Trauma patients rushed into the hospital are at a great risk for complications from blood clots, and some researchers believe quick application of blood clot prophylaxis is the key to reducing this risk. Other researchers are afraid that administering these drugs too soon is too risky - putting trauma patients at risk for intracranial hemorrhage. To settle the debate once and for all, researchers from the American College of Surgeons conducted a study.
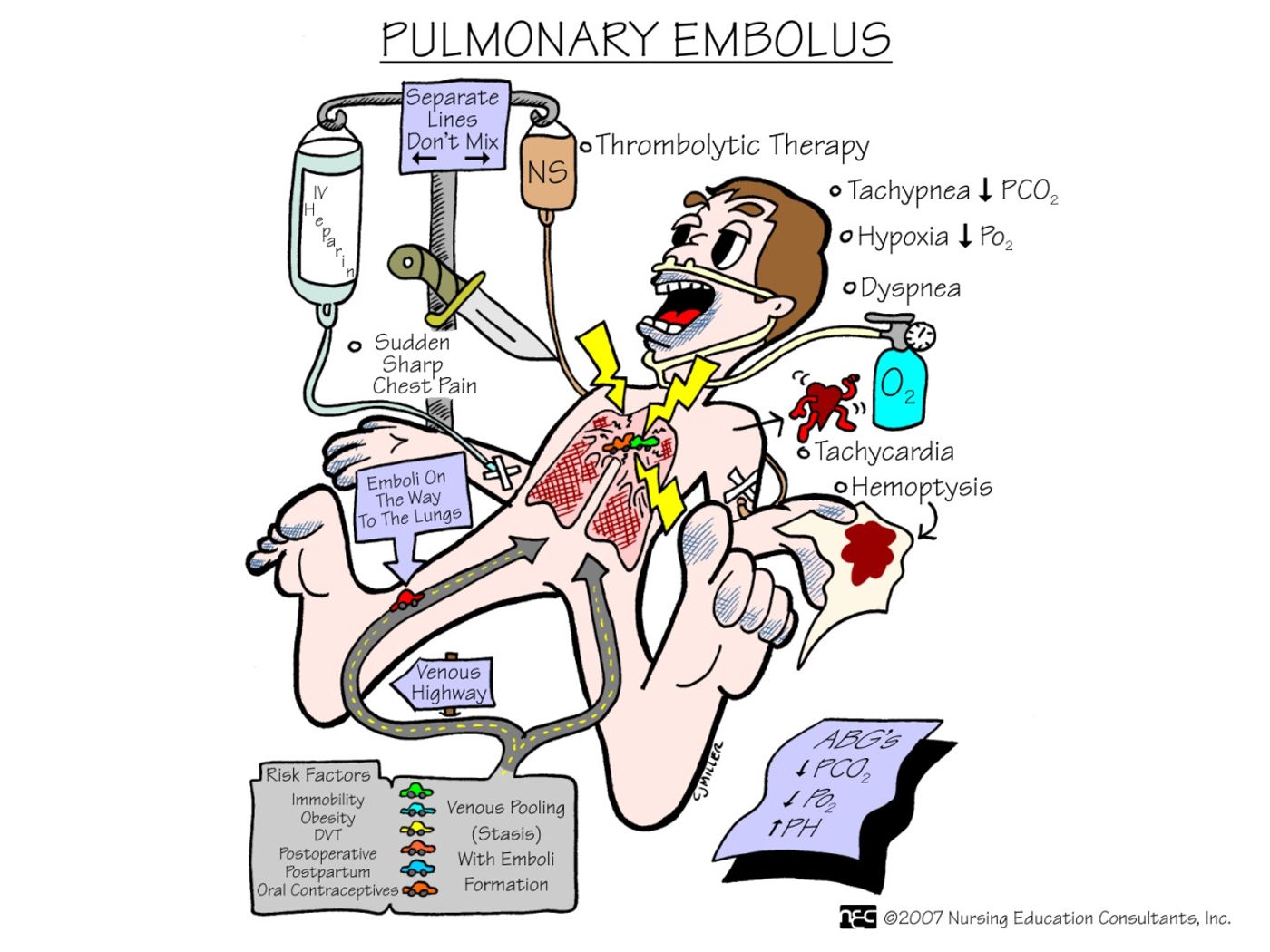
Anticoagulants, or blood-thinning drugs, like heparin work by decreasing the clotting ability of the blood cells by boosting the activity of an anti-clotting protein. Heparin is often used to treat blood clots in many situations, but concerned researchers thought that traumatic brain injury patients might be too vulnerable to excessive, fatal bleeding if a blood-thinning drug were to push them over the edge soon after their injury.
On the other side of the argument, researchers believed that not only was using anticoagulants early on in brain trauma patients, but it was also preventative of future, potentially fatal clotting conditions like deep vein thrombosis (DVT) and pulmonary embolism (PE). Traumatic brain injury patients are likely to remain sitting down for extended periods of time, and combined with their condition, they are at an especially high risk for DVT and PE. Researchers on the early prophylaxis side of the argument wanted to prove that administering anticoagulants 72 hours after hospital arrival and even earlier was both safe and effective for preventing blood clots.
Researchers gathered data from almost three thousand adult patients from the American College of Surgeons Trauma Quality Improvement Program (TQIP), all who experienced severe traumatic brain injury between 2012 and 2014.
“By limiting our cohort to patients with isolated severe traumatic brain injury, we were able to minimize confounding due to other injuries in multiple body regions, while ensuring that our results are generalizable to patients with the most severe head injuries,” said lead study author James P. Byrne, MD.
Did they receive prophylaxis with heparin? Was their treatment early (72 hours after hospital arrival and earlier) or late (after 72 hours)? Did they experience worsening intracranial hemorrhage, DVT, PE, surgical operations 72 hours after hospital admission, or in-hospital death? The researchers asked all of these questions and compared results between “early” and “late” prophylactic treatment groups.
Their results led to their study being the first to ever show the safety of early prophylaxis as well as its ability to lower the risk of PE and DVT: odds of both of the clotting conditions in the early prophylaxis group were 50 percent lower compared to the late prophylaxis group. There was also no difference between the early and late prophylaxis groups per the incidence of neurosurgical interventions or in-hospital death, proving its safety.
Severe brain trauma is very common in patients treated for major injuries at trauma centers, and for the researchers at the American College of Surgeons to confidently say from their findings that early prophylaxis is safe and effective at preventing PE and DVT, it means that many lives will hopefully be saved in the future with the administration of quick blood clot prophylaxis.
This study was recently published in the
Journal of the American College of Surgeons.
Source:
American College of Surgeons,
U.S. Food and Drug Administration,
Circulation