COVID-19 Attacks Endothelial Cells
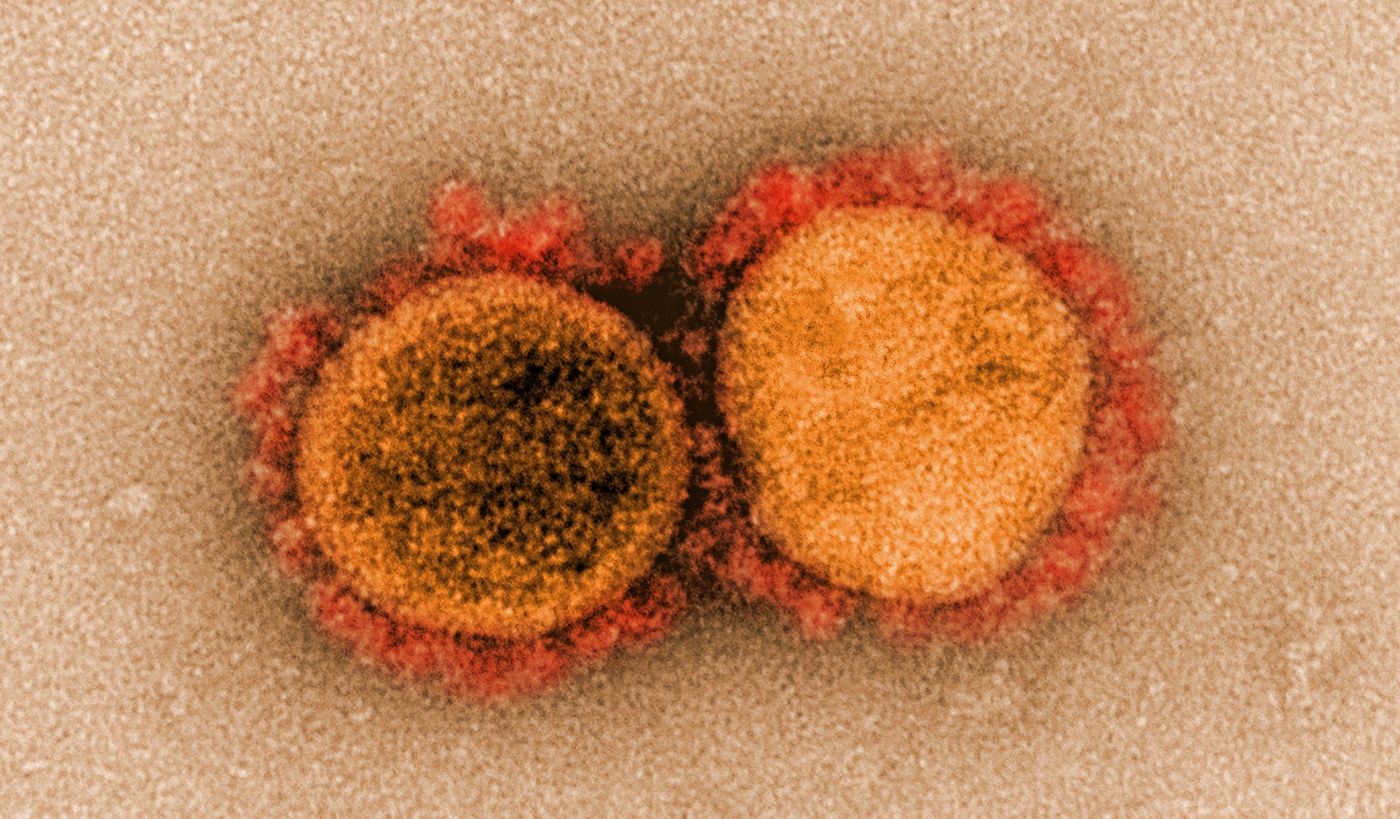
The pandemic virus SARS-CoV-2 can enter the body via cells in the nose to cause the illness COVID-19. But we know now that it doesn't stop there. Clinicians and scientists have found that it can attack many different organ systems. Researchers now are starting to catalog the ways that it can affect the cardiovascular system.
In mid-April, Frank Ruschitzka, leader of the cardiology department at University Hospital Zürich, noticed that COVID-19 patients had symptoms that went way beyond the respiratory system. Some had acute kidney failure, damage to different organs, and blood clots. Autopsies revealed little blood clots in the capillaries in the lungs, which help exchange gases there. Inflammation was also observed in blood vessels ferrying oxygen to every organ. Ruschitzka and his pathologist could see that the virus was targeting blood vessels.
Dozens of other studies have since confirmed and expanded on those findings. Researchers have reported seeing similar vascular damage in COVID-19 fatalities.
This is not just something viruses do, either; a report published in The New England Journal of Medicine determined that COVID-19 victims had nine times more blood clots in their lungs than patients that died of the H1N1 flu. There also seems to be a 'second phase' of some COVID-19 infections that can be fatal.
That second phase appears to be caused by damage to cells that line blood vessels, especially in the lungs, vascular biologist Peter Carmeliet told Science. When the virus attacks these endothelial cells, they become leaky and blood starts clotting. These events trigger systemic inflammation, which leads to acute respiratory distress syndrome (ARDS), a common cause of death in COVID-19 patients.
SARS-CoV-2 enters the body and infects cells in the lung's air sacs, which move oxygen to the blood. Capillaries lined with endothelial cells surround the air sacs. The virus can get into those cells, triggering some to commit suicide and causing their contents to leak out, and others to become 'activated.' The cell damage and fluids could be filling the air sacs, suggested Carmeliet and colleagues.
The immune system probably then launches a massive response in the lungs, ultimately raising local blood pressure and damaging the endothelial cells even more. Clotting would be initiated to try to repair that damage, but it would be out of control. The clotting can then spread throughout the body in a kind of chain reaction, choking off the blood supply in organs and culminating in inflammation that overwhelms the body. Cytokines move in to destroy the invaders and get rid of debris, but too many may respond, and the cytokine storm can lead to shock and death.
This research can help explain why people with metabolic disorders and cardiovascular conditions have more severe cases; their endothelial cells are already taxed. The study may also help identify treatments. Different patients may also need different drugs, and it will be beneficial for everyone to have many options. That will also reduce the demand for individual drugs.
Scientists are now trying different medications that are anti-inflammatory and others that reduce clotting to treat COVID-19. Statins may also have a good impact, said Ruschitzka, because they improve the function of endothelial cells by reducing inflammation.
Source: Science