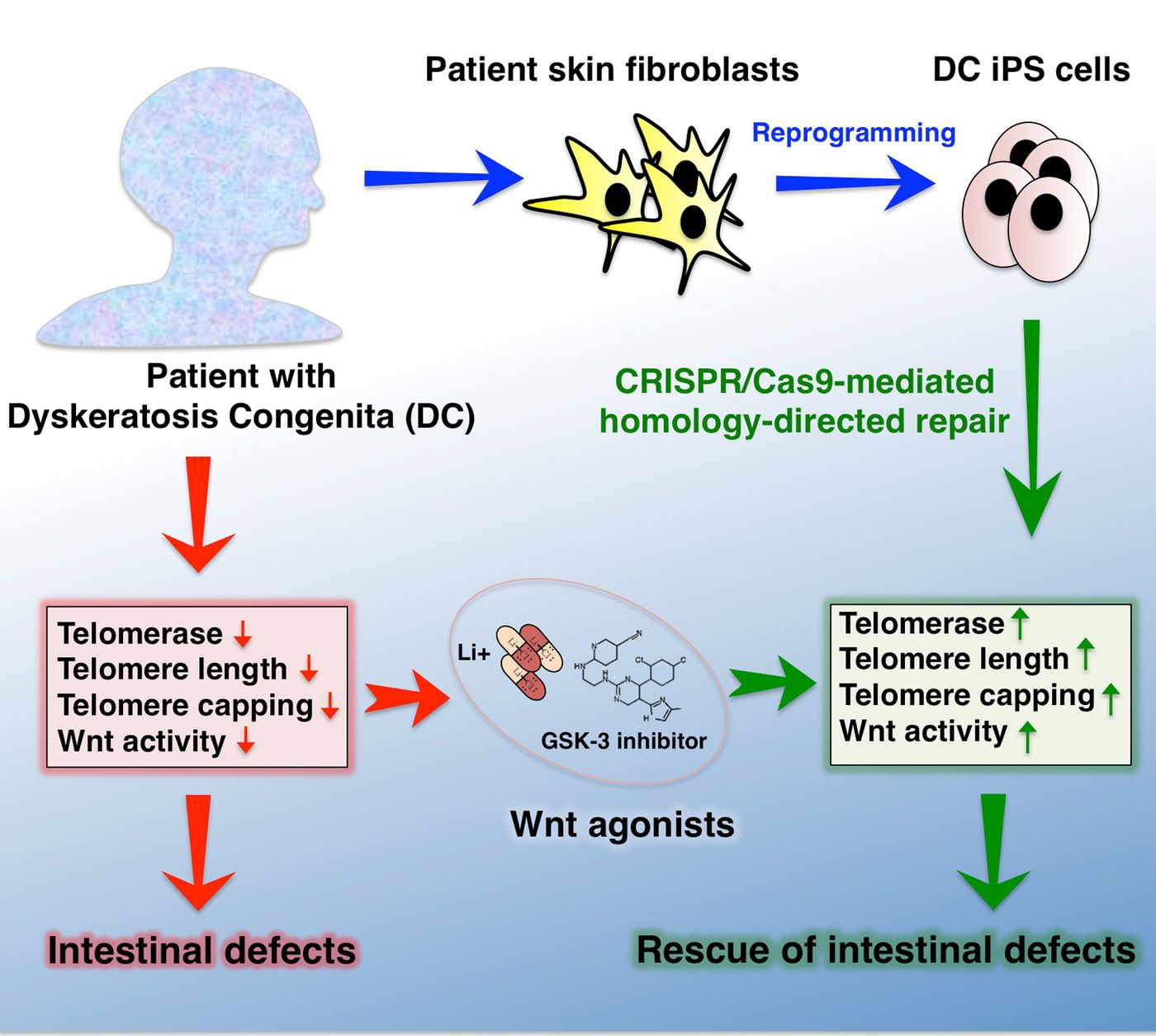
A research team led by Christopher J. Lengner of the University of Pennsylvania School of Veterinary Medicine and Brad Johnson of the Perelman School of Medicine have identified a link between telomeres and a biochemical cascade called the Wnt signaling pathway that could open up new treatment options for patients with telomere dysfunction. They reported their findings in
Cell Stem Cell; the graphical abstract for the paper is seen below.
Telomeres are the capped ends of chromosomes where they have a protective effect, and with every round of cell division, they get smaller. For more information on telomeres, check out the video below. Telomere shortening has been linked to aging and some disease. One such disease is dyskeratosis congenita (DC).
DC is a rare genetic disorder that can impact a variety of parts of the body, and is variable between patients. The three main features of the disease are altered skin pigmentation, poorly growing or misshapen nails, and white patches in the mouth. Other more serious symptoms can occur as well due to the effects the disease has on bone marrow, including increased cancer risk. Many people affected by DC carry a mutation in the DKC1 gene, which is critical to the telomerase enzyme. The clinical guidelines for the disease are discussed in the video below.
Using mice from Johnson's lab, the Lengner and Johnson research groups were able to connect the Wnt pathway to telomeres. They followed up on the finding with human tissues in culture to show that when the Wnt pathway is stimulated, intestinal dysfunction due to DC is reversed. The scientists hope their findings can help fight telomere dysfunction in a broad sense, which could have implications for aging and some cancers.
"What you see in the mutant mice and the dyskeratosis congenita patients is the consequence of having less telomerase activity in rapidly dividing tissues," explained Johnson, an Associate Professor of Pathology and Laboratory Medicine at Penn Medicine and the co-senior author of the study. "It's not the same thing as natural aging where you might have telomere defects in cells that don't have a lot of telomerase activity to begin with. But I think it's fair to say our findings inform an understanding of some of what might be happening as telomeres shorten in aging."
There are currently very few treatment options for DC patients. "Right now the main therapy for these patients is a bone marrow transplant," said Lengner, another co-senior author and an Assistant Professor in the Department of Biomedical Sciences at Penn Vet. "That can address the bone marrow failure but doesn't fix other problems associated with the disease, and especially not the risk of cancer. This work suggests a way to address the underlying cause of the disease."
The investigators knew from previous work that there could be a connection between the Wnt pathway and telomerase. They used a variety of new techniques to delve deeper.
Using induced pluripotent stem cells (iPSCs), reprogrammed adult cells that resemble embryonic stem cells, they were able to alter cells from both DC patients and healthy people in order to create many different types of cells.
The CRISPR/Cas9 gene-editing system was employed to both create a mutation in the DKC1 gene of the healthy stem cells, or to correct the mutation in unhealthy DC-derived cells. Want to know more about the CRISPR/Cas9 system? The video below, featuring one inventor of the technology, explains further. Those various cell lines would allow the researchers to rule out confounding effects from other parts of the genome.
Finally, organoids, or miniature, simplified versions of organs, were grown using the stem cells. In this case, the organ was the intestinal tube. Organoids derived from DC patients were only able to form so much of the tube before the process became dysfunctional and had shorter telomeres. The same thing was observed in organoids made from healthy stem cells that had been mutated. No such problems were seen in the organoids made from healthy individuals, or from DC patients that had been edited with CRISPR.
"We could see at the molecular level that this is accompanied by a failure to activate specific intestinal stem cell gene programs," Lengner explained, "specifically genes in the Wnt pathway." Since the Wnt pathway had been implicated, the researchers wanted to see if it could be an avenue for treatment.
After transplanting the organoids they’d created into mice (for a more clinically relevant model), the mice were treated with a Wnt pathway stimulator, lithium. In lithium-treated mice that received the DC-affected transplant, intestinal tissue structure was maintained. Basically, they were like the mice that got a transplant of an organoid made from a healthy patient.
This led the scientists to conclude that Wnt pathway activation can reverse the gastrointestinal distress caused by DC. They hope to extend these findings into therapies for tissues affected by this disorder.
Sources:
AAAS/Eurekalert! via
UPenn,
Genetics Home Reference,
Cell Stem Cell