Different Autism Risk Genes Lead to Similar Brain Dysfunction
Researchers have been trying to determine what causes autism spectrum disorder for many years. Those efforts have revealed that hundreds of genes have small sequence variations that are linked to autism. New work has investigated the impact of some of those variations; researchers used simplified, miniature models of human brains called organoids to analyze them. This effort showed that while some of those autism-linked variants have different effects initially, they ultimately lead to similar problems in the development of neurons in human brains. The findings have been reported in Nature.
A lot of work has gone into seeking common features and patterns "among the many risk genes associated with autism." If scientists can uncover shared mechanisms, it could open up new intervention or treatment options, regardless of the genetic cause of the disorder, noted senior study author Paola Arlotta, a Harvard University Professor and member of the Stanley Center for Psychiatric Research at the Broad Institute.
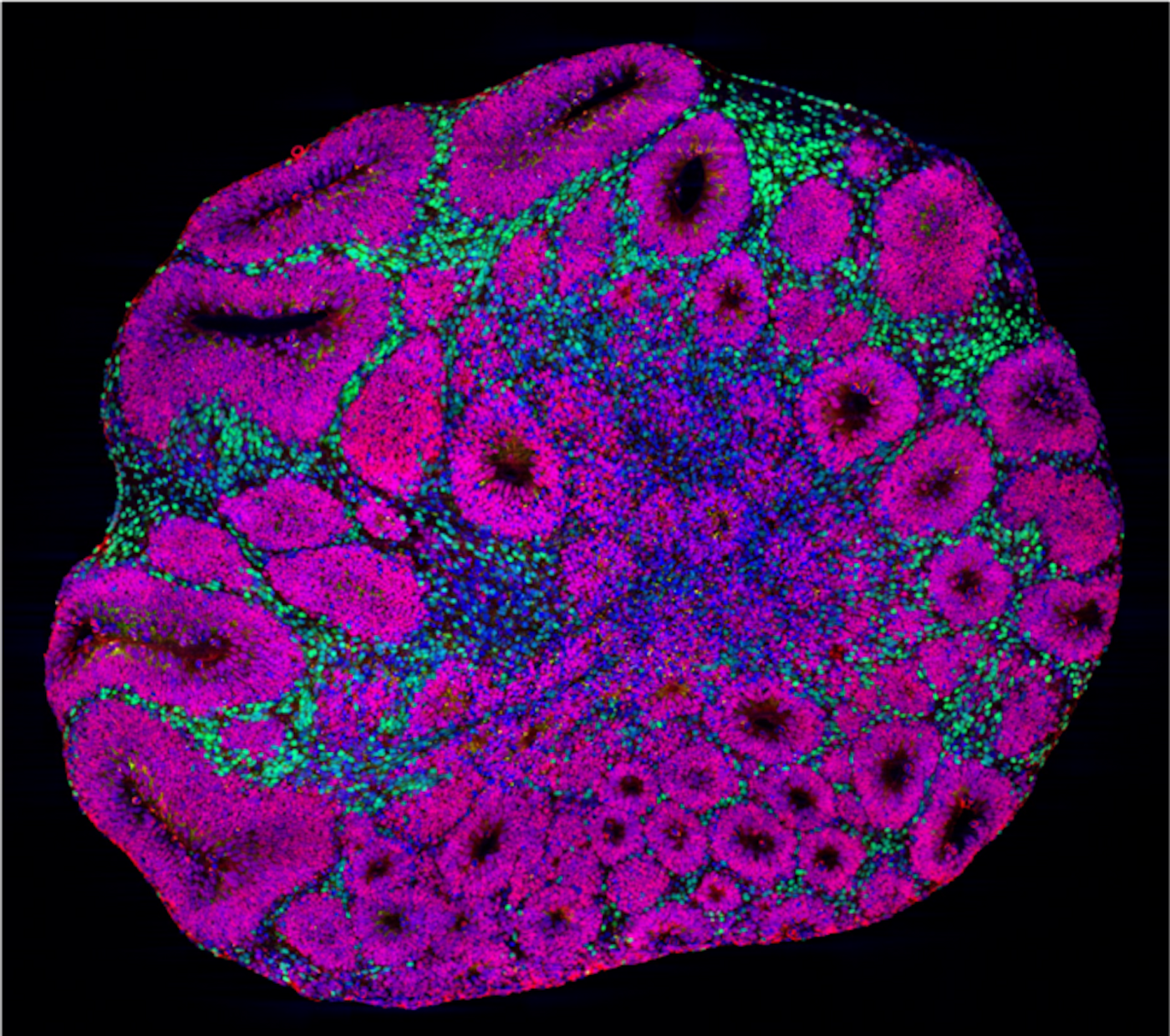
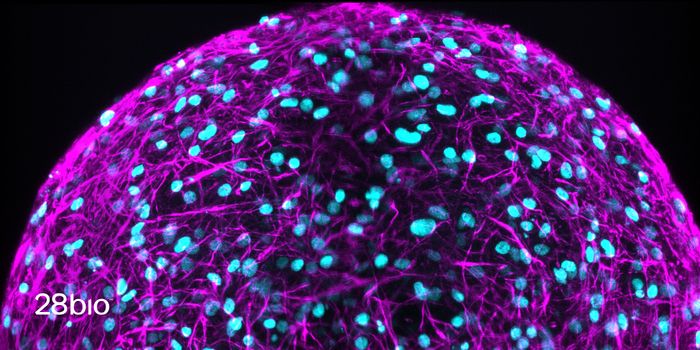
Arlotta's team has been using organoids to model the human cerebral cortex; they are created with stem cells that are programmed to specialize into cell types that are found in that region of the brain. These cells self-organize into cortex mini-models. “It is a dream come true to now see that organoids can be used to discover something unexpected and very new about a disease as complex as autism," noted co-lead study author Silvia Velasco, PhD, a postdoctoral fellow in the Arlotta lab.
In this study, the team began with variations that are found in genes called SUV420H1, ARID1B, and CHD8. The functions of the genes are not fully understood, so the researchers were interested in whether they might cause similar pathologies in the organoids, explained co-lead study author Bruna Paulsen, PhD, a postdoctoral fellow in the Arlotta lab.
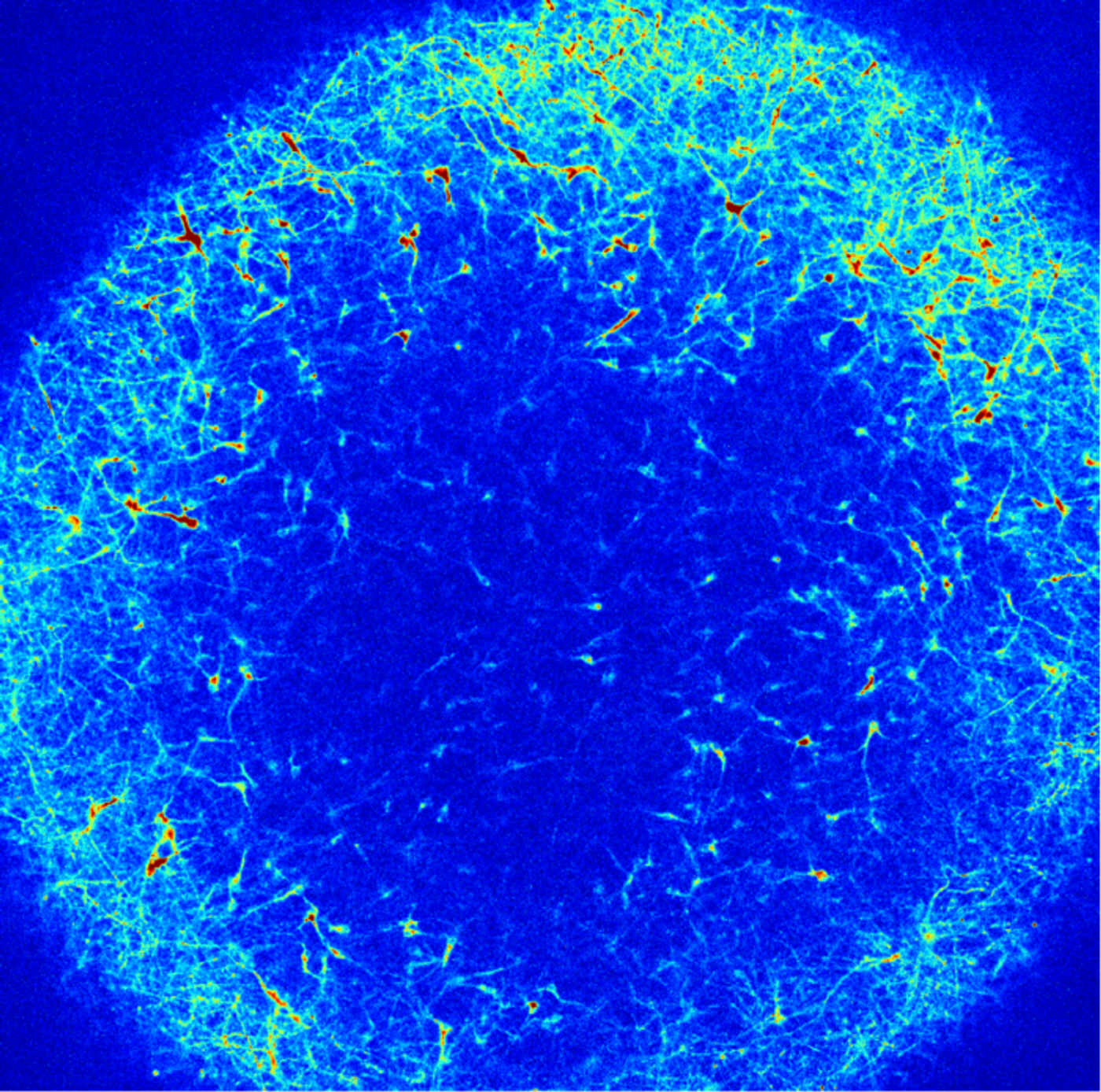
The organoids were grown for several months, then gene and protein expression was assessed at the single cell level. The team also investigated calcium signaling to see if neural activity was disrupted. This work indicated that all the risk genes caused neural development to either slow down or speed up, and some neurons were developing at the incorrect time. The genes also only affected two cell types: GABAergic neurons, which are inhibitory, and deep-layer excitatory projection neurons. It may be possible to treat autism by targeting these cells.
“The cortex is made in a very orchestrated way: each type of neuron appears at a specific moment, and they start to connect very early. If you have some cells forming too early or too late compared to when they are supposed to, you might be changing the way circuits are ultimately wired,” said co-lead study author Martina Pigoni, PhD, a former postdoctoral fellow in the Arlotta lab.
Organoids were also created from donated stem cells. The researchers wanted to know if the genetic background of an individual influenced the organoids, said co-lead study author and computational biologist Amanda Kedaigle.
The researchers found that organoids from different donors still reflected similar alterations in neural development, but the severity varied from one person to the next; an individual's genome seems to moderate the impact of the risk variants.
“It is puzzling how the same autism risk gene mutations often show variable clinical manifestations in patients. We found that different human genomic contexts can modulate the manifestation of disease phenotypes in organoids, suggesting that we may be able to use organoids in the future to disentangle these distinct genetic contributions and move closer to more a complete understanding of this complex pathology,” Arlotta said.