Cell Therapy Improves Muscular Dystrophy in More Ways Than One
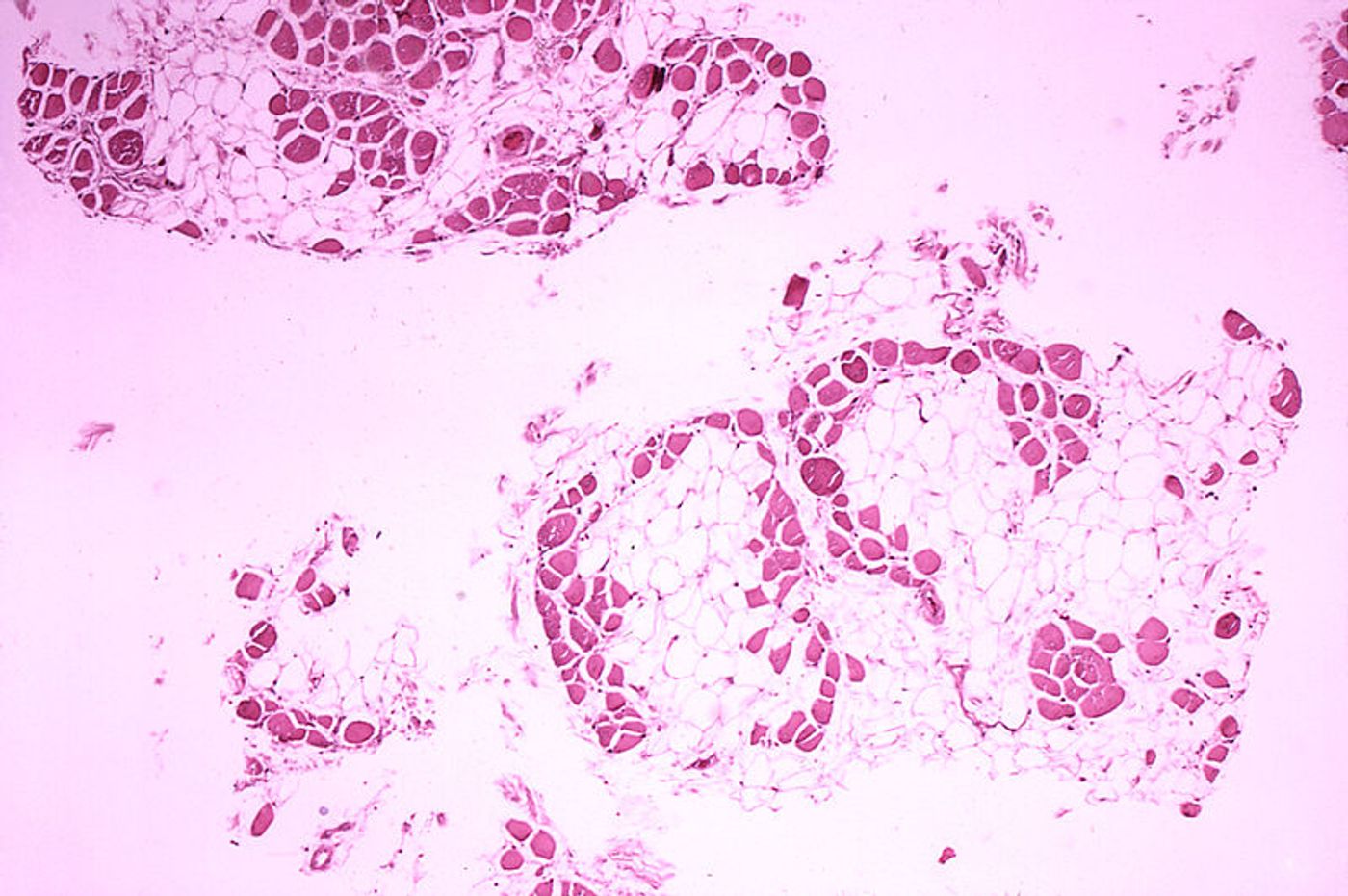
A genetic disorder that causes progressive muscle degeneration is mostly visible because of the toll it takes on young patients, who eventually lose their ability to walk. However, the disorder, called Duchenne muscular dystrophy (DMD), also affects another muscle that’s not so visible: the heart.
In a new study from Cedars-Sinai Medical Center, scientists learned that by treating the parts of DMD that impact the heart, they could also treat other parts of the disease that affect other muscles in the body. The new treatment approach involves injecting cardiosphere-derived cells (CDCs). After successful results in mouse models, clinical studies with human patients are well underway.
The cardiosphere is a place rich with “primitive, proliferating cells” like cardiac progenitor cells. These are the ancestor cells that differentiate into different cell types. In the new study, researchers injected CDCs into the hearts of mouse models of DMD. Both heart function and exercise capacity improved.
"We unexpectedly found that treating the heart made the whole body better," explained Eduardo Marbán, MD, PhD. "These basic findings, which have already been translated to clinical trials, rationalize why treating the heart may also benefit skeletal muscle function in boys and young men with Duchenne."
DMD, a neuromuscular disease, affects males almost exclusively, impacting about 1 in 3,600 boys. Progressive muscle weakness is the hallmark of the disease, a result of a deficiency in a protein called dystrophin. Those affected by DMD usually do not live past 25, and the cause of death is often heart failure because muscles in the heart lose their ability to adequately pump blood to the body’s tissues.
"We found that after receiving CDCs, the lab mice had elevated levels of dystrophin, which likely enabled easier movement and improved survival," explained one of the study’s primary investigators, Ronald G. Victor, MD. "Even just adding a small amount of dystrophin would make a tremendous difference for these young patients."
The study also produced a surprising set of additional results. While the beneficial effects of CDC injection remained even when CDCs disappeared from the heart over time, levels of dystrophin only increased temporarily.
Looking for an explanation, researchers discovered that exosomes secreted by the CDCs were responsible for the long-lasting effect of the drug, despite the fact that dystrophin levels eventually returned to their below-normal state when the cells left the heart. Nearly every cell in the body produces exosomes, which facilitate communication between other cells.
With a clear understanding of the connection between CDCs, dystrophin, and exosome secretion, researchers are going forward with clinical trials in human DMD patients. The first clinical study, conducted last fall, was the first study to test cell therapy in the context of DMD. Researchers saw improved arm strength in the participants, treated with single-dose CDC injections directly into the heart. The next clinical study will be even larger, to begin later this year. Patients will instead receive multiple cell infusions over the course of a year via an intravenous drip.
The present study was published in the journal Stem Cell Reports.
Sources: The Muscular Dystrophy Association, Cedars-Sinai Medical Center, Stem Cells International