Worms Developed as Research Model for Microbiome & Disease
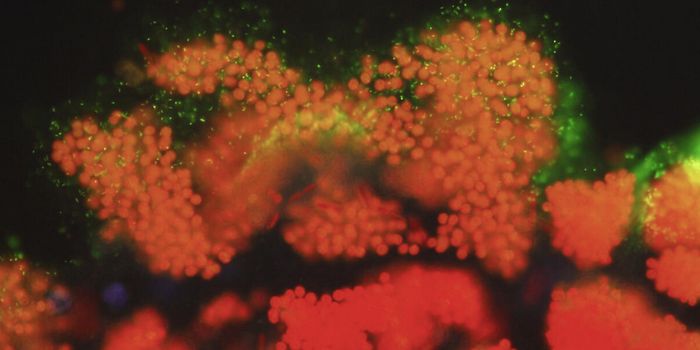
A vast community of microbes lives in symbiosis with the human body, many of which reside in the gastrointestinal tract. As scientists have learned more about that community - the gut microbiome - since the advent of high-throughput genetic technologies, it has become clear that human health is impacted by the microbiome in many different ways. The gut appears to be especially influential on some diseases like diabetes and autoimmune disorders, but exactly how it’s all working, or failing, is still not understood well. Researchers at the Buck Institute have now developed Caenorhabditis elegans, a roundworm commonly used in biomedical research and briefly introduced below, as a model for researching how bacteria in the microbiome are communicating and interacting with their host, regardless of the host’s species.
Publishing in Scientific Reports, the researchers have shown how it is genes, and not the metabolites, of bacteria that are affecting the physiology of the worms that consume them.
"The dynamic nature of the gut microbial community has proven hard to study in mice and even harder in human subjects," said the senior author of the work, Pankaj Kapahi, a Buck Professor. Worms typically eat bacteria in their diet, and the research team thought they’d make an ideal way to untangle some of the parts of the complex body-microbiome interactions. "We have uncovered the effects of bacterial genetics on the physiology of a simple organism, which may serve as a model system to study the gut microbiome in mammals to identify novel therapeutics to treat diseases," he explained.
"Humans have a gut full of bacteria that are 'talking' with intestinal cells and ultimately affect the whole organism, so there has been a lot of research targeting bacterial metabolites associated with human disease. This study is the first one to explore how the bacteria themselves talk to the host," commented Amit Khanna, a postdoctoral research fellow in Kapahi's lab.
Kapahi noted that while roundworms are quite different from humans, many of the basic molecular pathways in the biology of both organisms are similar, such as the insulin-like signaling pathway, a factor in human disease like type 2 diabetes and obesity.
Previous work by Kapahi looked at a phenomenon in the worm life cycle, dauer, in which worm larvae go into a sort of hibernation to survive a detrimental environment. Compounds made by bacteria the worm eats can affect whether it enters dauer; the insulin-like pathway is involved in controlling the process.
The researchers looked for bacterial genes in human gut microbes that could impact the insulin-like pathway in worms. Around 4,000 strains of E. coli were systematically mutated to knock out one gene at a time; their screen led them to determine that 56 genes enhance dauer formation. Interestingly, some of those single-gene knockouts extended lifespan.
Following up on their finding about lifespan extension, they learned that adenylate cyclase (cyaA) increased lifespan the most and modulates dauer formation by extering an effect on the TGF-beta signaling pathway. The researchers were able to see how the sensory neurons communicated with target cells, and which pathways control the dauer state.
"The idea that a single gene mutation - in the bacteria that the worms normally eat - could throw off an entire animal and send it into a dauer state was certainly not a concept that we anticipated when we began this study," said Kapahi.
The study shows how bacterial and worm genetics can be used to unravel the relationship between bacteria and host, and how it impacts physiological processes like aging and biological dysfunction.
"There a lot of studies showing that the microbiome influences this and that, but we have very little understanding of the mechanisms and how to make sense of the mounds of data," said Khanna. "We think our method might be the way forward: to be able to ask specific questions about what do individual bacterial components contribute and how do they do it."
The talk in the video above with Filomena Trindade, MD, (who was not part of this study) discusses how the microbiome impacts human conditions like type 2 diabetes and obesity.
Sources: AAAS/Eurekalert! via Buck Institute, Scientific Reports