Injection Improves Corneal Transplant Outcomes
The common form of tissue transplant is the corneal transplant. Corneal transplantation is performed to correct visual loss that has occurred when the cornea, the transparent structure forming the front of the eye, becomes opaque (cloudy) as a result of many eye diseases.
According to a research study in the American Journal of Pathology, Injection of neuropeptide vasoactive intestinal peptide (VIP) directly into the eye of mouse models was found to enhance corneal graft survival. The injection was also found to produce other benefits such as accelerating wound healing, protecting corneal endothelial cells, and improving the corneal graft clarity. If VIP is shown successfully in clinical studies, the novel approach may bring hope to patients who lost their vision due to corneal disease. "The successful outcome of corneal transplantation mainly relies on the density and function of CEnCs, which keep the graft transparent. To improve the outcomes of corneal transplantation, various strategies have been employed to prevent immune-mediated graft rejection or enhance survival and function of CEnCs. However, an effective method has remained elusive so far," explains Dr. Ahmad Kheirkhah of the University of Texas San Antonio. During the study, researchers evaluated the effect of VIP on corneal tissue in cell culture and living animals who received corneal transplants.
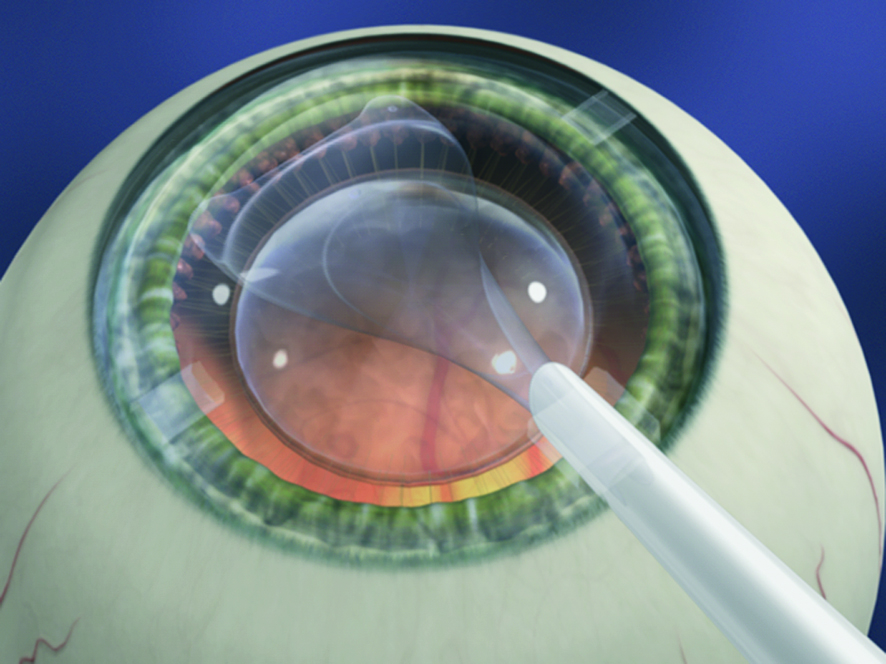
VIP is a 28-amino acid neuropeptide found in the aqueous humor of the eye and may be secreted by corneal endothelial cells. It is recognized as a protection and immunoregulation factor in multiple organ systems. In mice that underwent corneal transplantation, grafts were more transparent in VIP-treated mice comparison to the controls. After eight weeks since transplantation, 85 percent of VIP-treated grafts have survived in comparison to only 0 percent of control grafts. Additionally, corneal endothelial cell density was higher in VIP-treated corneas than controls. "Millions of patients around the world are blind due to corneal opacity, and they are in dire need of corneal transplantation. Unfortunately, there is a significant shortage of donor corneas across the world. On the other hand, many donated corneas cannot be used for transplantation due to inadequate endothelial cells. Moreover, corneal transplants can deteriorate over time due to continuous loss of CEnCs," noted Reza Dana, MD, MPH, MSc, Professor of Ophthalmology at the Massachusetts Eye and Ear, Department of Ophthalmology, Harvard Medical School, Boston, MA, USA. "If confirmed in further clinical studies, we believe that the use of VIP will increase the number of donated corneas suitable for transplantation and improve the outcomes of corneal transplantation."
Source: Elsevier
-
MAY 07, 2024Is It Anti-RNP or Anti-Sm/RNP?
-
MAY 08, 2024Expand your Multiomic Capabilities with RNAscope™
- See More
-
APR 30, 2024Immuno-Oncology Virtual Event Series 2024
-
MAY 07, 20243rd International Biosecurity Virtual Symposium
-
MAY 23, 2024For the Love of Digital PCR 2024
- See More