Diagnoses based on genetic testing results from the past ten years may be misdiagnosing some groups of people with a serious heart condition. Scientists from Harvard Medical School have reason to believe it’s due to a lack of racial diversity in control participants from the initial studies that provided the foundation for genetic testing.
Hypertrophic cardiomyopathy (HCM) is a relatively common heart condition that often causes sudden death from cardiac complications in young athletes. Seemingly healthy people with HCM often unknowingly experience a thickening of the heart muscle that often leads to arrhythmias. In their new study published in
The New England Journal of Medicine, Harvard researchers showed how certain benign mutations associated with HCM are much less common in white Americans than in black Americans, an important distinction to be made when reading results from genetic tests.
If early studies, lacking racial diversity, showed that genetic variations relating to HCM are rarely benign, it makes sense that applying those results later to reading results for black Americans led to misdiagnoses. Researchers from the present study looked at more than eight thousand DNA samples from multiple databases. They found that five benign mutations were linked to a large majority of all genetic discrepancies among different populations: between three and 27 percent of black Americans contained these benign mutations in their DNA, while only 0.02 to 2.8 white Americans had them.
"Ensuring that genomic medicine benefits all people and all populations equally is nothing short of a moral imperative, not only for scientists and clinicians but for political and health policy powers that be."
“The findings highlight the importance of interpreting genetic results against diverse control populations to ensure that normal variations of genetic markers common in one racial or ethnic group do not get misclassified as disease-causing in another,” researchers said.
"Our study powerfully illustrates the importance of racial and ethnic diversity in research," says Zak Kohane, M.D., Ph.D., senior investigator on the study. “Racial and ethnic inclusiveness improves the validity and accuracy of clinical trials and, in doing so, can better guide clinical decision-making and choice of optimal therapy. This is the essence of precision medicine."
Kohane and his team also looked at more than two thousand medical records of patients and their family members who received genetic testing between 2004 and 2014. Out of seven patients diagnosed with disease-causing mutations that ended up being later re-diagnosed as benign, five were black and two were of “unspecified ancestry.”
The Harvard study was the first to implicate errors in genetic testing results to “racially biased methodologies in early studies” that aimed to identify the common genetic variants that lead to HCM.
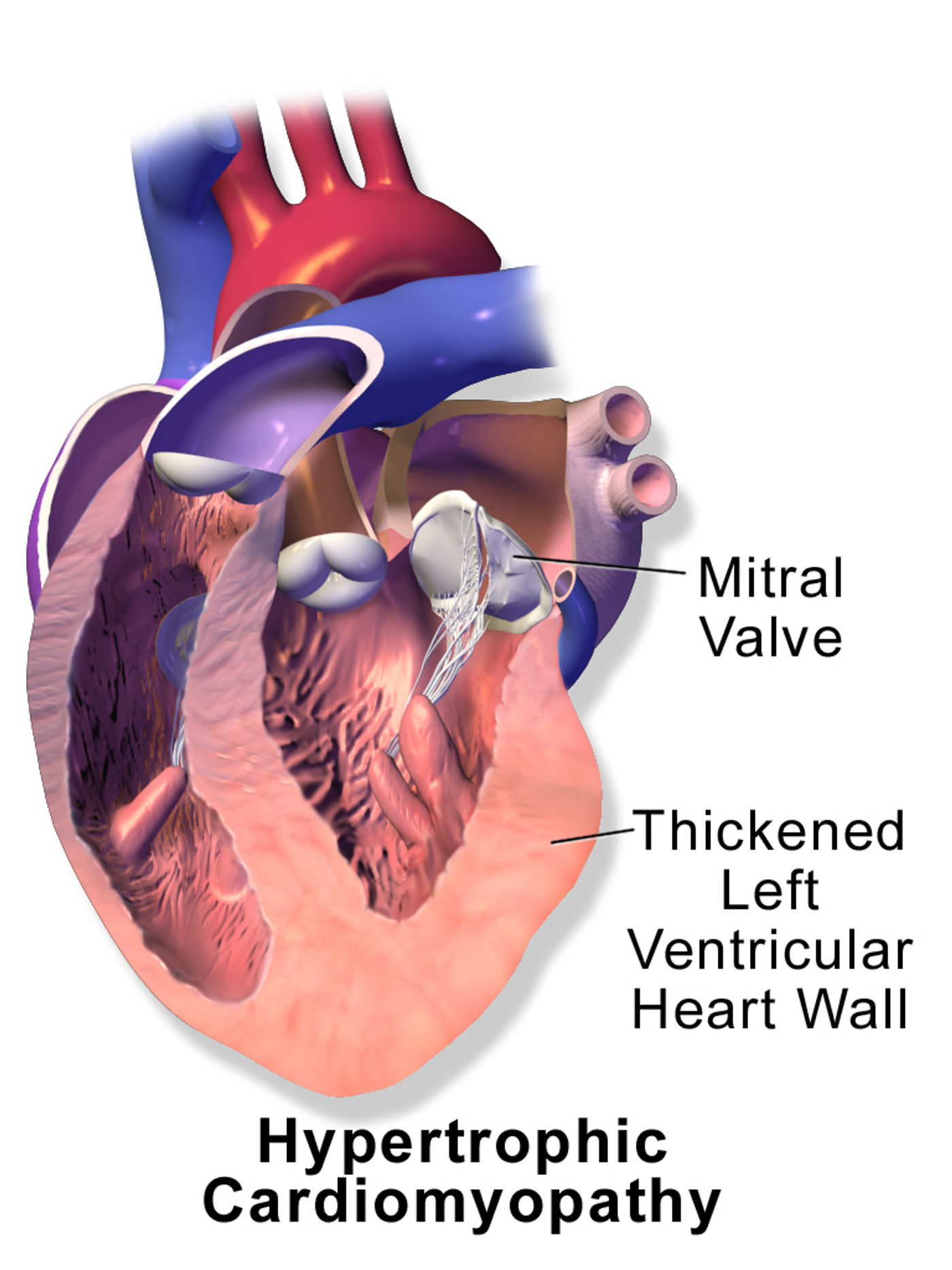
Based on statistical simulation studies, the Harvard researchers estimate that adding 20 black participants to a sample of 200 people would have a 50 percent chance of correctly diagnosing a false-positive. Increase the number of black participants to 67, and the chances increase to 80 percent. Make half of the study participants black, and the results have more than a 90 percent chance of correctly identifying a benign mutation.
Based on their research from the original five studies that provided the basis for translating genetic test results, researchers said: “All of them analyzed small population sizes, and none indicated that black people were included in the control groups.”
It is likely that recent and future studies will include more diverse participants, but until new precedents are set, researchers from the study strongly encourage doctors to rethink the data they use to compare genetic test results, not just for HCM but for other genetic diseases.
"Ensuring that genomic medicine benefits all people and all populations equally is nothing short of a moral imperative, not only for scientists and clinicians but for political and health policy powers that be," Kohane said.
Sources:
Harvard Medical School,
American Heart Association
Images: Time.com, cardiacgenetic.com