Ebola hides out in your eye
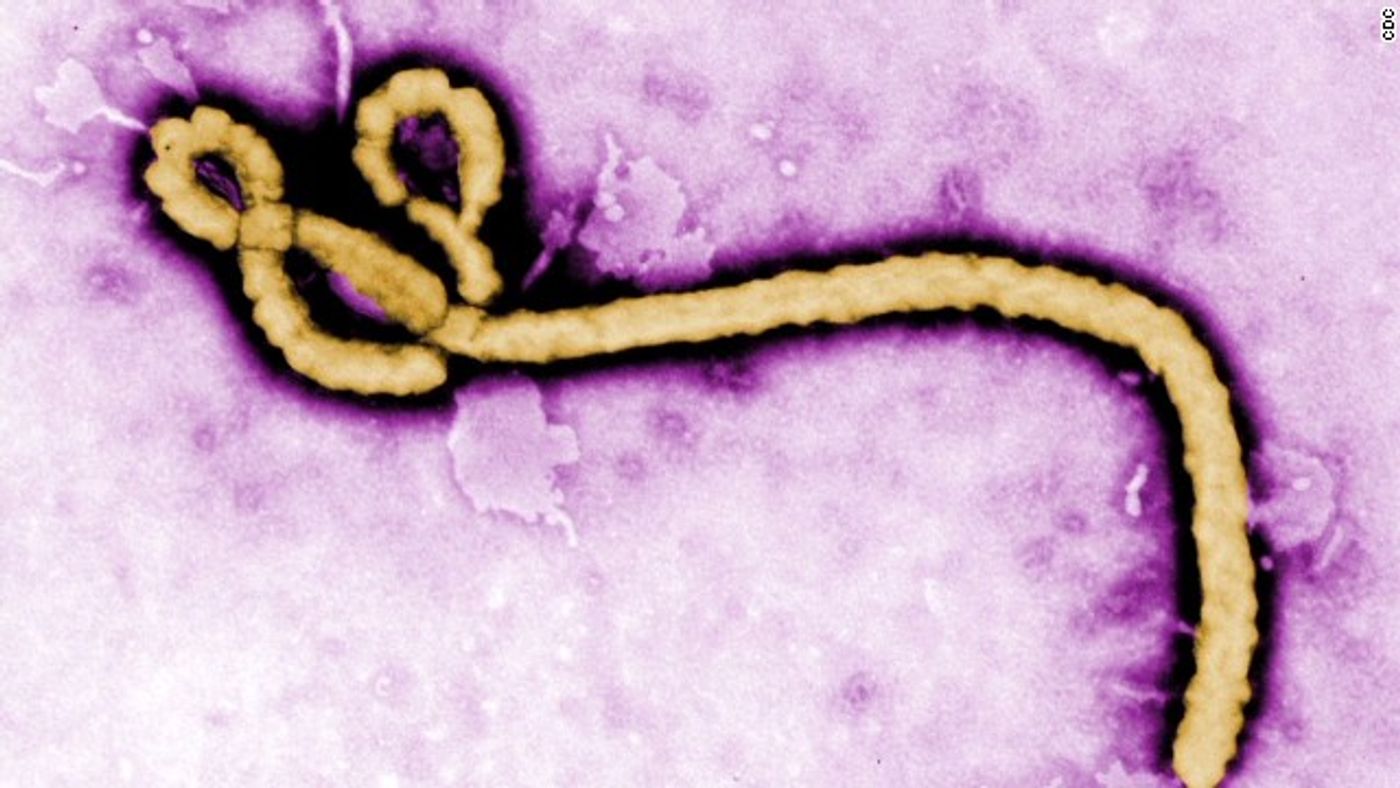
As if getting Ebola isn’t bad enough, some survivors continue to harbor the virus in their eyes.
Researchers at Flinders University School of Medicine in Adelaide, Australia, presented evidence that Ebola takes up residence in retinal pigment epithelial cells, causing chronic uveitis in Ebola survivors.
Image: CDC
The researchers knew that Ebola infection in the eye causes retinal scarring with both reduced and increased pigmentation. This suggested that Ebola may infect the retinal pigment epithelial cells. With this in mind, they determined if these cells could indeed support the growth of Ebola.
First, they inoculated cultures of retinal pigment epithelial (RPE) cells with Ebola and assayed the production of the viral nucleoprotein and the production of live progeny virus. Initially - after 4 hours - the RPE cells did not test positive for the viral nucleoprotein. However, by 24 hours, the nucleoprotein was evident in the RPE cells. They also calculated the TCID50 (tissue culture infective dose) for the progeny virus, and the data showed that viral titers increased from 24 to 72 hours after infection. Thus, Ebola readily infects RPE cells.
Next, they looked into the immune response of the RPE cells to Ebola. They performed RNA-seq on total RNA from the infected RPE cells to measure changes in gene expression. Overall, 1,060 genes were differentially expressed by the RPE cells in response to infection. The expression of 560 transcripts increased, while 500 decreased. The upregulated genes corresponded to those involved with type I IFN signaling and general antiviral responses.
The researchers confirmed their findings with RT-qPCR. Between 24 and 72 hours after infection, IFN-β expression increased significantly, as did the expression of several IFN-stimulated, antiviral genes.
At the same time, the RPE cells produced immunomodulatory molecules. These cells help make the eye an immune-privileged site - a site that can be exposed to numerous antigens without signaling an immune response. Ebola virus infection had little effect on the expression of 6 major immune modulators, such as IL-10 and macrophage migration inhibitory factor. However, the expression of PD-L1 and PD-L2 increased during the course of infection (up to 72 hours).
According to the authors, “our results and previous clinical observations suggest that retinal pigment epithelial cells may serve as one reservoir for EBOV within the eye. We speculate that infected cells activate the type I IFN response, which would limit spread of infection, but that these cells also restrict innate and adaptive immune responses, which otherwise would clear the virus from the eye. Ultimately, infected cells must mount a robust innate immune response that overwhelms ocular immune privilege, leading to clinical uveitis.”
Sources: Translational Vision Science & Technology and Science Daily