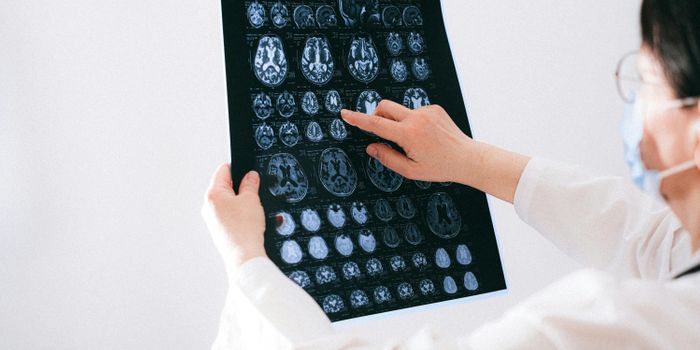
Contrary to previous thinking, Alzheimer’s disease consists of three distinct subtypes, according to a
UCLA study. The discovery could mean more highly targeted research and, ultimately, new treatments for the neurological disorder.

The UCLA study also found that one of the three variations, the cortical subtype, seems to be fundamentally a different condition from the other two, said Dr. Dale Bredesen, the study’s author, a UCLA professor of neurology and member of the Easton Laboratory for Neurodegenerative Disease Research. According to Bredesen, “Because the presentation varies from person to person, there has been suspicion for years that Alzheimer’s represents more than one illness. When laboratory tests go beyond the usual tests, we find these three distinct subtypes. The important implications of this are that the optimal treatment may be different for each group, there may be different causes, and, for future clinical trials, it may be helpful to study specific groups separately.”
The subtypes are:
- Inflammatory, in which markers such as C-reactive protein and serum albumin to globulin ratios are increased.
- Non-inflammatory, in which these markers are not increased but other metabolic abnormalities are present.
- Cortical, which affects relatively young individuals and appears more widely distributed across the brain than the other subtypes of Alzheimer’s. It typically does not seem to cause memory loss at first, but people with this subtype of the disease tend to lose language skills. It is often misdiagnosed, typically affects people who do not have an Alzheimer’s-related gene and is associated with a significant zinc deficiency.
The two-year study, which involved metabolic testing of 50 people, was published in the journal Aging and reported in
Bioscience Technology. The article explained that there is no effective therapy for Alzheimer’s, scientists have yet to identify the cause and some studies cite metabolic abnormalities such as insulin resistance, hormonal deficiencies and a high level of an amino acid in the blood.
In 2014 Bredesen demonstrated that making lifestyle, exercise and diet changes to improve metabolism reversed cognitive decline in nine out of 10 patients with early Alzheimer’s disease or its precursors. The current finding grew out of an extensive evaluation of data from that study, and it could eventually help scientists to find more precise targets for treatments in the same way they have made advances in treating other diseases. For instance, Bredesen said, researchers have been able to develop precise treatments for cancer by sequencing tumor genomes and comparing them to the patients’ genomes to see what drives the formation and growth of tumors.
He added, “However, in Alzheimer’s disease, there is no tumor to biopsy. So how do we get an idea about what is driving the process? The approach we took was to use the underlying metabolic mechanisms of the disease process to guide the establishment of an extensive set of laboratory tests, such as fasting insulin, copper-to-zinc ratio and dozens of others.”
Bredesen and his team will now try to determine whether the subtypes have different underlying causes and whether they respond differently to potential treatments.