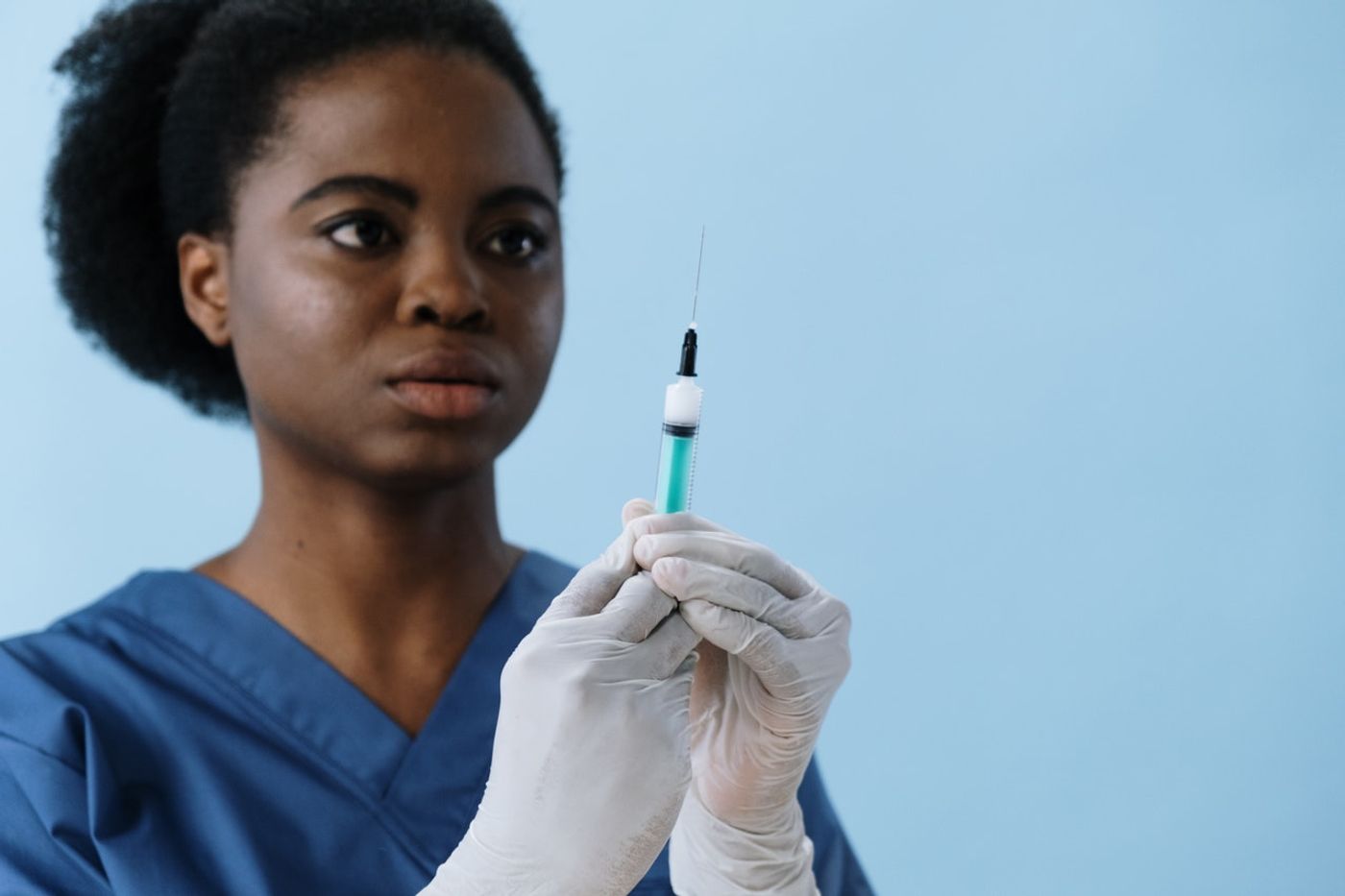
6 Injections a Year Prevent HIV Infections
Last year, around 1.7 million people became infected with HIV, with around half of these being women. Encouraging results emerging from a clinical trial of an investigational drug is providing hope to these women in the form of a reliable prophylactic therapy. The injectable drug, cabotegravir, was found to be more effective than the once-a-day preventative pill Truvada (Gilead), the current gold standard for pre-exposure prophylaxis.
A group of international collaborators came together as part of the H.I.V. Prevention Trials Network to conduct the randomized, double-blind clinical trial in a cohort of over 3,000 participants across seven African countries. Their goal was to compare the efficacy of Truvada with the new drug.
HIV affects the immune system by infecting white blood cells called CD4-positive T cells. The virus is incapable of reproducing on its own. Therefore, it relies entirely on the infected T cell to do the heavy lifting. The virus attaches to the immune cell, fusing its envelope with the cell membrane before hijacking the nucleus of the cell, forcing it to make copies of itself using the cellular machinery. More viruses are subsequently released into the blood, multiplying and weakening the body’s natural defenses over time.
The results of the trial were groundbreaking: the injection was 89 percent more effective than Truvada, compelling researchers to end the trial early. Cabotegravir is an integrase inhibitor, a type of antiretroviral that blocks the viral enzyme integrase from inserting the HIV genome into the host cell’s DNA. Besides its improved efficacy, the treatment has clear advantages over existing HIV prophylactics: individuals only need to get a shot once every couple of months and the drug does not require refrigeration, allowing mobile clinics to administer it to women together with injectable birth controls.
One drawback is that there is a higher risk of viral resistance in the event that the injection schedule is disrupted. “If you go too long, and you get exposed to H.I.V., you could get a drug-resistant virus, so every eight weeks is going to be mandatory,” said Dr. Monica Gandhi, an H.I.V. expert at the University of California, San Francisco. “And because of that, to keep adherence to that type of schedule, we have to be creative.”
Sources: New York Times, World Health Organization.