Learning How Norovirus Infections Start
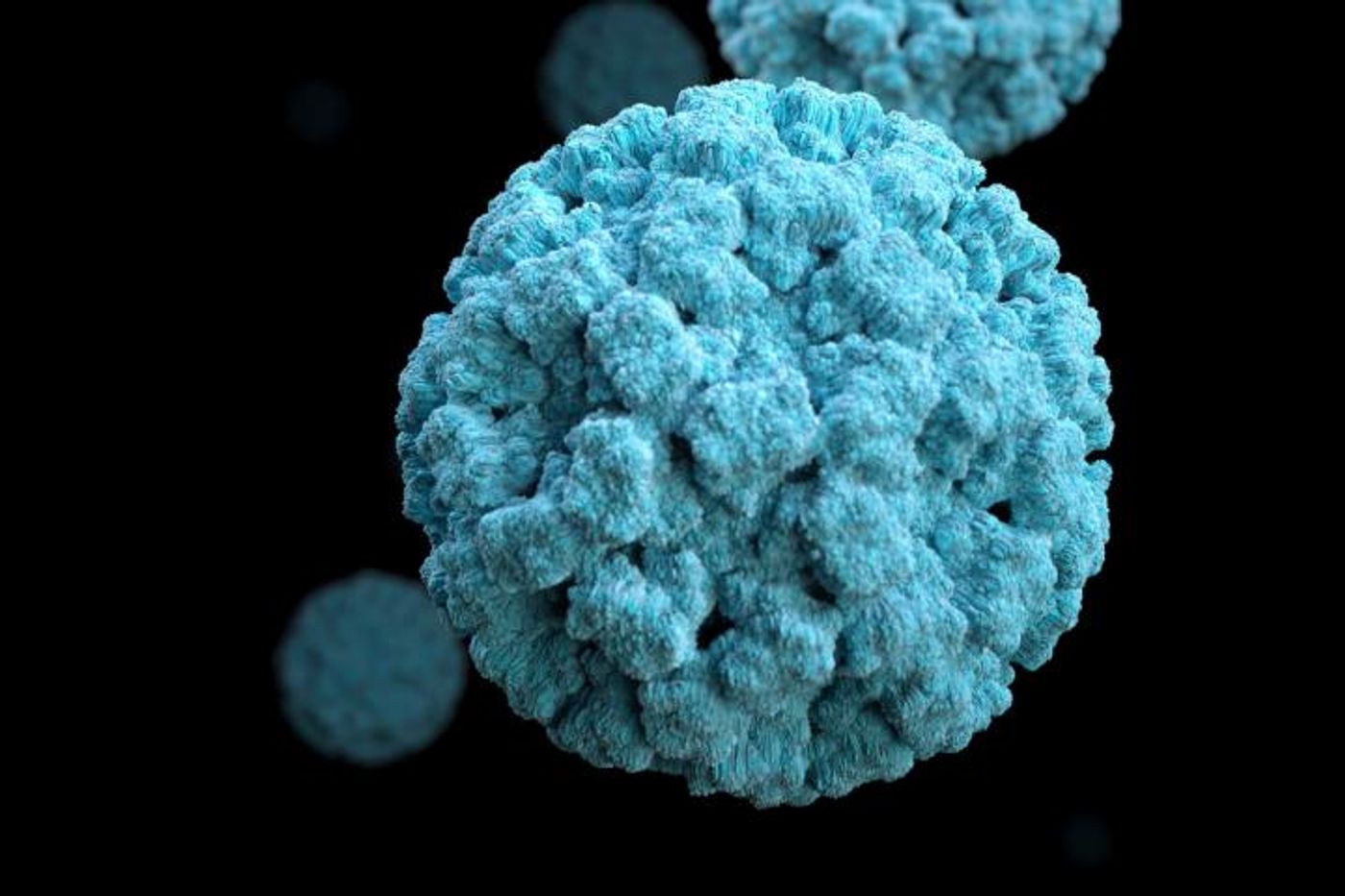
Norovirus is famous for turning cruises into nightmares for vacationers. The virus is highly contagious and is also commonly found in schools, nursing homes, and other places with dense groups of people. The virus can be deadly; it is estimated to cause the deaths of around 20,000 people every year, most of them in the developing world. There are no treatment options, and there is no vaccine. Scientists also don’t know much about how these infections start. New research may change that; scientists at Washington University School of Medicine in St. Louis found that an unusual kind of cell in the intestine could be critical to norovirus infections.
Tuft cells are named that because they feature extensions on their surface, like hairs. There aren’t many of these cells, but this new work has found that in mice, the virus infects them. The cells rapidly replicate the virus after that and start serious infections. The work, which was reported in Science, indicates that tuft cells make an attractive drug target, which may aid in the prevention or treatment of norovirus infections.
"Norovirus is one of the deadliest human pathogens that we know the least about," noted the first author of the report, Craig B. Wilen, MD, Ph.D., an instructor in pathology and immunology. "Of the viruses worldwide for which there are no antiviral drugs or vaccines, norovirus arguably kills the most people. This study provides a therapeutic avenue to explore."
There have been challenges to studying norovirus. It’s difficult to grow it in a lab; these researchers used mice to model the infection instead. Their work revealed that in mice carrying the virus, five to ten times as many tuft cells are generated. These cells have been known to sense viral or parasitic infections and initialize an immune response. Such infections also make norovirus worse when people are sick with both; this work could help show why that is.
"We were most surprised that the virus infects such a rare cell type and that even with so few cells infected, the infections can be intense and easily transmitted," explained Wilen. "In a single mouse, for example, maybe 100 cells will be infected, which is very few compared with other viruses such as the flu."
Broad-spectrum antibiotics reduced the number of tuft cells in those infected mice and reduced infection risk. But that option is not available to patients, who would experience the loss of too many beneficial gut microbes in that process, cautioned Wilen. The work does reinforce the idea that gut cells are closely linked to norovirus.
Norovirus causes gastrointestinal distress including severe vomiting and diarrhea that comes on suddenly. It is spread through contact between people, by touching surfaces that are contaminated or by eating contaminated food. Good hand hygiene can prevent the spread of the virus, which is shed in feces and vomit, sometimes for months after the illness is over.
That may be because norovirus hides away in tuft cells, added the scientists. People harboring those dormant infections are suspected to be a source of outbreaks. Understanding the mechanisms that keep the virus hidden will help prevent future recurrences.
"This raises important questions about whether human norovirus infects tuft cells and whether people who have chronic norovirus infections and continue to shed the virus long after infection do so because the virus remains hidden in tuft cells," Wilen said. "If that's the case, targeting tuft cells may be an important strategy to eradicate the virus."
Learn more about how norovirus has recently affected the United States from the video.
Sources: AAAS/Eurekalert! Via Washington University, Science