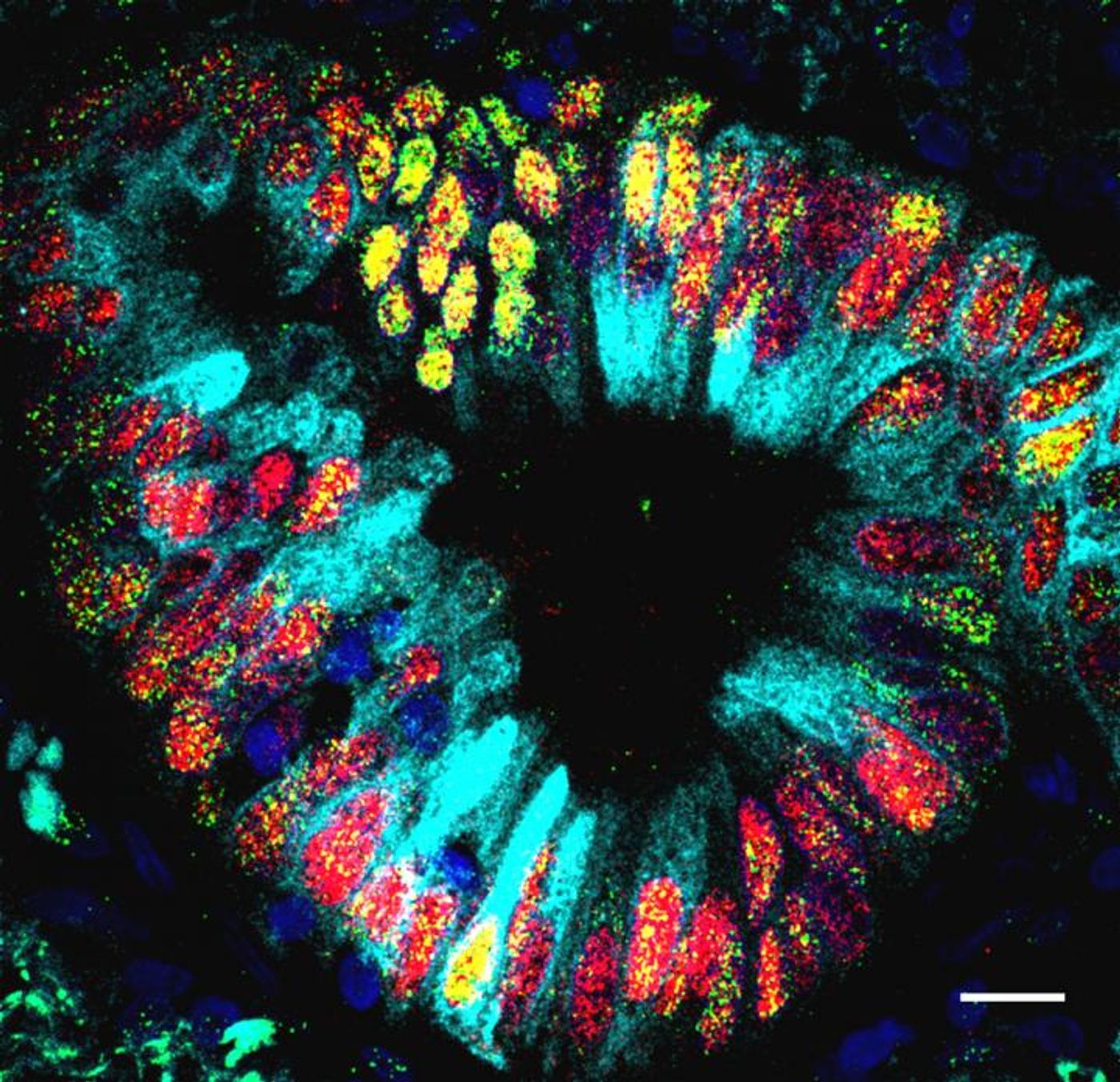
Cells Change Type After Losing One Gene
Tumors tend to consist of a chaotic mix of cells; one area of the tissue will express one set of genes and have different physical properties than other parts of the tumor. Researchers were still surprised to find a bunch of tiny digestive organ parts along with the cells of a lung tumor. Reporting in Developmental Cell, the researchers found that these cells had lost a regulatory gene that helps determine cell type. When the cells could not turn into lung cells, they went for the closest available type in the developmental line, cells of the gut.
Lead researcher of this work, Purushothama Rao Tata Ph.D., has spent years studying how cells regenerate after injury, and the developmental flexibility they can employ. He wondered if any of these processes applied to tumor cells. He turned his attention to non-small cell lung cancer, a leading cause of cancer deaths around the world.
The Cancer Genome Atlas Research Network contains genomic data from thousands of samples taken from 33 different kinds of cancer, which Tata utilized for his work. He determined that many tumors from non-small cell lung cancer did not express Nkx2.1, a gene that sends cells to their fate as part of the lung. The tumors were expressing genes that have been linked to esophageal and gastrointestinal organs instead.
"Cancer cells will do whatever it takes to survive," said Tata, an assistant professor of cell biology at Duke University School of Medicine and Duke Cancer Institute member. "Upon treatment with chemotherapy, lung cells shut down some of the key cell regulators and pick up the characteristics of other cells in order to gain resistance."
That led Tata to hypothesize that when lung tumor cells lose Nkx2.1, they cease to be lung cells and morph into other types. Lung and gut cells come from the same parent cell type, so it is not a surprising change, even though it seems strange.
The hypothesis was tested by Tata’s research team by using a mouse model. After deleting the Nkx2.1 gene from only lung cells, structures began to appear like some in the gut. These gastric-like tissues, incredibly, also made digestive enzymes as though they were part of the stomach.
Additional genetic manipulation was performed in the mouse model; the activation of cancer genes SOX2 or KRAS along with the lung cell deletion of Nkx2.1. In the SOX2 mice, tumors appeared that resembled the foregut, while in the KRAS mice, tumors looked like parts of the mid- and hindgut.
In additional work, a mini lung tumoroid system was developed. That enabled the researchers to confirm that genes are enough to change the fate of lung cells. Those cells don’t need signals from the local environment.
"Cancer biologists have long suspected that cancer cells could shapeshift in order to evade chemotherapy and acquire resistance, but they didn't know the mechanisms behind such plasticity," said Tata. "Now that we know what we are dealing with in these tumors - we can think ahead to the possible paths these cells might take and design therapies to block them."
Tata has plans to continue this work to investigate the mechanisms by which lung cancer cells develop drug resistance.
Sources: AAAS/Eurekalert! Via Duke University, Developmental Cell