New insights into gonorrhea
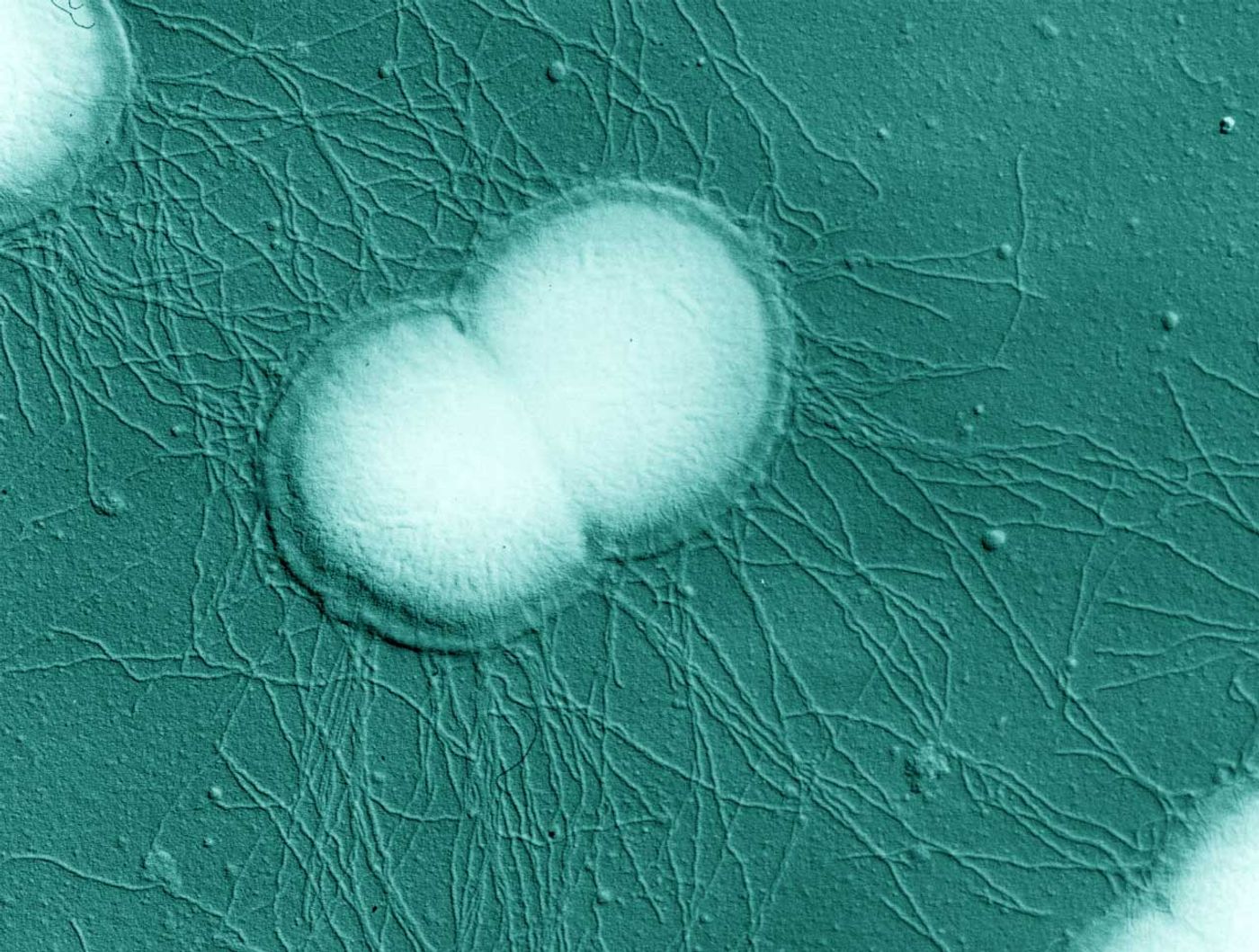
Researchers at the University of Maryland figured out why some Neisseria gonorrhoeae infections become invasive, while others don’t. More invasive strains cause the epithelial layer of the endocervix (in the female genital tract) to shed, giving the bacteria access to deeper tissues.
N. gonorrhoeae, as the name suggests, is the bacterium that causes gonorrhea. Gonorrhea is a common sexually transmitted infection, and it is becoming a serious public health issue because many strains of the bacterium are resistant to antibiotics.
Gonorrhea has been difficult to study because the bacteria only infect humans - this means that other animal models aren’t particularly useful (and no humans are volunteering as guinea pigs). Here, the University of Maryland researchers, led by Liang-Chun Wang, developed an explant culture model that uses human endocervical tissue.
The group found that the bacteria cause epithelial cells lining the endocervix to shed off. The bacteria also disrupt the junctions between epithelial cells by activating myosin. This is a pretty surprising finding because researchers have always thought that this “epithelial exfoliation” helped to prevent infection.
They started their experiments by testing out their new explant model and comparing it to a monolayer of T84 colonic epithelium cells. They incubated the two cell cultures with bacteria, and by 24 hours both cultures showed bacteria-induced exfoliation. Importantly, both the endocervical explants and the T84 cells behaved similarly, indicating that both models could be useful for studying gonorrhea.
Next, the researchers investigated the N. gonorrhoeae cell-surface protein called Opa because previous studies indicated that it is especially important for the pathogenesis of gonorrhea. Opa is also important because it undergoes phase variation - the bacteria only express it under certain environmental conditions.
They incubated the endocervical and T84 cells with a mutant strain of bacteria that did not produce Opa. Surprisingly, cells that lacked Opa showed more exfoliation in response to the bacteria. The percentage of exfoliation increased in the endocervical cells from 32.3% to 66.3% and in the T84 cells from 31.2% to 55.8%. Thus, it appears that cells that do not express Opa are able to establish a more productive infection (from the bacterial point of view, of course).
Their next goal was to better understand the mechanism behind the bacteria-induced epithelial exfoliation. They suspected that non-muscle myosin II was involved in the process and tested whether small chemical inhibitors of myosin affected bacteria-induced exfoliation. Sure enough, two of the inhibitors (one that inhibited calcium-dependent and another that inhibited ROCK-dependent myosin activation) reduced exfoliation.
Thus, N. gonorrhoeae activates myosin in host cells to induce exfoliation. This, along with the absence of Opa, allows the bacteria to produce a more invasive infection.
Sources: PLOS Pathogens, Science Daily