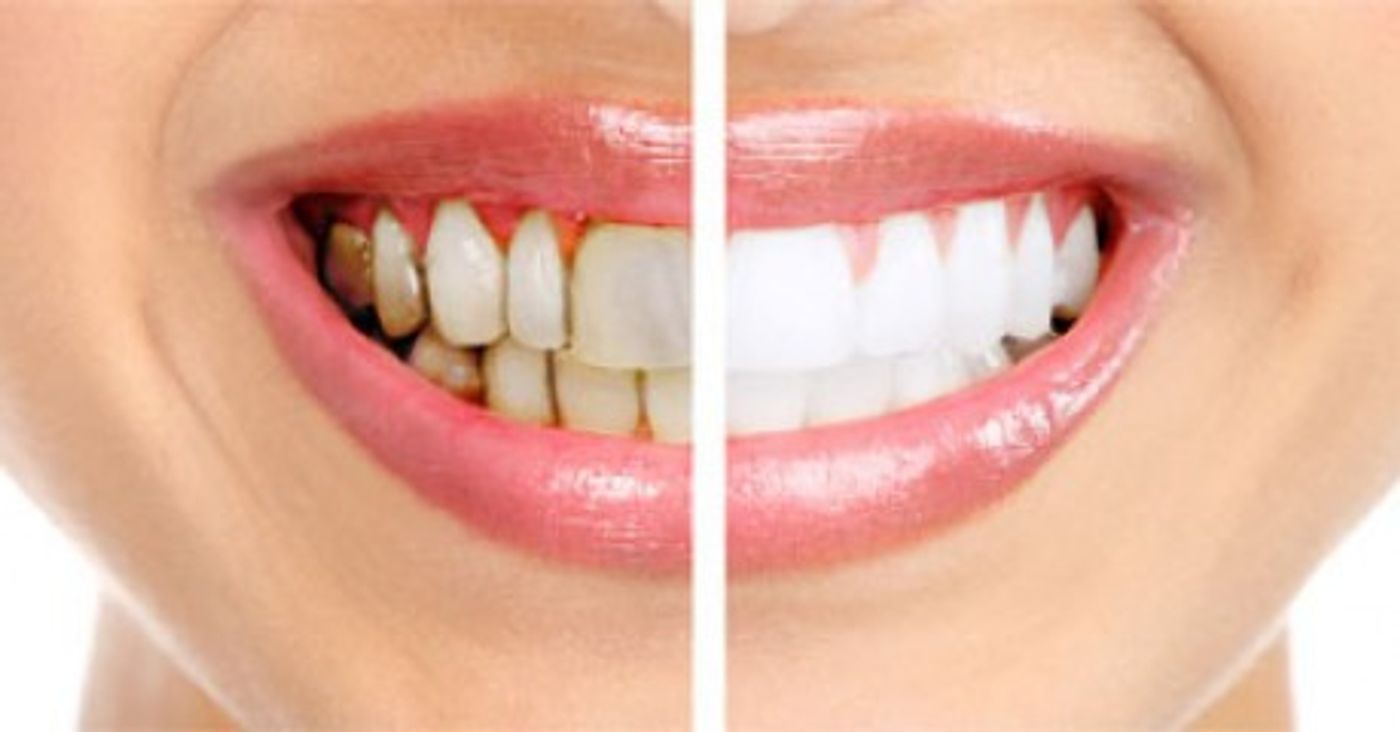
Nobody likes going to the dentist, but most of us do it anyway. Why? Because regular dental care helps prevent things like cavities and gum disease.
There are many species of bacteria in your mouth, around 700, and 500 or more make their home in dental plaque! Your mouth is an ideal place for bacteria to grow - the temperature is pretty constant, the pH is rather neutral, and saliva contains all sorts of goodies. Besides bacteria, there’s an array of other lifeforms in your mouth, including fungi, viruses, and even protozoa! Keeping on the topic of bacteria - one species that resides in your mouth is Porphyromonas gingivalis, the bacterium responsible for gum disease (chronic
periodontitis, to be exact).
The presence of P. gingivalis and other dental pathogens isn’t enough to incite disease, however. When the oral microbiome is appropriately balanced, no disease is present. The problems occur when the microbiome is somehow disturbed - that’s when we get cavities and gum disease.
Gum disease is the name given to a range of oral inflammatory infections. Mild inflammation, known as gingivitis, is often reversible, but chronic infections can destroy connective tissue and cause people to lose teeth. A 2012 study by the World Health Organization reported that 10-15% of the world’s adults have some form of gum disease.
Gum disease tends to be more prevalent in people with diabetes, leukemia, AIDS, and Down’s syndrome. The condition may also increase your risk for heart attack, stroke, and diabetes. As an interesting side note, S. mutans, a bacterium responsible for dental cavities, is also commonly found infecting heart tissues and may promote atherogenic plaque formation.
Back to the topic at hand. P. gingivalis is a Gram-negative anaerobe that has a black pigment to it (which I think is pretty neat). P. gingivalis, along with Tannerella forsythia and Treponema denticola, make up the “red complex”, a group of bacteria associated with severe gum disease. (If anyone knows why it’s called the “red” complex, I’d love to know!)

P. gingivalis produces a number of virulence factors that contribute to the pathogenesis of gum disease. Most strains produce a capsule, and the composition varies from strain to strain. In each case, the capsule seems to help the cells adhere to the teeth and gums. On the whole, strains that make a capsule tend to be more virulent, probably because they literally hide bacterial surface components from the host’s immune system. P. gingivalis can also live inside gingival fibroblasts, and in some cases the capsule can hinder its invasion of fibroblasts. On the other hand, the capsule seems to keep the fibroblasts from producing immunomodulating cytokines like IL-1, IL-6, and IL-8.
P. gingivalis also produces proteases, and these are divided into two distinct families - cysteine proteases and serine proteases. These enzymes are also known as “gingipains” and are secreted by P. gingivalis into the environment (your mouth!). Gingipains degrade periodontal tissue by breaking down collagen and other extracellular matrix proteins; they also deactivate host protease inhibitors and deregulate the host inflammatory response by degrading antimicrobial peptides and the T cell receptors CD4 and CD8.
Finally, like most all Gram-negative bacteria, P. gingivalis produces LPS. There’s evidence that LPS keeps gingival epithelial cells from secreting IL-8 - this chemokine is required to activate other immune cells, including neutrophils, basophils, and eosinophils. Without it, “chemokine paralysis” occurs, allowing the bacteria to proliferate and avoid killing.
There’s a promising new therapeutic on the horizon, however. Researchers at the University of Melbourne recently tested a P. gingivalis vaccine in mice. In their study, published in the Nature partner journal Vaccines, the group developed a vaccine consisting of a chimeric gingipain antigen. In a mouse model of periodontitis, the vaccine protected the animals from bone resorption through the production of a Th2 response and the production of gingipain-specific antibodies.
Sources: Frontiers in Microbiology,
Vaccines,
Mayo Clinic,
Infection and Immunity, Wikipedia