Genetic Tweaks Transform Salmonella into Tumor Destroyers
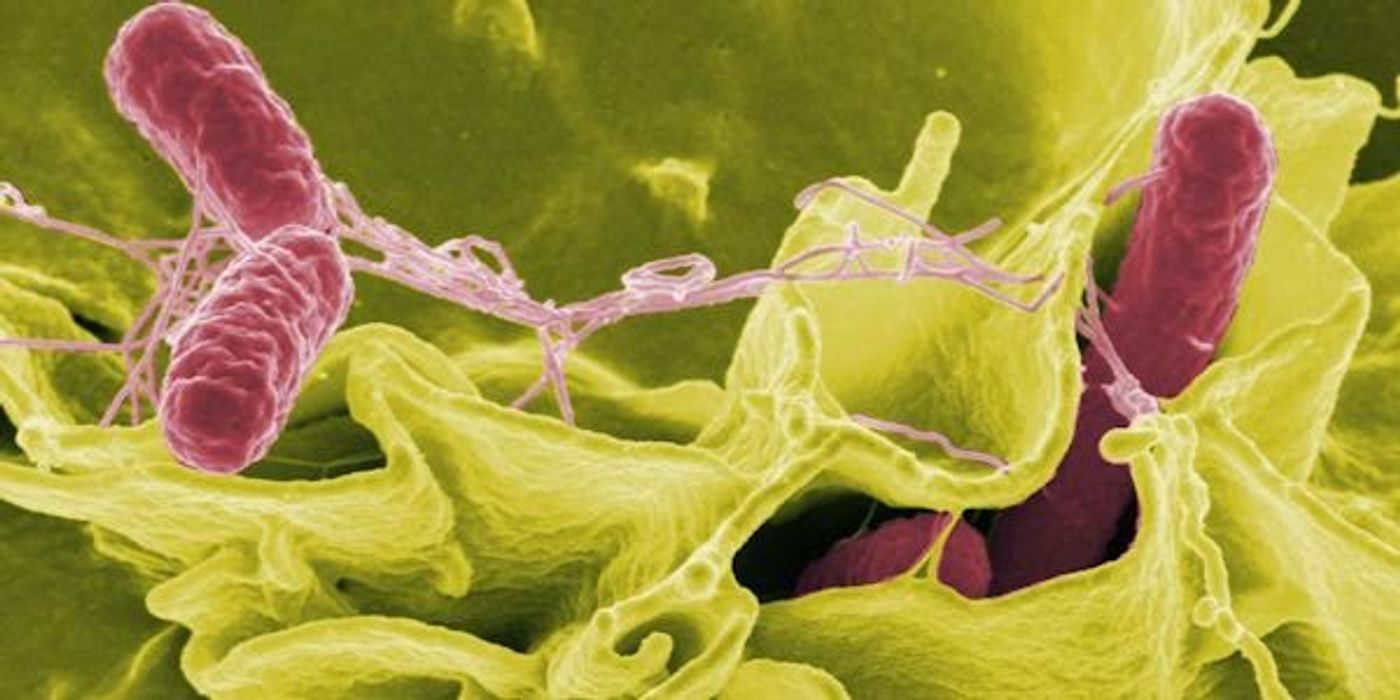
Salmonella, the bacteria that is bane of all restaurants and grocery stores, has now been transformed into “tumor-seeking missiles” to help fight one of the most lethal forms of brain cancer - glioblastoma.
Using clever manipulations that exploit both the bacteria’s normal biology and the brain tumor environment, researchers at Duke University created a genetically modified version of Salmonella typhimurium. But how can a strain of bacteria that causes typhoid-like diseases in mice and food poisoning in humans be commandeered to treat brain cancer?
Duke University researchers aimed to extend previous studies that suggest bacterial invasion could potentially kickstart the body’s immune system into fighting tumors. Because attempts using only the detoxified version of S. typhimurium have been unsuccessful, the team knew they would have to add tweaks to outsmart the cancer.
To begin with, the team used a detoxified version of S. typhimurium that was starved for purine - a nucleic acid that just happens to be found in abundance in brain tumors. This has the desired effect of targeting the bacteria to the tumor source.
Then, the team modified the bacteria such that they produced 2 chemicals: Azurin - a pro-apoptotic drug, and p53 - a tumor suppressor protein. These chemicals have the combined effect of inducing cell death. In particular the cellular suicide would occur when oxygen levels are low. Not coincidentally, tumor are well-known to be oxygen-deprived.
The genetic modifications work in concert to stage an unusual attack in glioblastoma tumors. Tested in rat models, the bacteria treatment led to a 19 percent survival rate over 100 days. By contrast, untreated mice survived a median of 26 days.
While nearly 20 percent may not sound impressive, we have to consider that the current median survival time for glioblastoma is around 15 months. "Since glioblastoma is so aggressive and difficult to treat, any change in the median survival rate is a big deal," said Jonathan Lyon, a co-author of the study. "And since few survive a glioblastoma diagnosis indefinitely, a 20 percent effective cure rate is phenomenal and very encouraging."
Of note glioblastoma multiforme is the most common and deadly form of primary brain cancer. In GBM, malignant glial cells form vast networks of tendrils throughout the brain, making it nearly impossible to surgically remove all the cancerous tissues. Dubbed as the “octopus tumor,” GBMs can evade even the most aggressive surgeries, chemotherapies, and radiotherapies, leaving patients with a five-year survival rate of less than 10 percent.
"A major challenge in treating gliomas is that the tumor is dispersed with no clear edge, making them difficult to completely surgically remove. So designing bacteria to actively move and seek out these distributed tumors, and express their anti-tumor proteins only in hypoxic, purine rich tumor regions is exciting," said Ravi Bellamkonda, the study’s senior author. "And because their natural toxicity has been deactivated, they don't cause an immunological response. At the doses we used in the experiments, they were naturally cleared once they'd killed the tumors, effectively destroying their own food source."
The team is conducting further studies to improve the efficacy of this treatment. In particular, they are hopeful that this bacteria-turned-tumor-destroyer platform can be adapted with different drugs to treat multiple tumor types.
Additional source: Duke University