'Butterfly Child' Given New Skin Thanks to Gene Therapy
A boy whose extremely fragile skin, like that of a butterfly, has been saved by an experimental therapy. The first-of-its-kind treatment gave the boy new skin thanks to stem cell grafts.
Seven-year-old Hassan is unique in many ways, but it was his skin that defined his life so far. In the first few weeks of life, Hassan’s parents noticed blisters on his back. The diagnosis? An extremely rare genetic disease called epidermolysis bullosa (EB). Patients with EB are also known as the “butterfly children,” a nickname that refers to the fragility of the skin, which can break and blister at even the slightest touch. There is no cure for EB.
For Hassan, the condition meant high risk of infections and other complications, including skin cancer. When his father brought him to the Children's Hospital at Ruhr University in Bochum, Germany in 2015, Hassan was fighting for his life.
"He suffered from severe sepsis [a blood infection] with high fever, and his body weight had dropped to a mere 17 kilograms (37 pounds) — a life-threatening condition,” explained Dr. Tobias Rothoeft, a pediatrician at the Children’s Hospital who treated Hassan, in a statement.
"We had a lot of problems in first days just keeping him alive," said Dr. Rothoeft. They tried various available therapies, including skin transplants, and aggressive antibiotic and nutritional regimens. But none of these treatments could stop the progression of the disease.
"By that time, he had lost 60 percent of his epidermis, the upper skin layer, and had 60 percent open wounds all over his body," said Dr. Maximilian Kueckelhaus of the Department of Plastic Surgery at Bochum's Burn Center.
With little else to turn to, Hassan’s team turned to Dr. Michele De Luca, a stem cell biologist at the University of Modena's Center for Regenerative Medicine in Italy. Previously, the De Luca team had shown success in transplanting skin grafts derived from genetically modified stem cells, which have the ability to turn into any type of tissue.
Even though the technique had only been done in a limited number of adults with small, non-threatening wounds, and Dr. De Luca had given Hassan only a 50 percent success rate, the family viewed the procedure as their only option left.
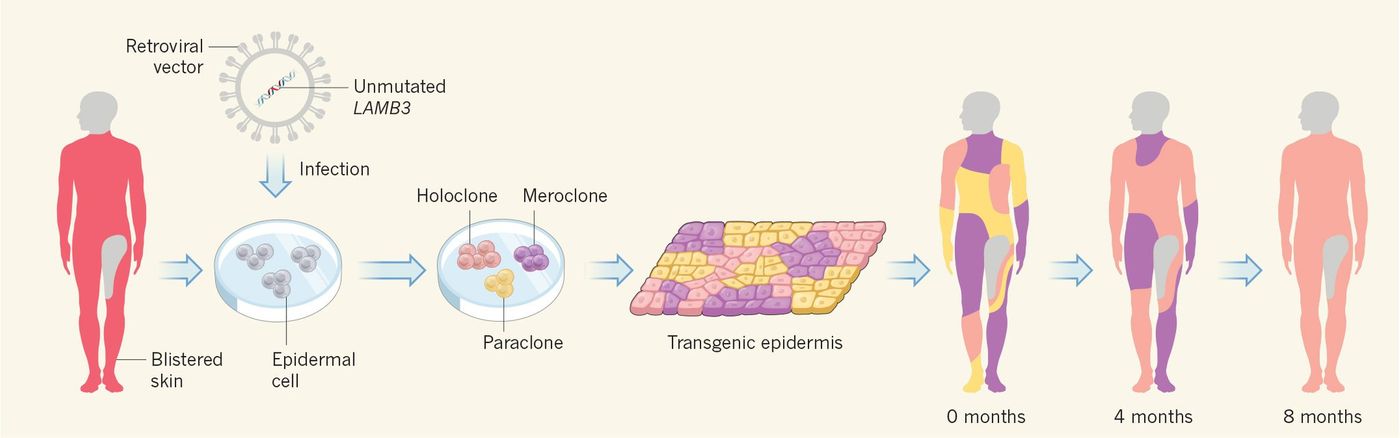
Doctors began by taking from Hassan a small patch of healthy skin, which provided the cells that the De Luca team could then modify. After processing, stem cells with the corrected version of the EB gene were grown on a clear sheet for eventual grafting back on Hassan’s body. It took the team only a month to grow the roughly 1 square meter of stem cell grafts to cover the affected 60 percent of Hassan’s body.
The grafts were transplanted in two sessions in 2015. The first procedure covered his arms and legs, and the second covered his entire back and the remaining affected areas.
The effects were immediate and life-changing. Not only did the grafts not get rejected, they were healing the damages caused from EB.
“For everyone that was involved, taking off the bandages and seeing for the first time that this is working out, that the transplants are actually attached to the patient and growing skin, that's an incredible moment," Dr. Kueckelhaus said.
In a series of checkups that spanned over 21 months, Hassan’s improvements continually amaze his doctors. The boy whose skin was so fragile that it nearly killed him, now had normal skin like any other boy. His new skin is resistant to blisters and tears, has hair, and bruises just like any other skin.
"It felt like a dream for us," Hassan’s father said. "Hassan feels like a normal person now. He plays. He's being active. He loves life."
"The investigators removed of small piece of patient's skin, isolated cells with stem cell potential for growth, introduced a normal copy of the mutated gene to the cells, propagated a large number of these cells in culture and then grafted them back to the skin," said Dr. Jouni Uitto, a professor and chairman of the Department of Dermatology and Cutaneous Biology at the Sidney Kimmel Medical College in Philadelphia, who was not involved with Hassan’s case. "This concept is not new, but what is remarkable here is that they were able to change essentially the entire skin of the patient with normal cells."
Indeed, Hassan is now also unique because he’s the first person in the world to have had 60 percent of his body covered with stem cell skin transplants.
"This approach has enormous potential for research into and development of new therapies for the treatment of epidermolysis bullosa as well as other diseases and trauma causing large skin defects," said Dr. Tobias Hirsch, a plastic surgeon at the Burn Center at Ruhr University, and the study’s lead author.
Additional sources: CNN, Live Science