Childhood Cancer Survivors Are Still at Risk
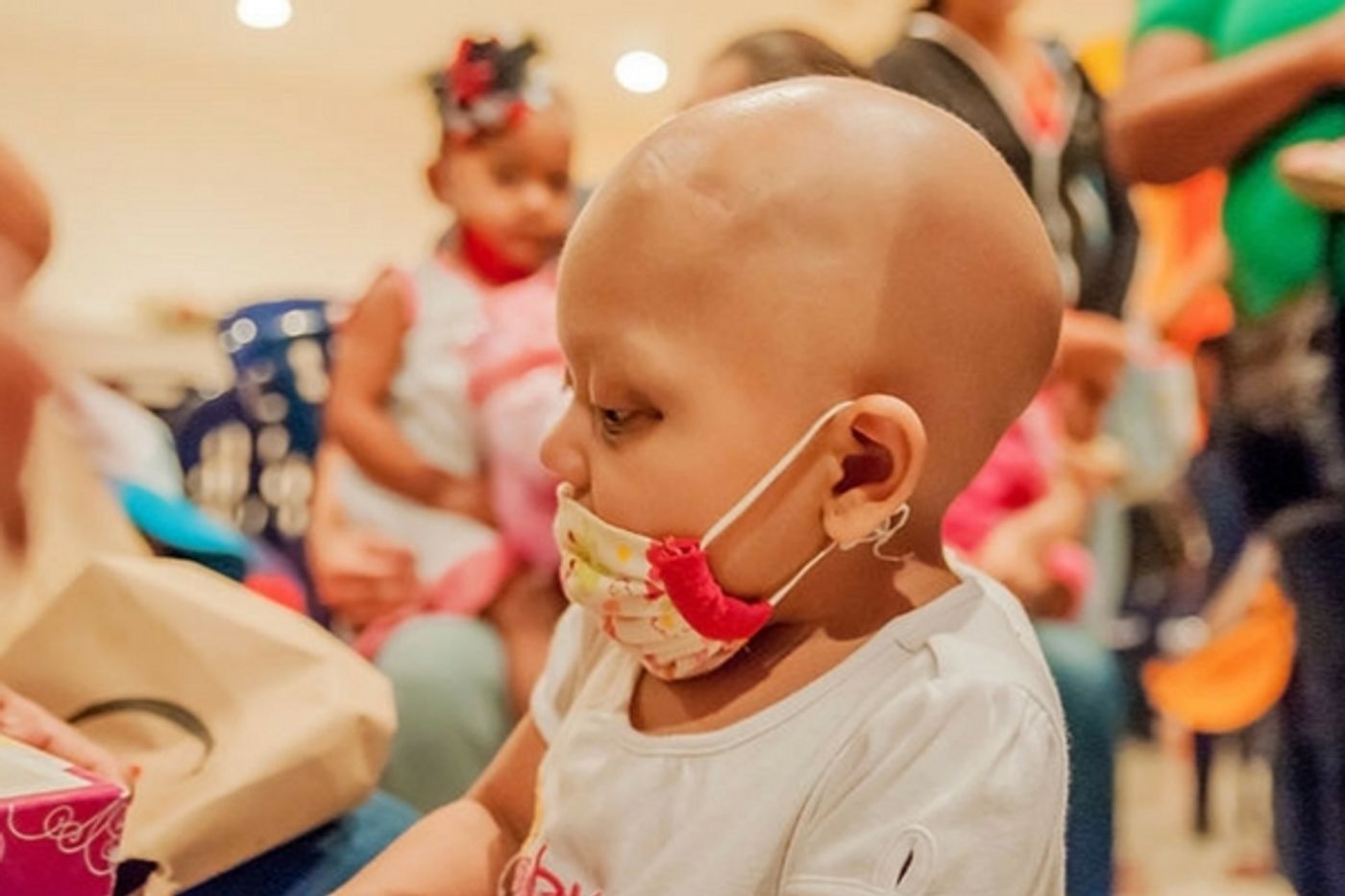
Surviving cancer is a major win for anyone, but when a child survives pediatric cancer, it's an especially sweet victory. Imagine the heartbreak, however, when a child who survived a bout of cancer grows up and receives another devastating diagnosis of cancer. As it turns out, children who have a history of cancer, are at a much higher risk for developing meningiomas, which are the most common form of adult brain tumors. In children who have had cancer, these tumors are associated with the use of radiation that was part of the treatment plan in patients who had leukemia or pediatric brain cancer.
A team at the Princess Margaret Cancer Centre, University Health Network in Toronto, Canada have published their recent research which suggests that the DNA is actually damaged to the point where it's rearranged and mutated, causing the adult brain tumor. This DNA damage occurs in childhood, but the tumors, called RIMs (radiation induced meningiomas) can occur decades later.
Principal investigator Gelareh Zadeh, a neurosurgeon-scientist and the Head of Surgical Oncology at UHN-Toronto is also an Associate Professor at the Division of Neurosurgery. Her work looked closely at the biology of RIMs and compared them to the meningiomas that occur in adults who have not suffered through childhood cancer and as such, were not exposed to cranial radiation. The study was published in the journal Nature Communications.
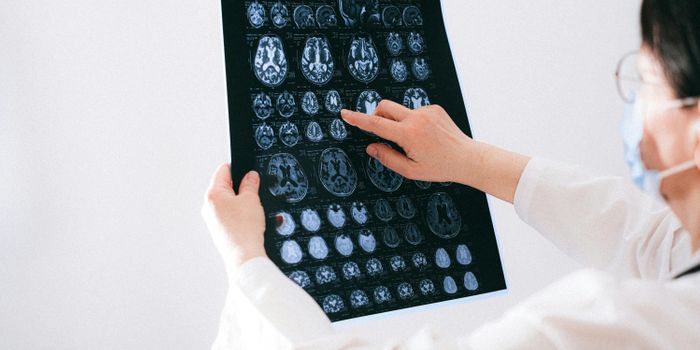
While the two kinds of meningiomas are similar, in some ways, there are important differences. Dr. Zadeh explained, "Radiation-induced meningiomas appear the same on MRI and pathology, feel the same during surgery and look the same under the operating microscope. What's different is they are more aggressive, tend to recur in multiples and invade the brain, causing significant morbidity and limitations (or impairments) for individuals who survive following childhood radiation."
The team looked at the tumors developed in adulthood in a group of patients who had received cranial radiation in childhood as a treatment for cancer. While 74% of the adults studied were former cancer patients, the rest of the study participants were from Germany and received cranial radiation as a treatment for scalp ringworm. Treating ringworm on the scalp with radiation is no longer done, but many years ago in Germany, it was the norm.
Dr. Ken Aldape is a neuropathologist-scientist and Director of the MacFeeters-Hamilton Neuro-Oncology Research Program at UHN and was the co-principal investigator with Dr. Zadeh. Aldape explained further, stating, "It is an important clinical problem because it presents a paradoxical dilemma that while cranial-spinal radiation is needed to cure many childhood cancers, an unfortunate consequence is that 10-to-15-years following radiation treatment some survivors develop meningiomas. Our research identified a specific rearrangement involving the NF2 gene that causes radiation-induced meningiomas. But there are likely other genetic rearrangements that are occurring as a result of that radiation-induced DNA damage. So one of the next steps is to identify what the radiation is doing to the DNA of the meninges. In addition, identifying the subset of childhood cancer patients who are at highest risk to develop meningioma is critical so that they could be followed closely for early detection and management." The team at Princess Margaret talks about their work in the video below; take a look.
Sources: UHN Toronto, Nature Communications, American Brain Tumor Association