Shigella gets creative to survive the GI tract
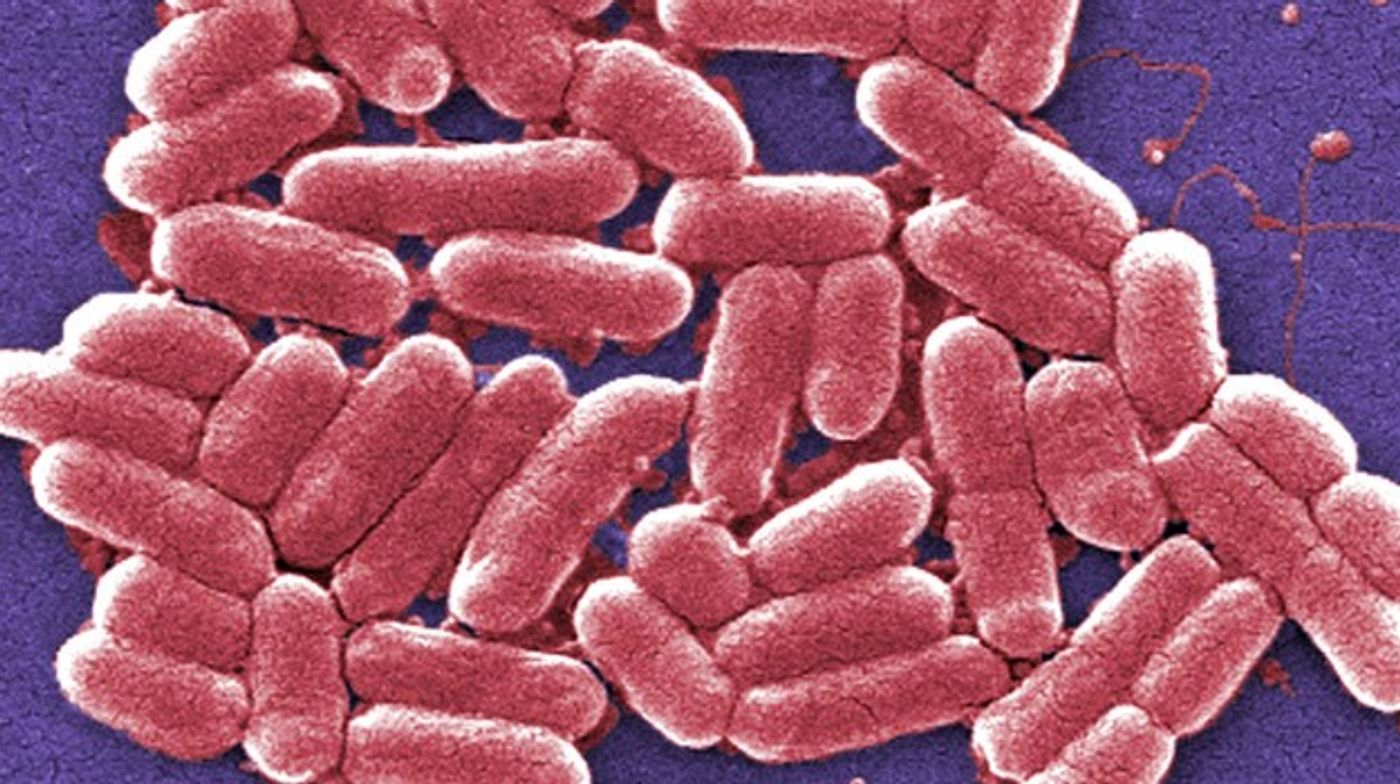
It’s a long, dangerous trip from the mouth to the colon. New research from Massachusetts General Hospital explain how Shigella makes the journey.
Shigella sickens some 80 million people worldwide each year, and about 700,000 die. Shigella can leave the survivors with many issues, including arthritis and kidney damage.
Bacteria that make it to the small intestine are exposed to bile - a digestive juice made up of proteins, carbohydrates lipids, mineral salts, and vitamins. Bile kills most bacteria - except Shigella (and E. coli, Salmonella, and Vibrio).
According to study author Christina S. Faherty, “we analyzed how the pathogen's gene expression changes in response to bile salts exposure. The changes we identified pointed to the use of antibiotic resistance mechanisms to resist bile, to the development of a more infectious organism through increased virulence gene expression, and to one better able to survive the colonic environment due to additional gene expression changes.”
The researchers found that exposure to bile salts causes Shigella to form biofilms. The cells formed visible aggregates in culture and produced extracellular polymeric substances (EPS, detected with concanavalin A staining). The production of EPS required not only bile salts, but also glucose, and removing the bile salts caused the biofilms to disperse.
Next, they investigated whether there were changes in gene expression when Shigella was exposed to bile salts. Ninety-six genes were differentially expressed when the bacteria were cultured in the presence of bile salts. For example, exposure to bile salts induced the expression of genes for central metabolism, sugar transport, drug resistance, and virulence.
To verify these results, the researchers grew acrB or galU mutants with bile salts. AcrB is a component of the AcrAB multidrug efflux pump, and GalU is required to produce O-antigen, a component of lipopolysaccharide. As expected, neither mutant was able to grow in the presence of bile salts.
The researchers hypothesize that when Shigella encounters bile in the upper small intestine, the cells form a biofilm. However, when the bile is reabsorbed in the lower small intestine, the biofilm is dispersed, allowing the bacteria to invade the colon and establish an infection.
Sources: Infection and Immunity, Science Daily