These Cells Can Cry Tears
Reporting in Cell Stem Cell, scientists have engineered miniature versions of human tear glands that actually emit tears. These mini-organs or organoids can be used in the research lab as a model of tear glands for scientists that want to know more about tear gland disorders and how to treat them. One day it may be possible to transplant functional organoids into patients to repair damaged or dysfunctional tissue.
Tear fluid is critical for lubricating the cornea, supplying it with nutrients, and preventing bacterial growth. Tears come from the tear gland; there's one above each eye.
"Dysfunction of the tear gland, for example in Sjögren's syndrome, can have serious consequences including dryness of the eye or even ulceration of the cornea. This can, in severe cases, lead to blindness," noted study co-author Rachel Kalmann, an ophthalmologist at the UMC Utrecht (UMCU).
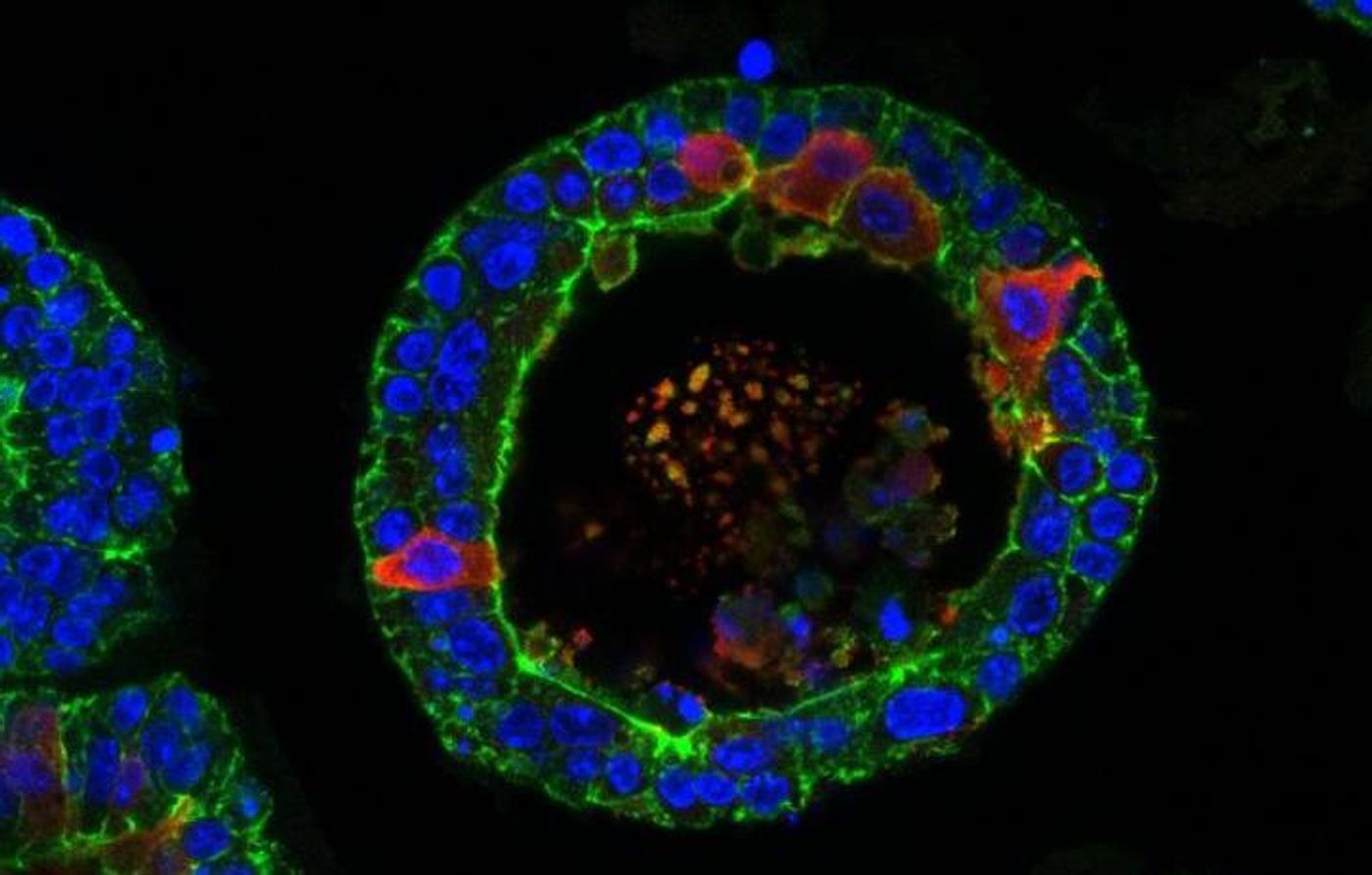
In this work, the researchers generated the first human model of the tear gland. Human and mouse tear gland organoids were grown in culture, and then the researchers set about making them cry. It didn't take humiliation or pain, it just took the right chemical stimulation. These organoids cried when exposed to noradrenaline, for example.
"Organoids are grown using a cocktail of growth-stimulating factors. We had to modify the usual cocktail to make the organoids capable of crying. Our eyes are always wet, as are the tear glands in a dish," explained study co-author and researcher Marie Bannier-Hélaouët.
The tears are shed inside the organoids in an area called the lumen, which makes the organoids swell. The ultimate size of the organoids, therefore, can indicate that tears were generated and released.
"Further experiments revealed that different cells in the tear gland make different components of tears. And these cells respond differently to tear-inducing stimuli," said study co-author and researcher Yorick Post.
While human tear glands are made up of a variety of cell types, these simple models only contain one type of cell right now. The researchers used single-cell sequencing to get a snapshot of which genes each cell was expressing, revealing more about each one's characteristics and generating a cell atlas. This enabled the researchers to identify tear products that can help prevent infection as well.
"In the future, we would like to also grow the other tear gland cell type, so-called acinar cell, in a dish. That way, we can eventually grow a full tear gland in the lab," added Post.
This work could lead to new treatments for patients with tear gland disorders, or cancer of the tear gland.
"And hopefully in the future, this type of organoids may even be transplantable to patients with non-functioning tear glands," Bannier-Hélaouët concluded.
Sources: AAAS/Eurekalert! via Hubrecht Institute, Cell Stem Cell