Red Blood Cells: More than just an Oxygen Delivery Service
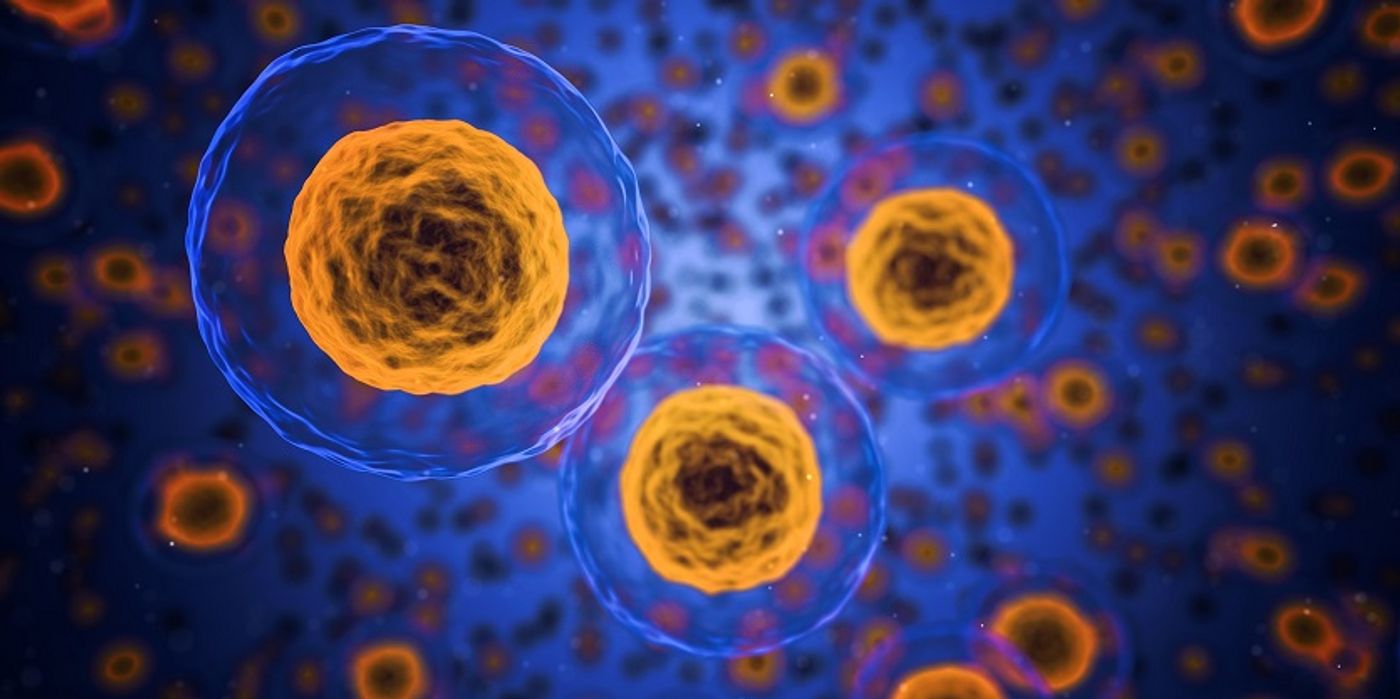
The human body is a complex network of systems that often interact and affect each other. Recent work shows that red blood cells (RBCs) may have more roles than to just bring oxygen from one part of the body to another. RBCs have recently been implicated in the regulation of parts of the immune system, in particular T-cell proliferation. While work on this is not extensive, a group from Australia hypothesized that RBCs altered by disease could change the effects RBCs had on other cells.
To do this, they decided to introduce RBCs to the cancer cell line A549. This cell line originates from non-small lung cell lung carcinoma (NSCLC), which releases several chemokines, cytokines, and growth factors that creates a microenvironment around the tumor that promotes tumor growth. Culturing two separate samples, one with RBCs alone (oRBC) and the other with RBCs cultured alongside the cancer cell line A549 (ccRBC), they generated an experimental RBC and a control. Isolating the RBC from these cultures, the ccRBC sample was found to be enriched in inflammatory cytokines, and other tumor-promoting molecules. These molecules were also found in the A549 media and thought to have been brought along during the purification process. This is hypothesized to be because of the Duffy antigen receptor for chemokines (DARC) on the RBC membranes, which is known to bind many of these molecules.
After identifying the difference between oRBCs and ccRBCs, the team wanted to examine how they interact with the immune system. Introducing both oRBC and ccRBC to Jurkat leukemia T-cells showed an interesting effect. Only ccRBCs were able to stimulate T-cell proliferation, although both oRBC and ccRBC could inhibit activation-dependent apoptosis in T-cells. ccRBC also induced a specific stimulation of CD8+ proliferation. Both of these observations had been seen in previous work. RBC is known to stimulate T-cell proliferation, and CD8+ T-cell growth can be seen in patients who had undergone several blood transfusions. There hadn’t been a differentiation between healthy RBCs and altered RBCs, however. The most significant find was that ccRBCs from this study could induce T-cells to enter an immunosuppressive state, though this may be due to the particular chemokines and cytokines from the A549 cell line used.
The team finishes their work suggesting “that if there is interaction between the RBCs and cancer cells there may be some downstream immunological effects in vivo.” They continue to announce future experiments designed at examining this interaction with in vivo. Red blood cells are quite abundant in your body, and learning how they may interact with other parts of the body is something we should all be interested in.