The Detrimental Side Effects of Vascular Grafts
With a constantly increasing amount of cardiovascular disease patients, doctors have more and more reasons to use vascular grafts and other medical implants during treatment. These devices are prone to infection that can lead to serious complications, so scientists are now more than ever focused on preventing and treating these infections.
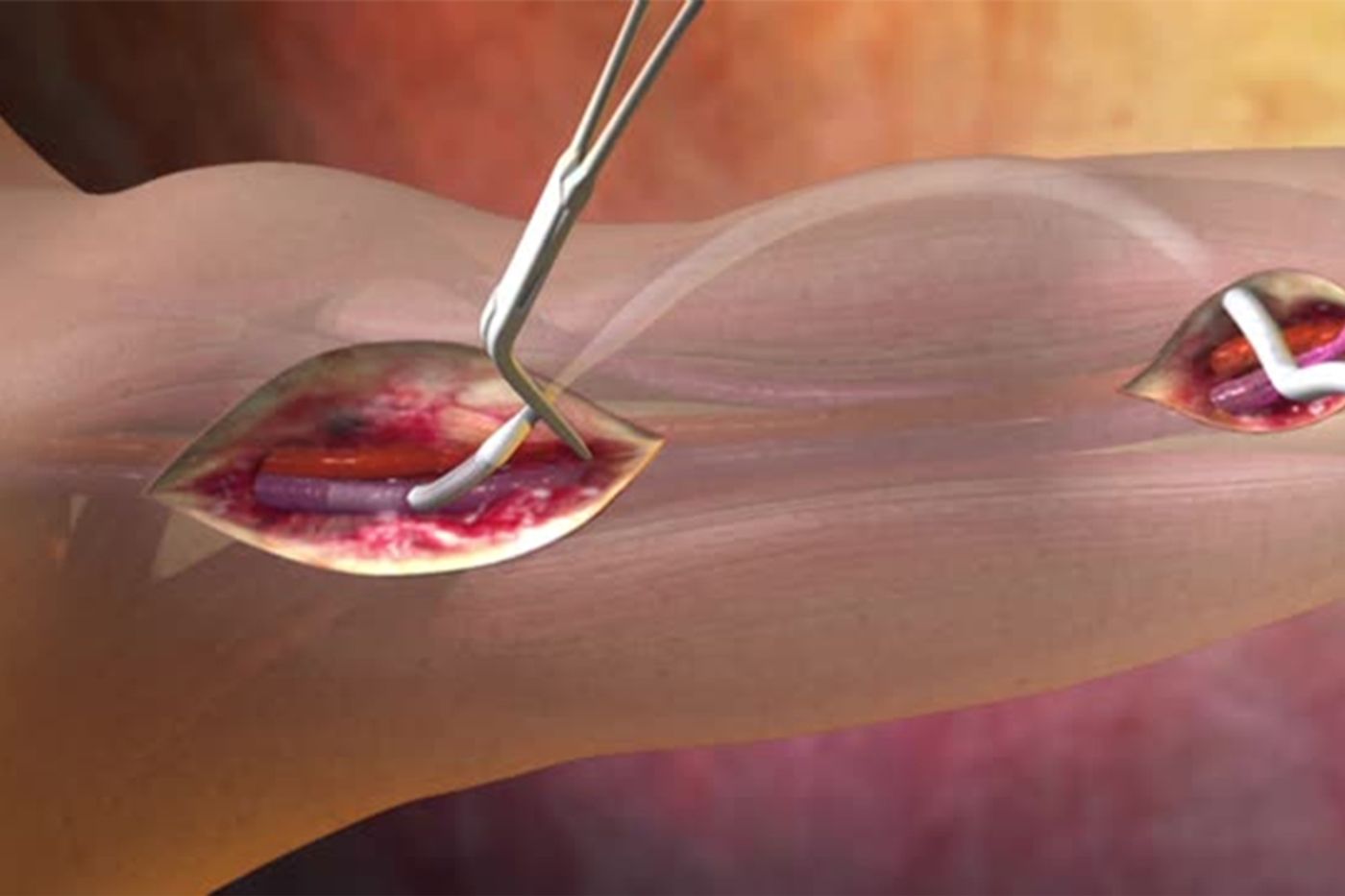
Vascular grafts can help reopen a closed or narrow blood vessel to improve blood flow. The procedure is generally less invasive than other surgeries and no general anesthesia is required.
Studies show that nearly a third of the population carry a bacteria called Staphylococcus aureus (S. aureus) in their noses without knowing it. In many cases this bacteria is harmless, but S. aureus is a leading cause of infected vascular grafts because of its ability to stick to implants by forming protective layers of biofilm.
Microorganisms form biofilms to attach to surfaces like S. aureus attaches to vascular grafts. They do so thanks to specialized cells that that release a compound called “extracellular polymeric substance matrix,” reduced growth rates, and a manipulation of gene expression.
“Biofilms can shelter bacteria from the patient's immune responses or antibiotic treatment,” said lead scientist Bettina Loffler, MD. “These biofilm layers are difficult to detect because they are often unaccompanied by clinical symptoms.”
Currently no effective treatment exists against S. aureus vascular graft infections. “Biofilms require antibiotic concentrations up to 1000 times higher than normal and these concentrations are not clinically feasible,” Loffler explained. “It is of great importance to understand the underlying pathogenesis of biofilm formation on vascular grafts in order to find quick and effective treatment possibilities without having to resort to invasive procedures such as surgical removal."
Loffler recently conducted a study with a newly developed mouse model that resembles closely a human graft infection. First, a catheter is inserted via blood vessel; in this case it was the right carotid artery. Bacteria, like S. aureus, gain access to the catheter through the bloodstream. In the study, researchers introduced bacteria into tail veins a week after catheter insertion.
"Just as in humans, with this model the bacteria need to overcome the stress of the blood flow, the shear stress induced by the blood flow, and the host's immune system to form a biofilm infection on the catheter," Loffler said. Developing this new mouse model will help researchers better study these types of infections and eventually establish more effective treatments and detection strategies.
From their studies with the new model, they found that all S. aureus strains tested formed biofilms in vivo (in a living organism) whether or not they also formed high biofilm levels in vitro (in cell culture). What does this mean? The tendency for S. aureus to build biofilms in vascular grafts stems from them being highly adaptive to their surroundings.
Additionally, PET and MRI imaging showed high levels of inflammation at the catheter site as well as decreased blood flow through the catheter due to both the infection and bacterial biofilm formation.
"Our model takes all steps of the pathogenesis of infected implants into account and closely represents the clinical situation," Loffler said. "It provides a solid platform for microbiological and immunological experiments that could provide crucial insights into the pathogenesis as well as the diagnosis and treatment of these devastating infections."
Loffler’s study was recently published in The American Journal of Pathology.
Sources: Elsevier Health Sciences, Centers for Disease Control and Prevention, Emerging Infectious Diseases, RadiologyInfo.org
![MRI-[18F]-FDG imaging shows a high level of inflammation at the site of the catheter 10 days after Staphylococcus aureus infection.](https://d3bkbkx82g74b8.cloudfront.net/eyJidWNrZXQiOiJsYWJyb290cy1hc3NldHMiLCJrZXkiOiJfcHVibGljXC9fZmlsZXNcL3N5c3RlbVwvY2tcL3RyZW5kaW5nXC92YXNjdWxhciBncmFmdF9lZDdkODBiZGRlYzlhMGI3YzM5MDMxODYzZDljOWY1Mi5qcGciLCJlZGl0cyI6eyJyZXNpemUiOnsid2lkdGgiOjE0MDAsImZpdCI6ImNvdmVyIn19fQ==)