Hereditary Myeloid Neoplasm Predisposition
The systems in place for classification of cancer have historically been based on the type of tissue and primary site from which the cancer originates or the location in the body where cancer initially developed. Part of the primary site determination includes histological analysis and breaks cancers into the following six types: Carcinoma, Sarcoma, Myeloma, Leukemia, Lymphoma, and Mixed Type. Some of these are solid tumors and others are conditions that involve specific cell lines like in leukemia and myeloma. Prior to these recent times, cancers were classified after they had already been established within the body as determined by a tissue biopsy. Modern molecular analyses allow for more advanced knowledge to help in predicting where and how, and in whom, cancer may strike. An article published in the June 29, 2018 edition of the journal Expert Review of Hematology found germline changes are significant risk factors for familial myeloid malignancy development in adulthood.
History
In the 1970s, leukemia subject matter experts from France, the United States, and England collaborated to divide Acute Myeloid Leukemia (AML) into 9 distinct categories based on very specific cellular morphologies; examination and diagnosis was reached after microscopic analysis with routine and special cytochemical stains, some of which are still used today. The system, known as the French-American-British (FAB) classification system was loosely based on the type of cancerous cells present and/or their maturation stage. While some still find this system useful, so much more complex information is known about hematologic and lymphoid cancers, rendering this diagnostic method more subjective; since it is based on cell differentiation, even the most astute morphologists can struggle to make a diagnosis in cases where presentation is not straightforward. The World Health Organization (WHO) created an updated classification of tumors of hematologic and lymphoid origin in 2001. The WHO system merged the morphologic features useful in the FAB and the genetic abnormalities that were known to be associated with certain cancers through cytogenetic analysis. Since 2001, there have been multiple updates to the WHO classification to account for the increasing amount of molecular data available for assistance in diagnosis, prognosis, and treatment of cancers.
Current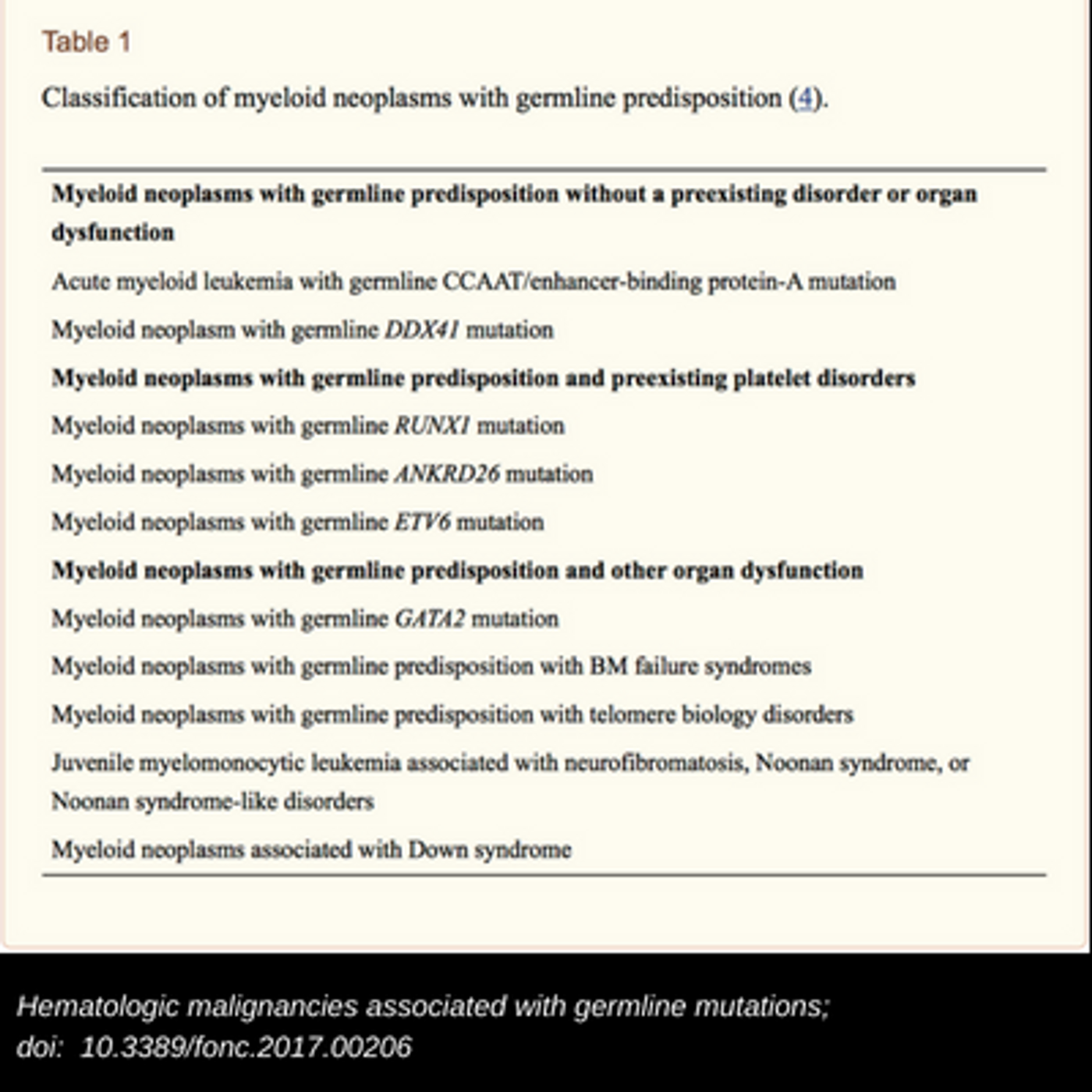 
Most recently, in 2016, the WHO revised their oncologic classification system again to recognize hereditary myeloid disorders under the AML category. While it is understood that many hematologic malignancies are sporadic, there’s new information that confirms that mutations in specific and known cancer-driving genes can be inherited or familial; this predisposition leads to increased risk of multigenerational leukemia diagnoses. In addition, there are germline changes that are associated with certain conditions which put those individuals at high risk of leukemia development, like Down Syndrome, Diamond-Blackfan Anemia, and some platelet disorders. The literature indicates that over the span of the last ten years, a dozen or so hereditary myeloid malignancy syndromes occurring in adulthood have also been identified as a result of inherited bone marrow failure syndrome (IBMFS). While some have few hematologic identifiers in their early lives, these patients then present with adult aplastic anemia, myelodysplastic syndrome (MDS), or acute leukemia (AL). The updated WHO classification can now help providers be more aware of this unique group of patients who need to be evaluated in the context of their hereditary predisposition, the effects of that predisposition on therapies chosen, and the potential need for family members to be evaluated as part of an oncology workup.
New testing is available through the use of sequencing analysis and continues to be are area of laboratory testing growth. Sequencing determines if a mutation, particularly one aligning with current clinical knowledge, is present in one of these gene regions characterized. Genes associated with hereditary myeloid malignancy and IBMFS include some well-known cancer drivers like RUNX1, TP53, BRCA1, BRCA2, ETV6, NF1, and GATA1. Some lesser known genes include: ANKRD26, DDX41, ACD, CTC1, and HAX1.
Sources: Expert Review of Hematology, Seminars in Hematology, University of Chicago, Frontiers in Oncology, National Cancer Institute, Blood, International Agency for Research on Cancer, WHO Classification of Tumours of Haematopoetic and Lymphoid Tissues,