First-Ever Genes Discovered to Cause Rare Congenital Heart Defect
For the first time, scientists discovered a genetic culprit for a severe congenital heart defect, hypoplastic left heart syndrome (HLHS). From the University of Pittsburgh School of Medicine, researchers found that two interacting genes, Sap130 and Pcdha9, are equally to blame for cases of HLHS, which affects two to three babies out of every ten thousand born.
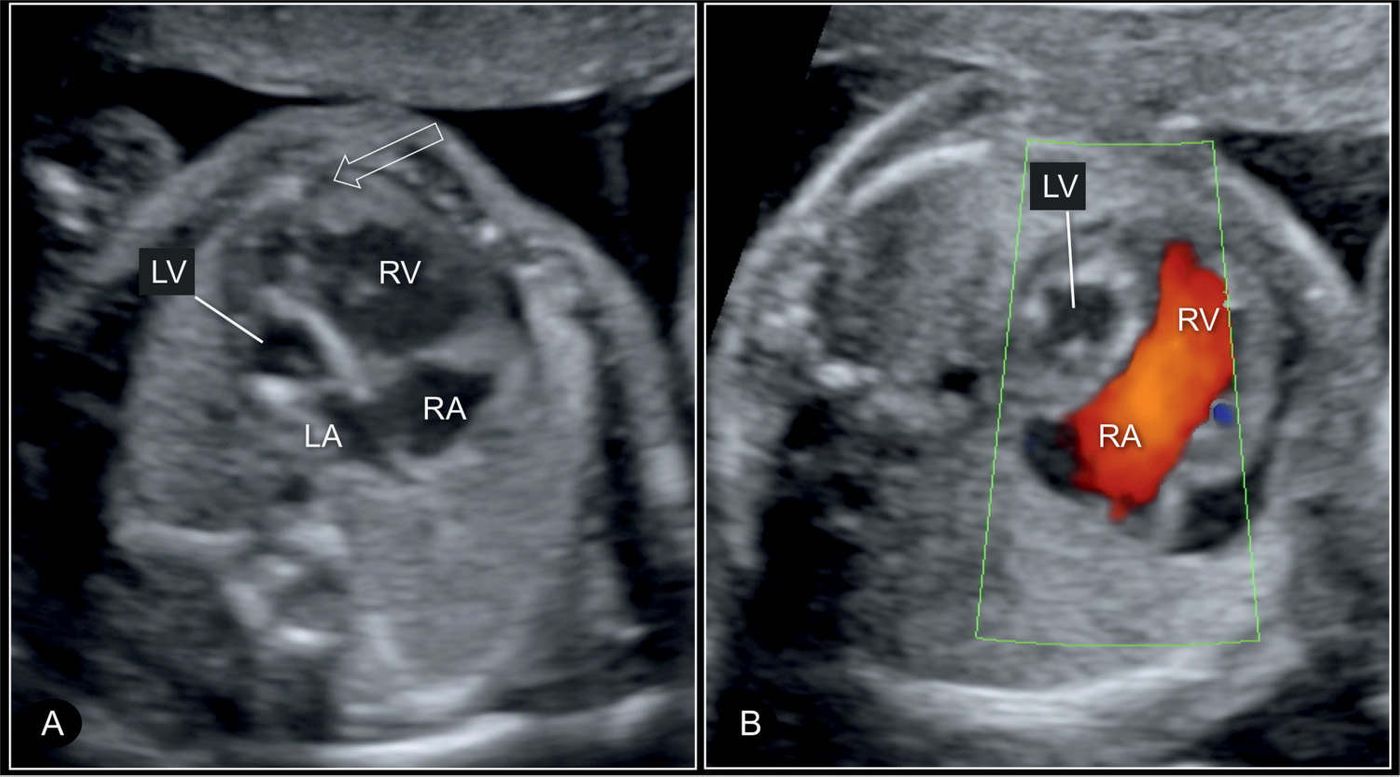
HLHS occurs when the left side of the heart, the ventricle and atrium receiving oxygen-rich blood from the lungs, is poorly developed, which results in a failure to adequately pump blood - carrying oxygen and nutrients - to the body. Experts at Cincinnati Children’s Hospital Medical Center suggest that HLHS is the most challenging congenital heart defect for doctors to manage. Multiple complex surgeries after birth are sometimes effective, but not always. The only option after several failed procedures would be heart transplantation.
Before there could be the first discovery of a genetic culprit, there had to be the first mouse models of HLHS. "Studying diseases with complex genetics is extremely challenging,” explained Pittsburgh’s Cecilia Lo, PhD. “Our study has been made possible by leveraging findings from a large-scale analysis in mice to recover mutations causing congenital heart defects.”
Researchers used fetal ultrasound imaging to scan for structural heart defects in relation to intentionally induced genetic mutations in mice. Then, they could compare mutated and normal mice genomes. After sifting through the data, they found the two genes acting in combination to cause HLHS: Sap130 and Pcdha9.
Sap 130 and Pcdha9 appear to work as a team; both gene mutations are required to produce the structural changes that characterize HLHS, though Pcdha9 mutations occurring alongside normal Sap130 caused some aortic defects. This, explained the first author on the study Xiaoqin Liu, MD, PhD, suggests “interaction between the two genes is needed to cause all the features of HLHS.”
Researchers confirmed their findings with CRISPR-Cas9, a gene editing technology. Now, the investigation is continuing with the potential of finding additional genetic mutations that contribute to HLHS pathogenesis. This provides hope to the families affected by HLHS, which is fatal if left untreated.
The present study was published in the journal Nature Genetics.
Sources: Cincinnati Children’s Hospital Medical Center, University of Pittsburgh Schools of the Health Sciences