Cortisol may link gut microbes, brain
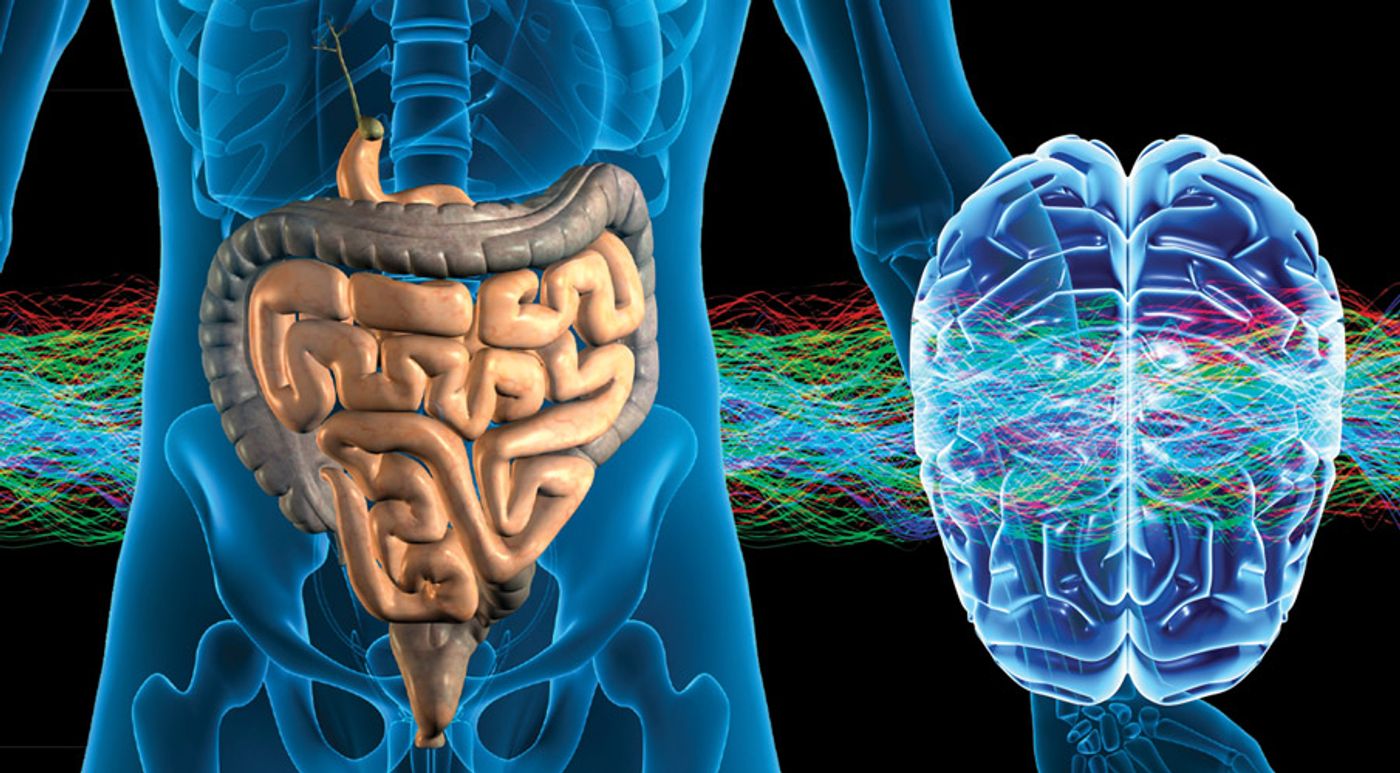
Your gut is a long way from your brain, but problems with your gut microbiome could lead to problems with your brain by disrupting the so-called microbiota-gut-brain axis.
Image: Soren Dreier
According to Austin Mudd, a researcher at the University of Illinois College of Agriculture, "changes in neurometabolites during infancy can have profound effects on brain development, and it is possible that the microbiome -- or collection of bacteria, fungi, and viruses inhabiting our gut -- plays a role in this process. However, it is unclear which specific gut bacteria are most influential during brain development and what factors, if any, might influence the relationship between the gut and the brain."
In a study published in the journal Gut Microbes, Mudd and colleagues used piglets to investigate the connection between neurometabolites and gut microbes.
Believe it or not, pigs are pretty good experimental surrogates for humans - their immune systems function similarly, and diseases progress in much the same way. For this study, they raised the piglets over 30 days on 2 different experimental diets.
At 30 days old, they underwent an MRI during which magnetic resonance spectroscopy (MRS) was performed. MRS was used to quantify neurometabolites in the hippocampus, including creatine, phosphocholine, myoinositol, and N-acetylaspartate.
At 31 days old, the piglets were euthanized, and various tissue samples were collected. Microbial DNA was also isolated from the colon, and different genera of bacteria were identified with 16S rRNA sequencing.
Once all the data were gathered, they crunched the numbers with some statistics (that I don’t pretend to understand) to identify relationships between specific bacteria and specific compounds in the brain and blood. It turned out that bacteria in the genera Bacteroides and Clostridium correlated directly with the concentration of myoinositol in the brain and Butyricimonas correlated with N-acetylaspartate (NAA). Conversely, Ruminococcus correlated indirectly with NAA in the brain. That is, more Ruminococcus in the gut meant less NAA in the brain.
NAA is made by mitochondria and is found in neurons, oligodendrocytes, and myelin. It functions as an osmolyte to balance fluid levels in the brain and is an important source of acetate for the synthesis of lipids and myelin.
Next, they ran a metabolomics analysis on blood samples to look for connections between the different bacteria and compounds in the blood. They found that Bacteroides correlated with a higher concentration of serotonin, and Ruminococcus correlated with a lower concentration of serotonin and cortisol. Because Ruminococcus was associated with both NAA and cortisol, they reasoned that there might be a mechanistic relationship between all 3.
They used mediation analysis (more confusing statistics) to look for such a relationship and found that, sure enough, serum cortisol mediated the relationship between NAA in the brain and Ruminococcus in the gut.
According to study author Ryan Dilger, “this mediation finding is interesting, in that it gives us insight into one way that the gut microbiota may be communicating with the brain. It can be used as a framework for developing future intervention studies which further support this proposed mechanism.”
Sources: Gut Microbes, Eurekalert, Wikipedia