Genetic Mutation in Human Embryo is Successfully Corrected
Researchers in the United States have made a breakthrough in gene editing by successfully repairing a deleterious genetic mutation in a human embryo that would otherwise cause a heart defect. This work, reported in Nature now paves the way for fixing disease-causing errors in genes before a person is born, and is sure to stimulate vigorous debates on the ethics of the technology. Learn more about the work, a collaborative effort by the Salk Institute, Oregon Health and Science University (OHSU) and the Institute for Basic Science in Korea, from the video.
"Thanks to advances in stem cell technologies and gene editing, we are finally starting to address disease-causing mutations that impact potentially millions of people," said the corresponding author of the work Juan Carlos Izpisua Belmonte, a Professor in Salk's Gene Expression Laboratory. "Gene editing is still in its infancy so even though this preliminary effort was found to be safe and effective, it is crucial that we continue to proceed with the utmost caution, paying the highest attention to ethical considerations."
Ethical precautions have been paramount when it comes to gene editing technologies in the United States. Belmonte has been a part of laying guidelines for the application of these tools to human embryos; he was one author of 2016’s "Human Genome Editing: Science, Ethics, and Governance" by the National Academies of Sciences, Engineering and Medicine. This work stuck to those recommendations, as well as adhering to guidelines made by the Institutional Review Board of OSHA and other committees established for scientific and ethical review.
This study aimed a known mutation in the MYBPC3 gene, which causes sudden death in young athletes that are otherwise healthy. The disorder is called hypertrophic cardiomyopathy (HCM), and while it is common, impacting around 1 in 500 people, it is not usually detected in time. Carriers can easily pass it to their children, so being able to correct this basic defect could save many lives not only by preventing a person from having a heart problem, but it will also stop it from being passed to the next generation.
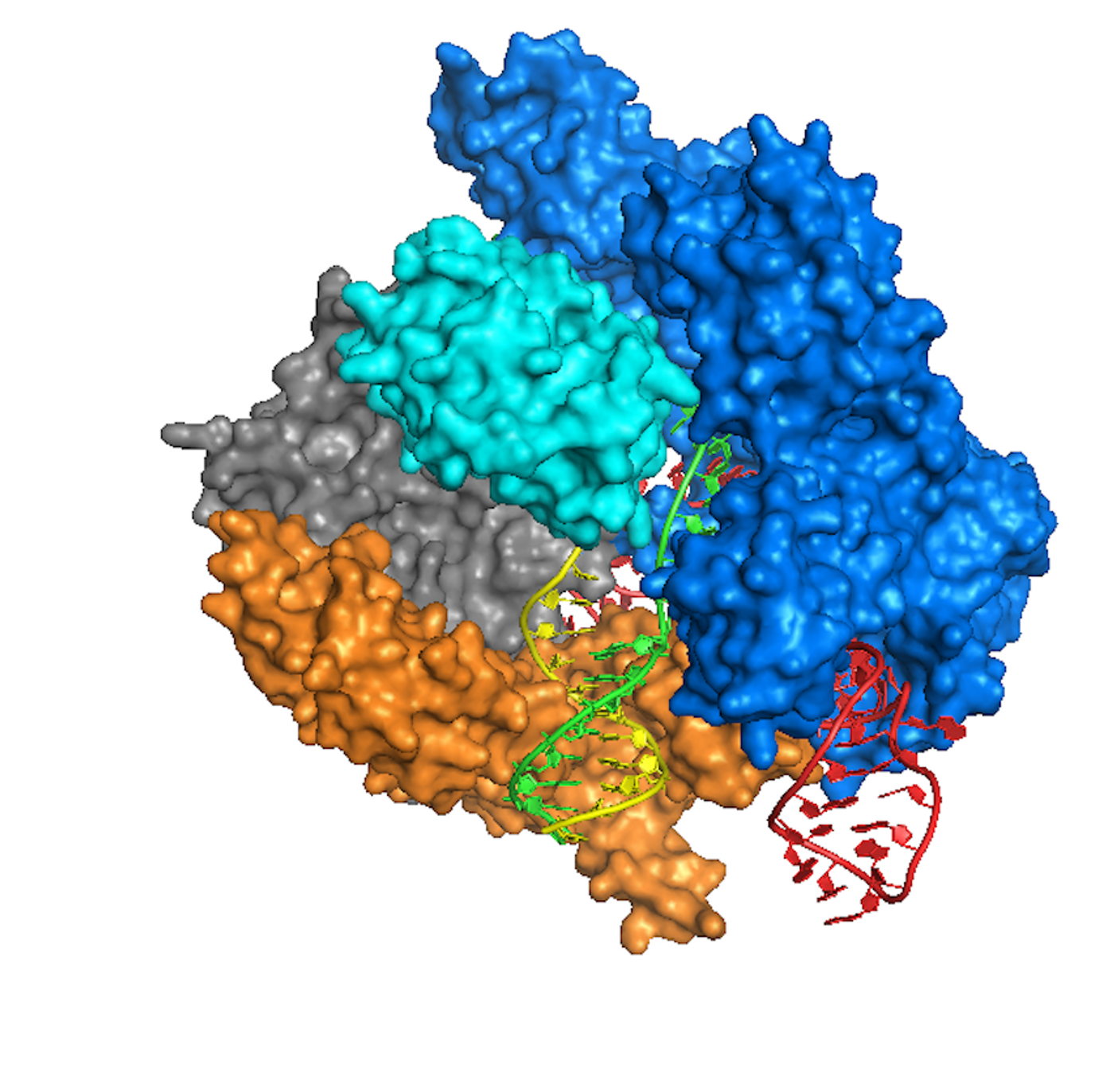
For this work, a man with HCM donated skin cells, and by using standard methods, the researchers created pluripotent stem cells from them. CRISPR-Cas9 gene-editing technology was used as inspiration to repair the mutation: the Cas9 enzyme targeted the mutation, and the repair machinery in the cells corrected it naturally.
After screening for the best results of their work, the gene-editing reagents were mixed with healthy human eggs and sperm donated by the HCM patient. The researchers found that their technique worked very well. Many embryonic cells are fixed and with a very low rate of off-target mutations or negative impacts on the genome.
"Even though the success rate in patient cells cultured in a dish was low, we saw that the gene correction seems to be very robust in embryos of which one copy of the MYBPC3 gene is mutated," said one of the first authors of the work Jun Wu, a Salk staff scientist.
When CRISPR-Cas9 had been applied to the mutated gene copy, it seemed that the embryo began repairs on its own. The embryo did not want to use synthetic DNA that was there and instead preferred utilizing the other copy of the gene - the healthy, normal one - to repair the mutated copy. "Our technology successfully repairs the disease-causing gene mutation by taking advantage of a DNA repair response unique to early embryos," said Wu.
The scientists emphasized that this tool is still in the early stages of development; much more evaluation remains to be done to understand what else may be occurring. It is also not yet known how this might work with other mutations.
"Our results demonstrate the great potential of embryonic gene editing, but we must continue to realistically assess the risks as well as the benefits," noted Izpisua Belmonte.
Sources: AAAS/Eurkealert! Via Salk Institute, Nature