Loss of Brain Lesions may Indicate Worsening MS
Doctors that monitor patients with multiple sclerosis (MS) have been using magnetic resonance imaging (MRI) to help treat the disease and determine outcomes. Expanding brain lesions are thought to indicate progressive, worsening MS. However, scientists at the University of Buffalo have now found that the disappearance of these lesions as they waste away into cerebrospinal fluid (CSF) is probably an indicator of disability.
Researchers completed this study of 192 patients over five years and reported it in the Journal of Neuroimaging. Their findings were similar to results from a ten-year study involving 176 patients, presented at this year’s annual meeting of the American Academy of Neurology (AAN).
"Using the appearance of new brain lesions and the enlargement of existing ones as the indicator of disease progression, there was no sign of who would develop disability during five or ten years of follow-up, but when we used the amount of brain lesion volume that had atrophied, we could predict within the first six months who would develop disability progression over long-term follow-up,” noted Robert Zivadinov, MD, PhD, senior author of the five year project and first author of the ten-year study. Zivadinov is a professor of neurology and director of the Buffalo Neuroimaging Analysis Center (BNAC) in the Jacobs School.
Brain lesions are seen as a bad sign in general and can accompany disease or trauma. These lesions are found in MS patients, who routinely receive MRI scans as part of their care. Loss of the lesions might be interpreted as a positive sign, noted Zivadinov. In MS, the protective sheath around neurons is lost, so new growth of those sheaths could indicate repair.
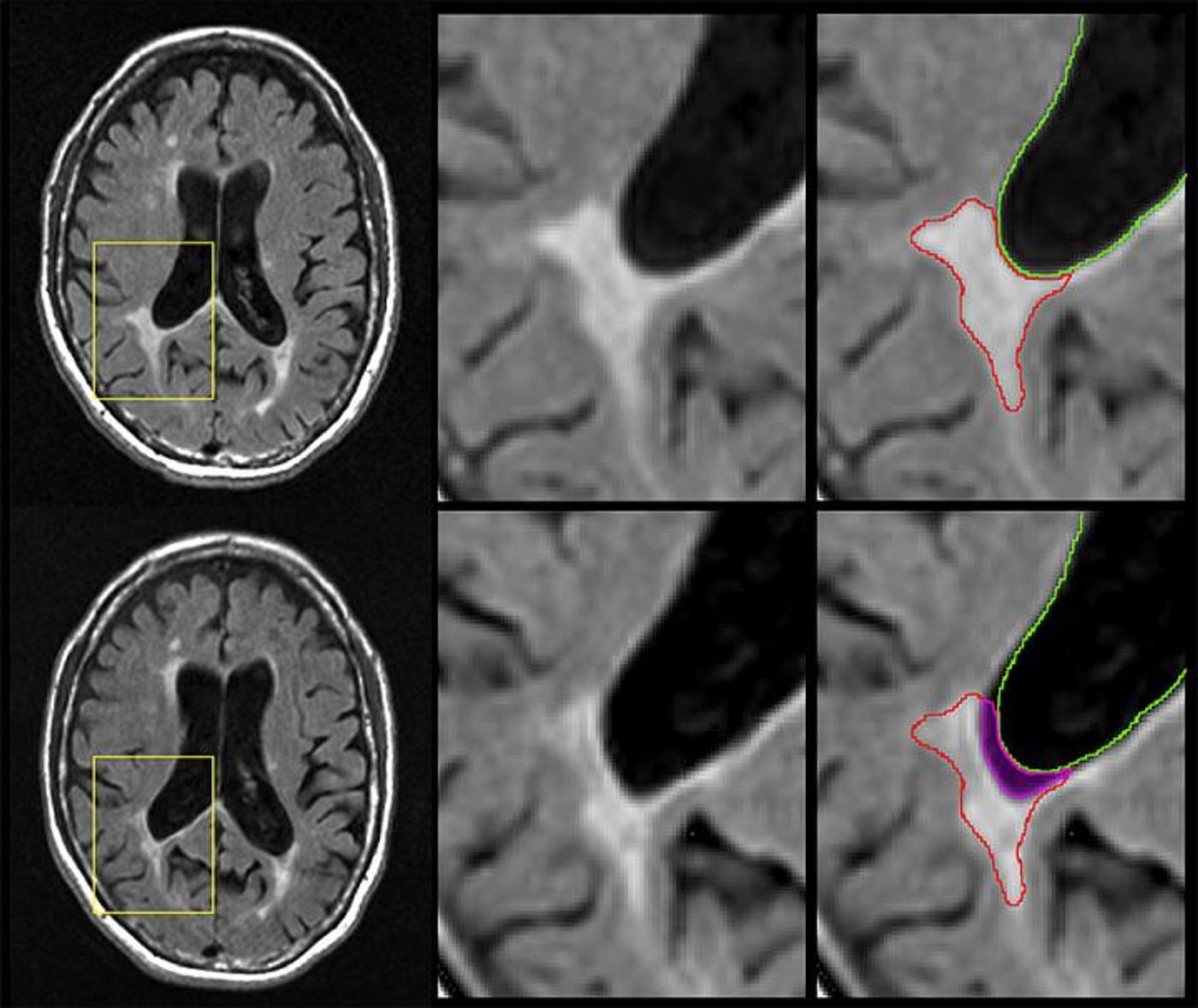
In this work, the investigators looked at lesions that were not replaced by neurons with new sheaths, but instead, neurons that were replaced by CSF. "How do we know the lesions have disappeared?" queried Zivadinov. "Because where there was brain lesion tissue before, there now is just fluid."
"The big news here is that we did the opposite of what has been done in the last 40 years," noted Michael G. Dwyer, Ph.D., assistant professor of neurology and bioinformatics in the Jacobs School and first author on the five-year study in the Journal of Neuroimaging. "Instead of looking at new brain lesions, we looked at the phenomenon of brain lesions disappearing into the cerebrospinal fluid."
The researchers linked a decrease in the size of lesions with a greater number of physical problems in MS patients. "We didn't find a correlation between people who developed more or larger lesions and developed increased disability," said Dwyer, "but we did find that atrophy of lesion volume predicted the development of more physical disability."
The biggest number of lesions were seen in those with a type of MS called relapsing-remitting, but in the most severe class, progressive MS, there was the fastest rate of atrophy in brain lesions. That could make imaging those lesions a critical biomarker for types of MS.
"Paradoxically, we see that lesion volume goes up in the initial phases of the disease and then plateaus in the later stages," said Zivadinov. "When the lesions decrease over time, it's not because the patient lesions are healing but because many of these lesions are disappearing, turning into cerebrospinal fluid."
The scientists also found that atrophy in brain lesions was a better way to predict disability than atrophy in the entire brain, which is the most common way to assess MS.
"Our data suggest that atrophied lesions are not a small, secondary phenomenon in MS, and instead indicate that they may play an increasingly important role in predicting who will develop a more severe and progressive disease," Zivadinov concluded.
Sources: AAAS/Eurekalert! Via University of Buffalo, Journal of Neuroimaging