Hypoxia Imaging: Oxygen-Sensitive Probe That Lights Up
Hypoxia, as the name indicates, is a condition in which a part of body experiences a lack of oxygen. Tissue hypoxia arises from various medical conditions from solid tumor to strokes. According to a recent publication in Nature Communication, a group of University of Illinois (UIUC) researchers has come up with a novel diagnostic regime that can help identify hypoxic microenvironment in the human body using a non-invasive and non-radioactive imaging technique.
Striving in an environment that has an inadequate supply of oxygen is considered a hallmark of solid tumors. As tumors have grown in size and form new blood vessels in its microenvironment, a pathophysiologic disturbed microcirculation is formed around them that has little diffusion of oxygen.
Hypoxia does not just happen in cancer. When access to oxygenated blood is blocked, a condition also known as ischemia, insufficient blood flow resulted in inadequate oxygenation. Common causes of ischemia are acute arterial thrombus (blood clot) formation, chronic narrowing of an artery, and atherosclerosis. Acute ischemia, like stroke and heart attack, leads to apoptotic and necrotic cell death.
The current standard method for detecting tissue hypoxia is to insert an oxygen-sensitive electrode into the tissue of interest to take a direct measurement, a very invasive procedure. It is limited by the depth of the potential hypoxic “pocket”. If the location is deep inside the body or blocked by other organs, the electrode approach will not work.
Alternatively, radiologists use nuclear scan like positron emitting tomography, a process that relies on radioactively labeled probes targeting hypoxia-specific biomarkers. It is an expensive procedure and involves a moderate dose of ionizing radiation.
The UIUC researchers developed an oxygen-sensitive molecular probe that has so-called an N-oxide trigger, which can be reduced in the absence of oxygen. The reduction of the probe emits spectrally unique ultrasound signals when comes in contact with light, a process called photoacoustic imaging.
Photoacoustic imaging has the potential to image animal or human organs with simultaneous high contrast and high spatial resolution. This highly promising technique measures unique optical absorption contrasts related to crucial biochemical information and provides better resolution in deep tissues than optical imaging. It is radiation free, non-invasive, and relatively inexpensive, and offers higher resolution 3-dimensional images.
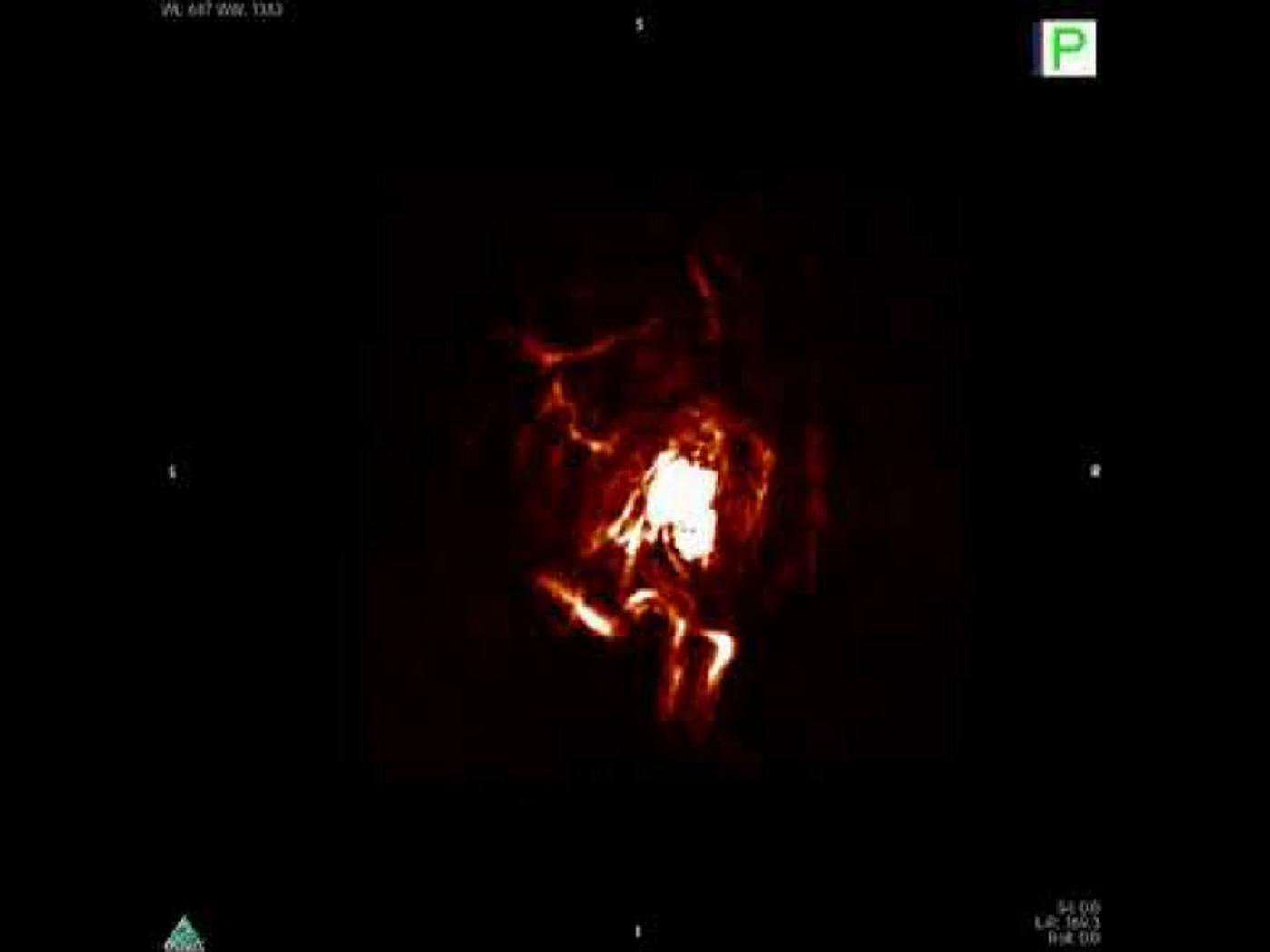
To the researchers’ delight, the oxygen-sensitive probe sent out photoacoustic signals shortly after a hypoxic condition was induced in a mouse's artery, showing promise for swift identification of tissue hypoxia deep inside a human body. In the tumor model, the probes enabled detailed, 3-D ultrasound imaging of hypoxic tumors in mice.
"We could give a doctor a three-dimensional, real-time view into the tissue to guide surgical procedures and treatment plans," commented Chemistry Professor Jefferson Chan, the leader of the study.
"The system that we used in this study is a preclinical system for animals. However, in a clinical setting, you can take a regular ultrasound machine and equip it with a light source - you can buy LEDs for around $200 that is powerful enough and safe for clinical applications," Chan said. Physicians would administer the photoacoustic molecules to the patient, either by injecting into a vein or directly to a tumor site, then use the modified ultrasound machine to visualize the area of interest, he added.
Regarding the potential application of this hypoxia imaging technique in tumor diagnosis, Chan said: "We know that a lot of tumors are hypoxic, so many new treatments have been developed that become activated in oxygen-deficient conditions. But they have been inconsistent in clinical trials, because not all tumors are hypoxic. This gives scientists and physicians a way to noninvasively look inside tumors and determine whether a patient's tumor is hypoxic and they would be a good candidate for a new drug. If the tumor doesn't look very hypoxic, they should go into a different treatment plan."
Photoacoustic imaging of hypoxic tumor. Credit: ChanLab/UIUC
Source: phys.org