Bacterial Species Found to Promote Colorectal Cancer and Chemotherapy Resistance
According to the American Cancer Society, colorectal cancer (CRC) is characterized by the unchecked division and survival of abnormal cells in the colon or rectum. The area of the intestines that make up the colon and the rectum are often referred to as the large intestine which functions to process food for energy and rid the body of solid waste.
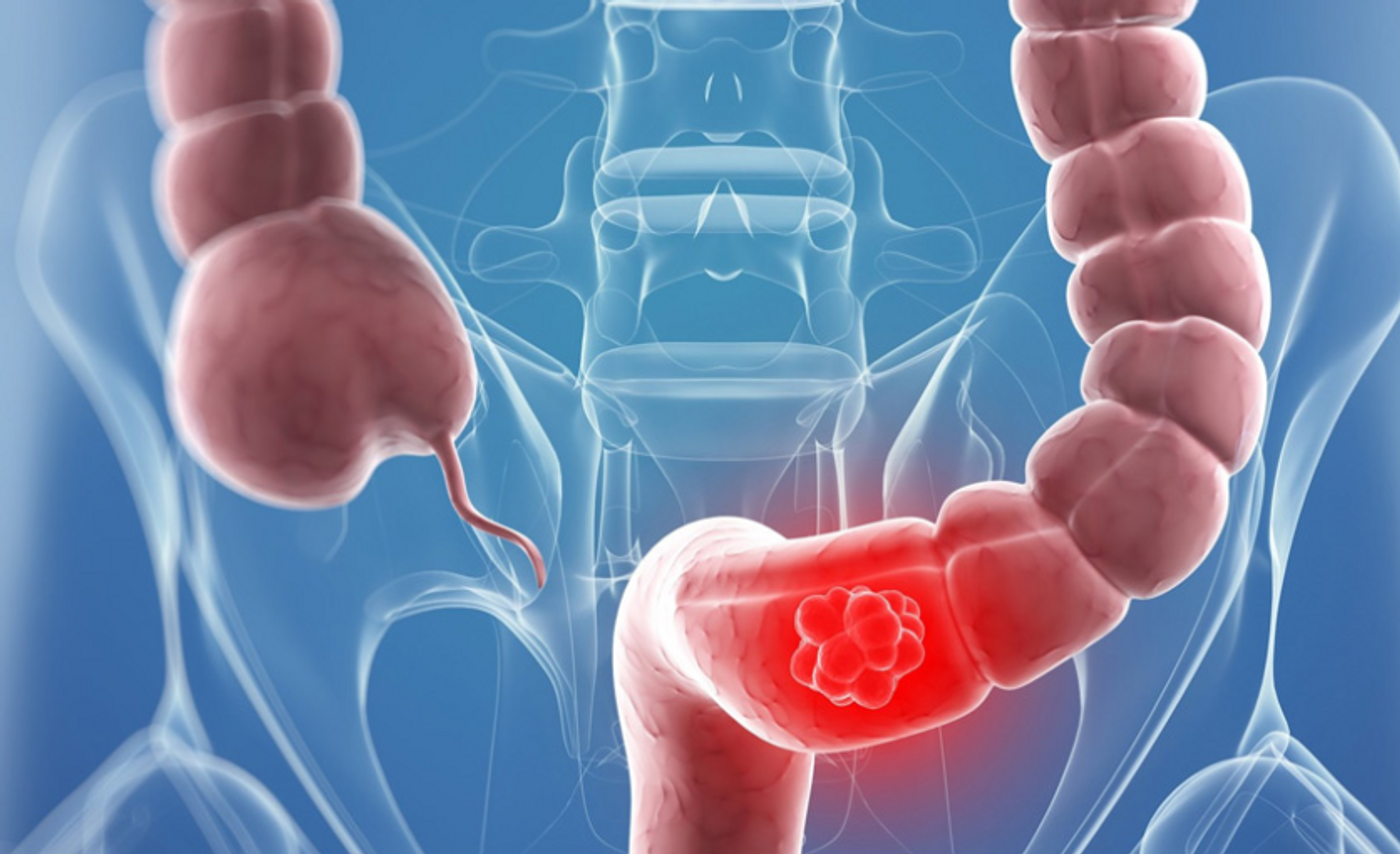
Recent studies have shown that specific bacterial species, including Streptococcus gallolyticus and Fusobacterium nucleatum, have an effect on the outcome of colorectal cancer disease and treatment. Credit: Media & Lifestyle
CRC typically begins with the growth of a noncancerous polyp on the lining of the colon or rectum. This polyp, if not removed, will continue to grow slowly over a period of 10 or 20 years. It could then develop into an adenomatous polyp, which has less than a 10% chance to develop into an invasive cancer. However; as the adenoma becomes larger, the likelihood of it turning into cancerous cells increases. Cancer which arises from the inner lining of the colorectum is known as adenocarcinoma and accounts from approximately 96% of all CRCs.
A mounting body of evidence suggests that microbes play a role in the outcome of CRC disease as well as potential treatments, including chemotherapy. According to a study published in PLoS Pathogens, scientists identified a specific species of bacteria known as Streptococcus gallolyticus, which can support the growth of colorectal tumors, depending on cell context, bacterial growth phase, and direct contact between bacteria and colon cancer cells.
In an animal model study, mice that were inoculated with Streptococcus gallolyticus, had significantly more tumors, higher tumor burden, higher dysplasia grade, and increased cell proliferation compared to mice in control groups inoculated with other species of bacteria. In humans, authors found that Streptococcus gallolyticus was found to be present in the majority of CFC patients. Interestingly, bacterial populations were found to be higher in tumor associated tissues compared to normal tissue samples that were taken from CRC patients.
In another study published in Cell, a bacterium identified as Fusobacterium nucleatum was found to be associated with chemoresistance in CRC patients. In human cohort studies, scientists found the bacteria was highly associated with patients experiencing cancer recurrence after chemotherapy treatment. In animal model studies, scientists found that Fusobacterium nucleatum has the ability to induce cell autophagy through the dysregulation of microRNA which results in tumor chemoresistance.
The results of these two studies suggest new targets for the clinical treatment of CRC. Targeting the specific actions of these two microbes which induce tumor growth and chemoresistance could provide alternative treatments to increase CRC patient prognosis.
Sources: American Cancer Society, Microcosm Magazine, PLoS Pathogens, Cell