Over one thousand DNA variations in the human genome are associated with both increased susceptibility to systemic lupus erythematosus (SLE) and the ability to alter gene expression that controls immune responses, UT Southwestern Medical Center scientists reported in an
eLife study published last week.
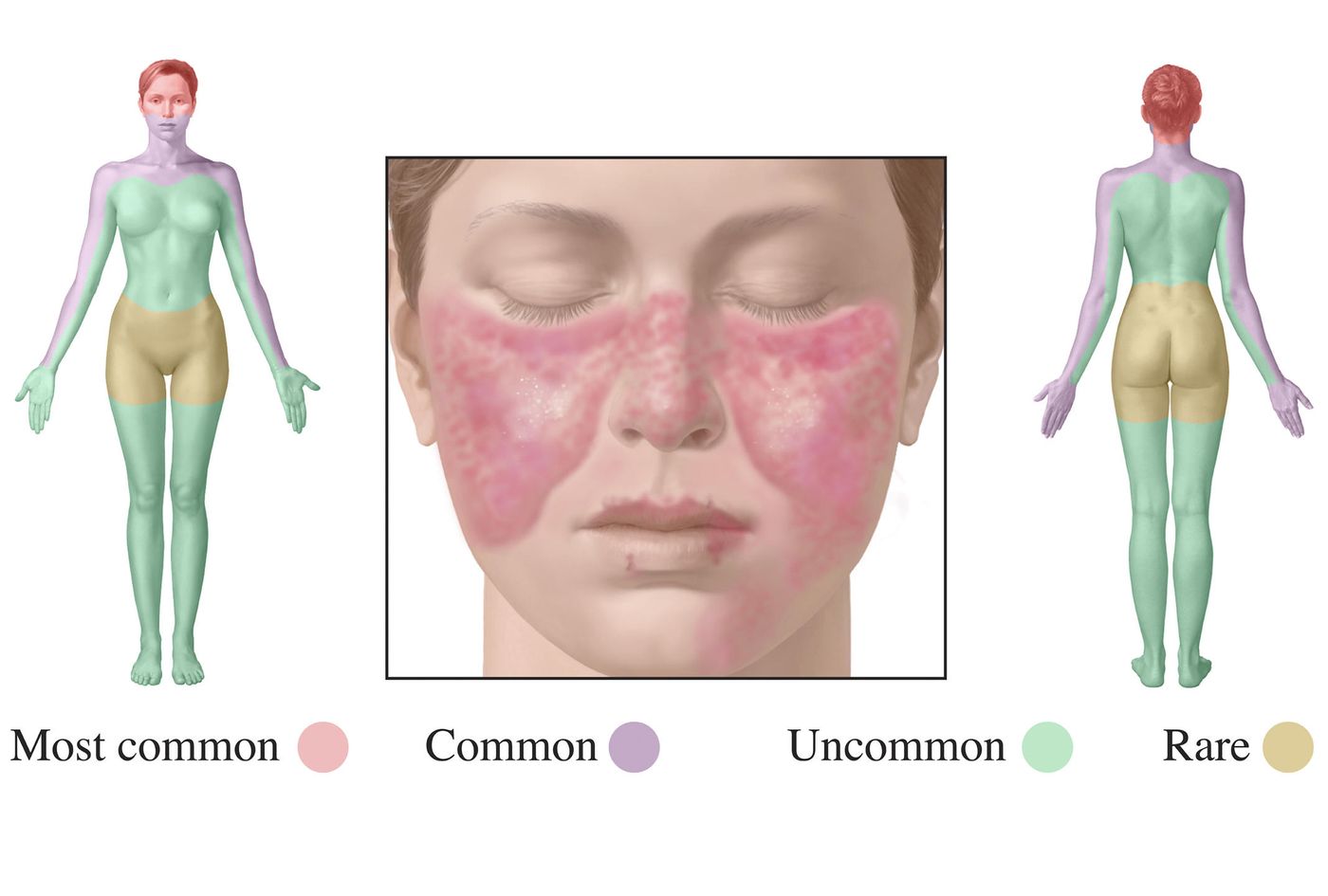
SLE, commonly known as lupus, is an autoimmune disease where the body’s immune system mistakenly attacks the organs, causing system-wide damage that can lead to death. Lupus affects 9 times as many women as men, and onset of the disease is most often between the ages of 15 and 44.
During a two-year study, researchers sequenced the DNA of 1349 American Europeans, 773 had lupus and 576 did not. These sequences provided the research team with genetic information leading them to lupus-associated genetic regions dispersed across the entire genome, with very specific DNA clusters linked to either increased lupus risk or increased protection from lupus.
After identifying both dangerous and protective genetic variants, they compared their data from American Europeans with data from public genome databases to discover where else, if anywhere, these DNA clusters are found. Results showed variations of the DNA clusters in various subpopulations across the globe: South America, South Asia, Africa, East Asia, and more. Scientists believe that this widespread diversity implies the ancient origin and persistence of lupus genes over time.
“This same type of genetic analysis will allow the clustering of [lupus] patients into specific groups, based on their genetic predispositions, which would improve clinical management and potentially allow the development of more targeted therapies," said Edward Wakeland, PhD, co-senior author of the study.

Depending on the specific genetic profile of people in high-risk groups, the use of personalized medicine could greatly reduce the amount of deaths that arise from lupus. Wakeland and his colleagues believe that a similar method of personalized health care could also be applied to other autoimmune diseases like type 1 diabetes, rheumatoid arthritis, and multiple sclerosis.
"Our findings support the potential of precision medicine to provide clinically relevant information about genetic susceptibility that may ultimately improve diagnosis and treatment,” Wakeland said.
Source:
UT Southwestern Medical Center