Rheumatic Heart Disease in 1990: Then and Now
Worldwide, the risk of dying from rheumatic heart disease has dropped since 1990, but the statistics have hardly changed in some poor populations. Rheumatic heart disease is preventable with antibiotics, yet it still devastates many communities. What can be done?
In a new study from scientists at the Institute for Health Metrics and Evaluation (IHME) at the University of Washington, published in the New England Journal of Medicine, researchers hope to answer that question.
Rheumatic heart disease is the end result of a common bacterial infection, one that many people remember from their childhood: strep throat. More specifically, rheumatic heart disease occurs due to an untreated or maltreated streptococcal infection. Rheumatic fever, the stage between strep throat and rheumatic heart disease, starts showing symptoms between one and six weeks after the initial streptococcal infection.
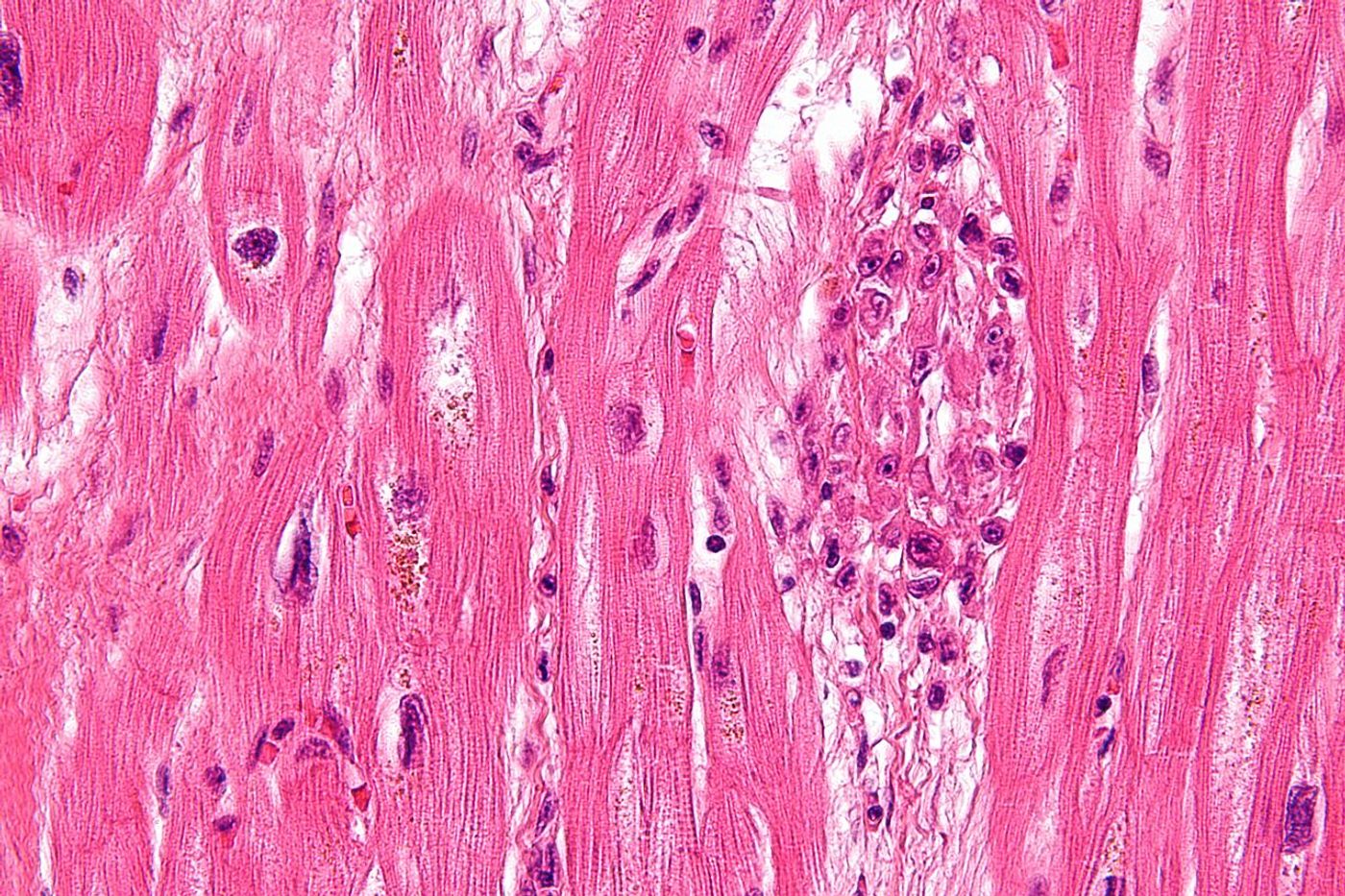
Once the infection begins causing permanent damage to the heart valves, it’s referred to as rheumatic heart disease. This stage can lead to heart failure because the heart has to work harder to make up for the valve damage. Together, rheumatic fever and rheumatic heart disease can cause the following symptoms:
-
fever
-
swollen joints
-
joint pain
-
red rash
-
chest discomfort
-
weakness
Rheumatic heart disease can be diagnosed with an echocardiogram, electrocardiogram, chest X-ray, cardiac MRI, and/or blood tests. There are surgical procedures to treat the disease, mainly to repair or replace damaged valves. Rheumatic heart disease is particularly dangerous for pregnant women, who can experience pregnancy complications if they develop the condition. Other complications for people with rheumatic heart disease include bacterial endocarditis and a ruptured heart valve.
"We have very cost-effective interventions that treat strep throat and prevent rheumatic fever and rheumatic heart disease from getting worse, but [individuals] often don't have access to the care they need," explained lead author Dr. David Watkins. “As a result, their heart conditions usually get worse with age and lead to premature death. Many of these individuals could be saved by open-heart surgery to repair or replace damaged valves, but unfortunately in [poorer] countries access to advanced cardiac surgery care is very low."
Watkins’s study reports that in 1990 there were 346,500 deaths from rheumatic heart disease, 319,400 deaths in 2015 - an eight percent decrease. Countries with the highest estimated death rates include:
-
Central African Republic
-
Federated States of Micronesia
-
Fiji
-
India
-
Kiribati
-
Lesotho
-
Marshall Islands
-
Pakistan
-
Papua New Guinea
-
the Solomon Islands
-
Vanuatu
Watkins and other scientists involved in the study call for better data and more studies of people in countries at a high-risk of rheumatic heart disease mortality.
"It is a tragedy that, in [present day], rheumatic fever remains a serious health concern for so many people,” said senior author Dr. Gregory A. Roth. "The persistence of rheumatic fever and rheumatic heart disease reflects the challenges many countries face in improving the social, environmental, and economic conditions that lead to the disease."
Sources: Johns Hopkins Medicine, Texas Heart Institute, Institute for Health Metrics and Evaluation