Heart Cells Sense Tension and Contraction in Heart Disease
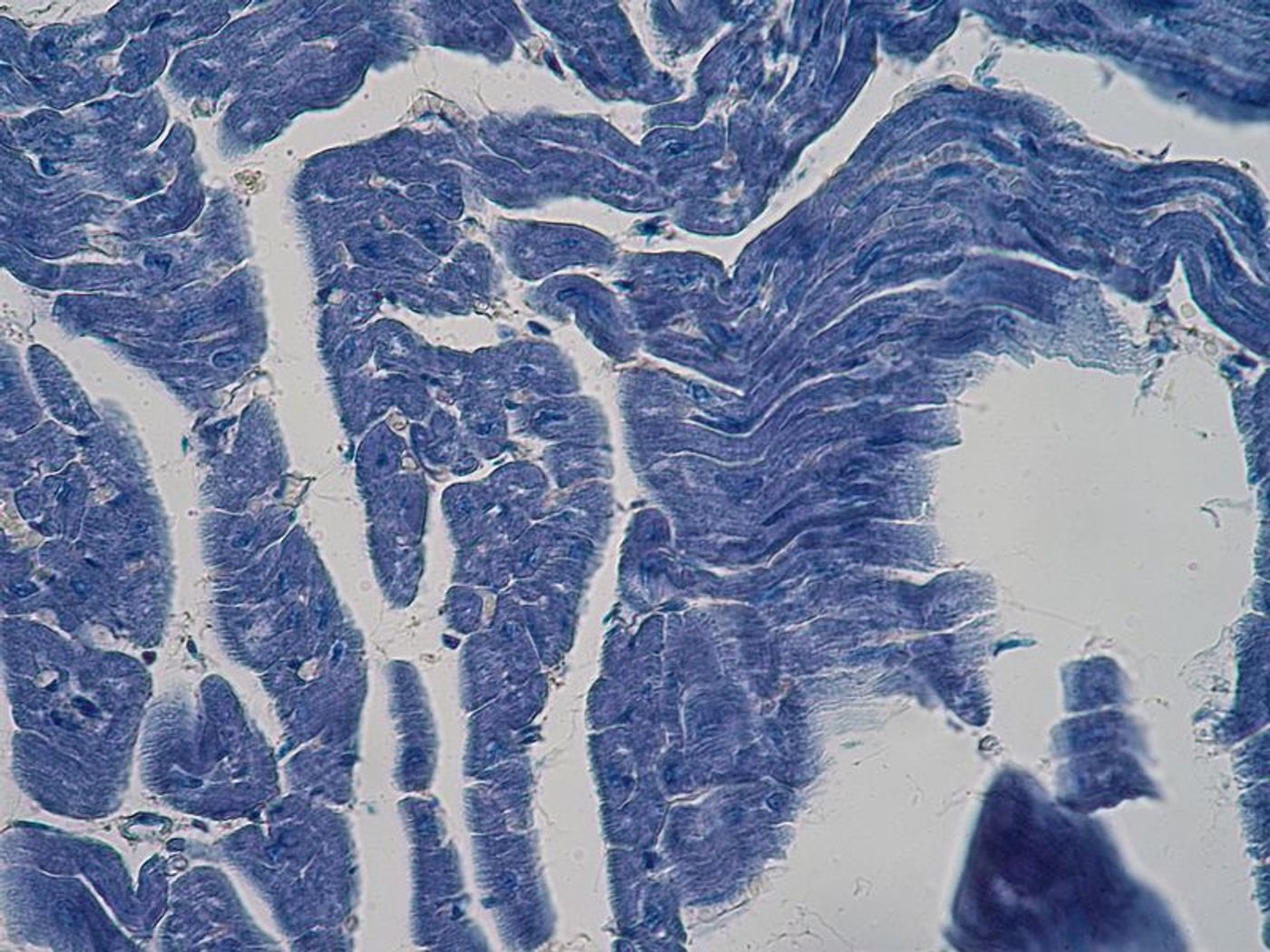
After a heart attack, heart cells lose sensitivity. According to recent discoveries from Queen Mary University of London, this means that heart cells lose their ability to effectively sense stiffness and tension. Normally, heart cells can sense both simultaneously. But loss of sensitivity after a heart attack inhibits this and promotes the progression of heart disease.
The new study mainly focused on how heart cells use adhesive structures to sense stiffness - through muscle contractions - and resting tension, which increases after heart disease, like a heart attack. Without the right sensing abilities, cells tend to “misread the properties of their environment.”
“On the one hand [a heart attack] changes the mechanical properties of the heart and on the other hand it changes how heart cells measure and respond to these properties,” explained lead author Thomas Iskratsch.
Why is it beneficial for heart cells to accurately sense stiffness in their cellular environment?
Obtaining accurate information on the stiffness of heart cells’ environment helps them direct key cellular processes, such as migration to different tissues, differentiation into different cell types, and necessary cell death. Organs can change stiffness during development, over time, or as a result of disease. Abnormal stiffness in the heart negatively affects the way heart muscle cells work together, beating to pump blood.
How do heart cells use adhesive structures to sense contraction and tension?
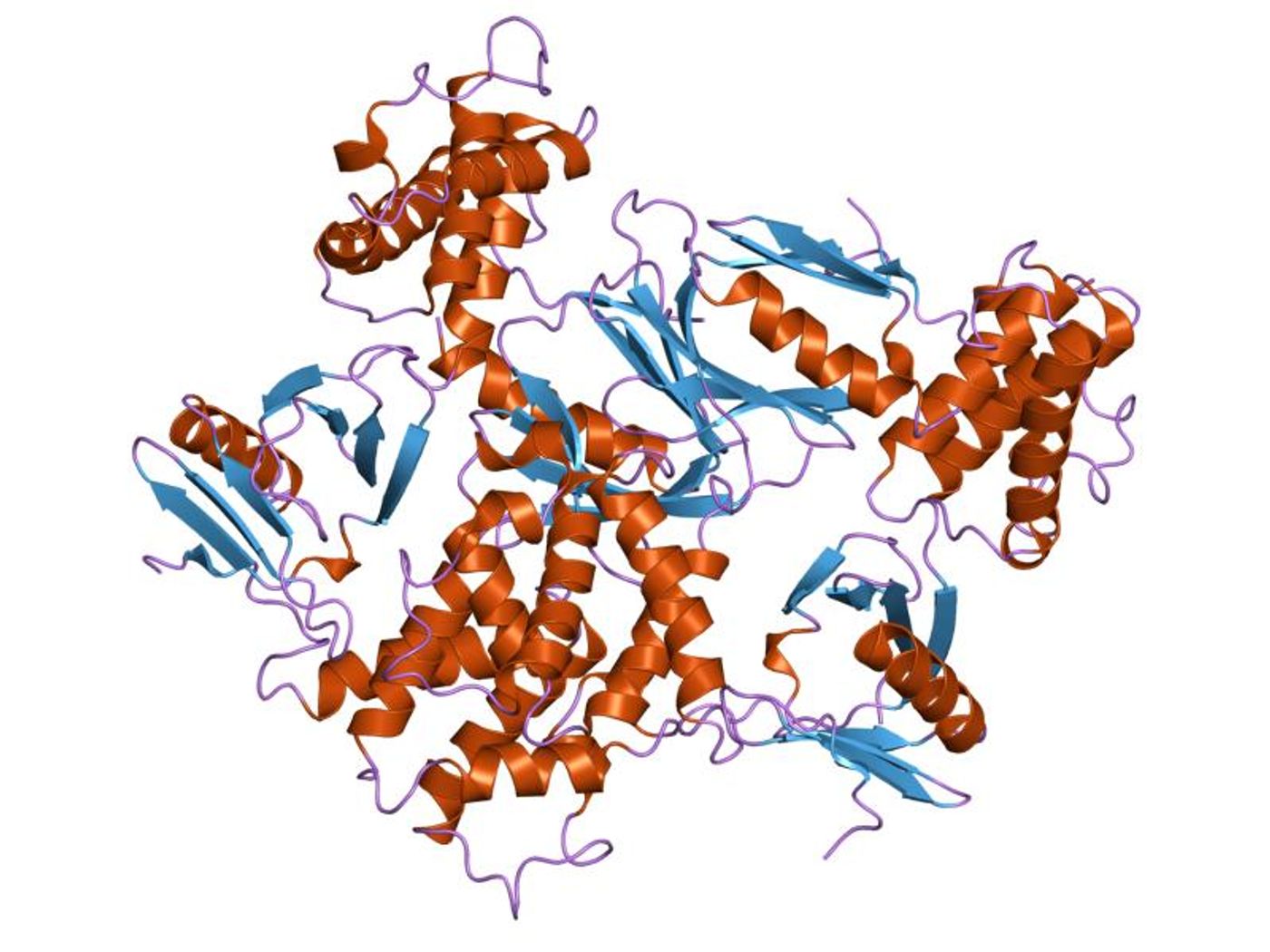
Just as important as sensing contraction and tension in the heart muscle is the stretching of a mechanosensitive protein called talin, which researchers say occurs as a result of the mechanical force used by heart cells’ adhesive structures. When talin stretches, adhesions get stronger, and signals are sent to the nucleus to change the activity of the cell.
Either cyclic, continuous, or no stretching of talin occurs based on the stiffness of the cell environment. As resting tension increases as a result of heart disease, the balance between cyclic and continuous stretching of talin becomes disrupted.
"Further steps are needed to investigate how the different types of talin stretching are translated into changing the cell behavior,” Iskratsch said. “Also, more experiments are needed to observe the changes in mechanical sensing in the diseased heart. Together this will allow the identification of targets for new drugs."
The present study was published in the journal Developmental Cell.
Sources: Methods in Molecular Biology, Queen Mary University of London