Antibodies Gain the Upper Hand Against Sly Tumors
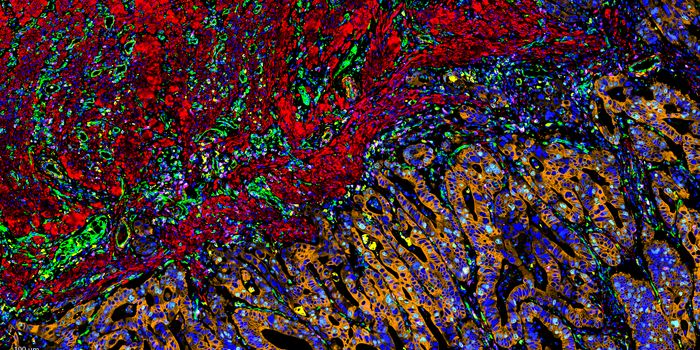
Tumors use ingenious approaches to stay just out of reach of immune cells on patrol and avoid detection. For instance, cancer cells at the periphery of the tumor have been shown to secrete a cocktail of chemicals that creates an impenetrable barrier to immune cells. By suppressing the immune system, these tumor factors interfere with antigen-presenting cells such as macrophages and block the production of tumor-specific T lymphocytes. Beyond the reach of the immune patrol, tumor cells continue to multiply uncontrollably.
Scientists have developed several therapeutic countermeasures to overcome this tumor-induced immune suppression—treatments that, at least in theory, bear tremendous potential. Unfortunately, when it comes to real-world clinical outcomes, many of these immunotherapies have missed the mark. For instance, some studies show that more than half of patients fail to respond to checkpoint blockade therapy as a means of overriding tumors’ immune suppression.
Now, cancer immunologists from the University of Southampton have added a promising new immunotherapy that’s destined to boost oncologists’ tumor-fighting arsenal: an antibody that targets an immune molecule called OX40. The results were published in the Journal for Immunotherapy of Cancer.
OX40 is predominantly expressed in a subset of T cells called Treg cells—specialized immune cells that regulate immune activity. Tregs have been observed to be prevalent around the outer border of tumor tissues, suppressing immune activity in this tumor microenvironment. The new antibody therapy binds specifically to OX40, inactivating Tregs and allowing other immune effectors to enter the scene and begin tumor destruction.
Antibody and vaccine experts Mark Cragg and Jane Willoughby, who led the study, also found that by swapping the antibody isotype, or the region which determines the antibody’s effector function, their new therapy was a potent activator of killer T cells. This triggered a powerful and sustained immune response against the malignant tissues.
"Clinical trials with anti-OX40 antibodies have shown that the body can tolerate these drugs but unfortunately have also shown disappointing clinical responses,” said Cragg. “We need to understand why this is.”
This study provides a means of overcoming these long-standing clinical challenges. "This new data shows us that when there is a cancer with lots of Tregs we could use the equivalent of the m2IgGa isotype and in patients where we feel we need better cytotoxic T cells we could use the equivalent of a mIgG1 isotype to boost the immune response.
“This information is important for developing the next generation of OX40 antibodies that we hope will be more effective in treating patients with cancer," Cragg added.
While this OX40 antibody therapy continues down the path towards the clinic, a combination of immunotherapeutic agents will likely provide better outcomes for cancer patients. For example, some preclinical studies have shown that a combo of anti-OX40 together with anti-CTLA-4 antibodies boosted the numbers of activated CD4+ and CD8+ T cells in the tumor microenvironment. This provided better outcomes compared to administering anti-OX40 as a monotherapy.
Sources: Journal for Immunotherapy of Cancer, Cancer Immunol Res, EurekAlert.