Cancer Cell 'Drones' Battle Immune System
Worldwide 8.8 million people die of cancer, that is almost 1 in 6 of all global deaths, and is the second leading cause of death globally. The most common cancers among men are lung, prostate, colorectal, stomach and liver while breast, colorectal, lung, cervix, and stomach cancer are most common among women. In all types of cancer, the body’s cells divide without stopping and spread to surrounding tissues. It can start almost anywhere in the human body and breaks up the orderly process of cell division and cell death. Cells become abnormal, old, and survive despite having damage, with new cells forming even if they are not needed. As cancerous cells continue to divide, they crowd out healthy cells and form growths called tumors, making it hard for the body to function correctly.
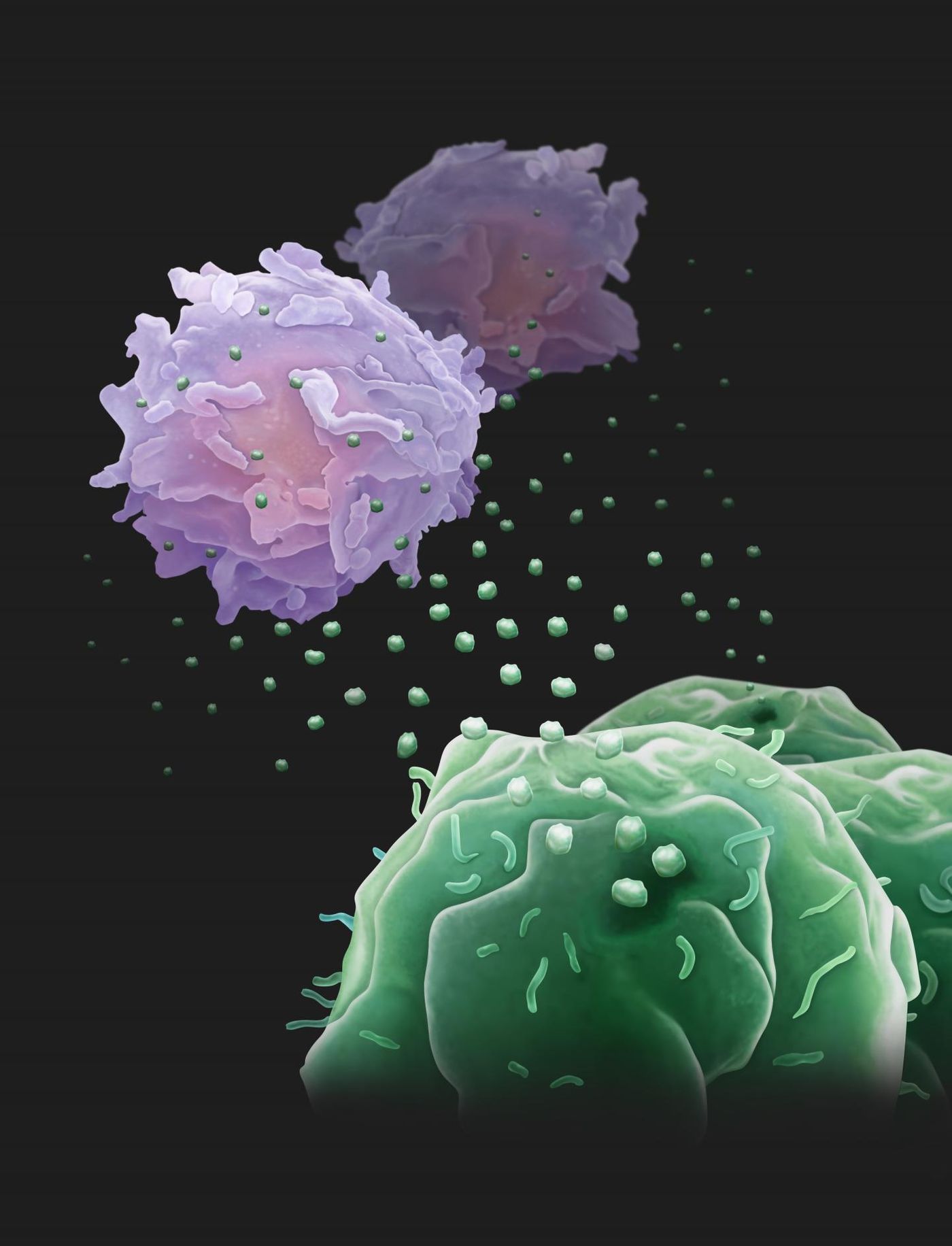
Cancer cells suppress the immune system to allow tumors and cancerous cells to thrive and spread unchecked in the body. One of the most significant innovations in cancer therapy is checkpoint inhibitor drugs. These drugs block attempts by a cancer cell to suppress the immune system; a primary target is a T cell surface protein known as PD-1. Previous studies have found the PD-L1 protein on tumor cells interacts with the T cell counterpart PD-1 and turns off the T cell anti-cancer response. A recent study, published in Nature, shows that cancer cells combat the immune system by releasing the biological version of drones carrying PD-L1 to assist in the fight.
The researchers from the University of Pennsylvania showed small vesicles, known as exosomes, circulate the blood armed with PD-L1 proteins that cause T cells to tire before they even reach the tumor to do battle. This discovery of PD-L1 on exosomes provides a new outlook on the immune checkpoint mechanism and offers novel insight into tumor immune evasion. While the study focused on metastatic melanoma, they did find PD-L1-carrying exosomes secreted by breast and lung cancer cells as well. Dr. Wei Guo, one of the collaborators on the work, said: "We propose a model in which these exosomes act like drones to fight against T cells in circulation, even before the T cells get near to the tumor."
These findings may allow for a less invasive measure of monitoring cancer/T cell battle through blood tests versus invasive biopsies of tumors. Measuring levels of PD-L1 before treatment may allow for prediction of tumor burden in a patient and utilize the information to predict treatment outcome. After initial treatment, researchers can use a blood test for PD-L1 levels to monitor how well drugs are keeping cancer cells in check. Much like we measure sugar levels in diabetes patients, it is possible that PD-L1 monitoring, along with other biomarkers on the circulating exosomes, could be utilized as a way to keep tabs on treatments and patient response in a similar manner. These findings are another step toward precision and personalized medicine in cancer treatment.
To learn more about cancer cells, how they spread, and treatment options watch the video below!
American Cancer Society, National Cancer Institute