These 3D-Printed Mouse Ovaries Are Fully Functional
Researchers based out of Northwestern University Feinberg School of Medicine and McCormick School of Engineering, both located in Illinois, have been working on a method of bringing fertility back to the lives of those who want to give birth, but can’t.
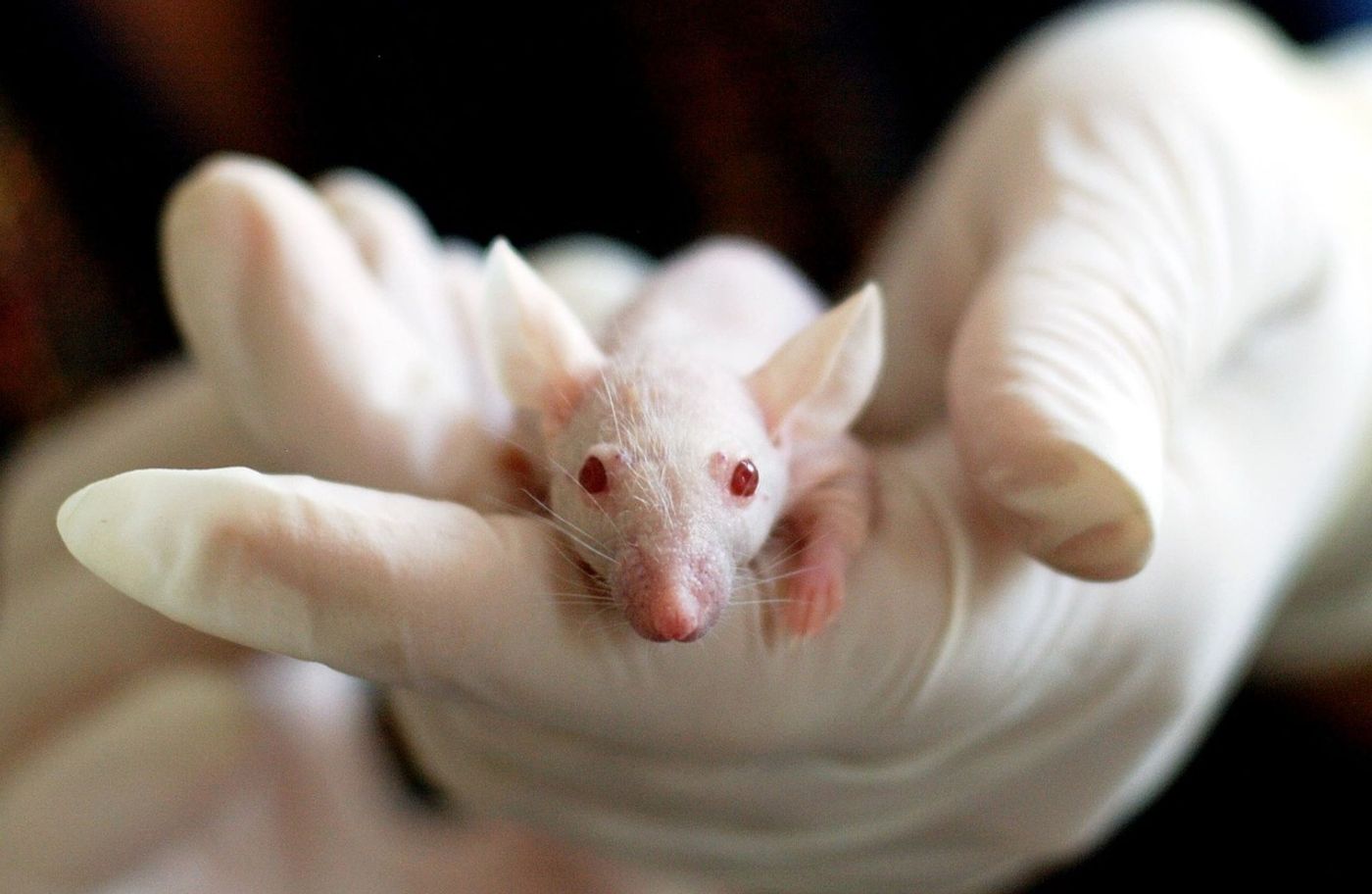
Starting with lab mouse research, they report being able to successfully 3D-print “ovaries” that were fully functional; capable of helping female mice give birth to live young despite complications that otherwise prevented them from doing so.
Image Credit: Tiburi/Pixabay
Published in the journal Nature Communications, the researchers describe how the method’s success could translate to real-world help for even humans.
Infertility can happen for many reasons, whether a person underwent harsh treatments to help with other life-threatening illnesses, diseases destroyed the ovaries’ operational prowess, or genetics simply rendered the person unable to reproduce.
No matter what the case is, this study shows that there could be a light at the end of the tunnel for females who want to be mothers and aren’t able to be for one health-based reason or another.
Although scientists have been growing organs in labs for years (including ovaries), 3D-printing is still an emerging technology that has the potential to revolutionize the way we manufacture organs in a lab-based environment. Not only is it more cost-efficient, but it’s also faster.
Related: Researchers grow a human ear on the back of a lab rat
Not only did the 3D-printed “ovaries” work as expected for producing the egg cells necessary for conception, but they also worked properly as hormone regulators, which is another key importance as some women have both ovaries removed surgically to prevent health issues down the line.
To make 3D-printing ovaries possible, the researchers had to dissect a real ovary and study its key building blocks under a microscope to better understand how to replicate it with a 3D printer.
They had found that a unique lattice layer of collagen actually works as an exoskeleton and deeper layers in the ovary are made up of other complicated things like follicles and tissues, all of which would need to be replicated to produce a working ovary.
Once they understood the collagen exoskeleton, they had to find a way to discharge tissue 'ink,' which was made out of gelatin, out of a 3D printer head and into a 3D-printed scaffold. They found this 'ink' needed to be expelled at a very specific temperature (30º C) so that it wouldn’t be too hot and watery or too cold and clumpy for the 3D printing process.
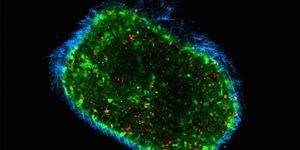
After determining what temperature would work, they moved on to producing the layers of the arificial ovary. Although a lot of trial and error went into it, they finally came up with a solution that seemed to work and they moved to the testing phase.
Image Credit: Northwestern Unviersity
This was where the researchers reportedly performed surgery on nine different female mice, removing one functioning ovary and implanting the 3D-printed ovary in its place. Two of the mice were purposely left with infertility as controls, and out of the seven others, three had babies after mating with males.
To ensure that there would be no genetic issues down the line, researchers continually allowed the newborns to grow up and mate with other mice for generations to ensure that the 3D-printed ovary in grandma mouse wouldn’t somehow have an adverse side-effect on the development or health her great grandson or great, great granddaughter.
To their surprise, everything worked out as it would have if grandma mouse had a natural ovary, which suggests that, at least in animal models, 3D-printed ovaries could become a possible safe treatment for infertility.
Related: 3D printing can be used to create stem cells
The team plans to test their 3D-printing method of ovary replacements in larger animals down the line. Since mouse ovaries are relatively small and simple, trying to replicate a much larger ovary that mimics the size of a human ovary will be more challenging. Nevertheless, it’s an important step to ensure we get things right the first time.
The future looks bright for 3D-printing, which will automate so many processes in both the manufacturing and medical industries. It ought to be interesting to see what else comes out of this fascinating technology.
Source: Popular Science, Wired