Acute lymphoblastic leukemia (ALL) and non-Hodgkin’s Lymphoma (NHL) affect 75,000 and 72,000 people each year in the United States, respectively. In addition to immunotherapy, chemotherapy, radiation, and stem cell transplants are a few treatments used to fight these cancers, but thousands of Americans still die every year.
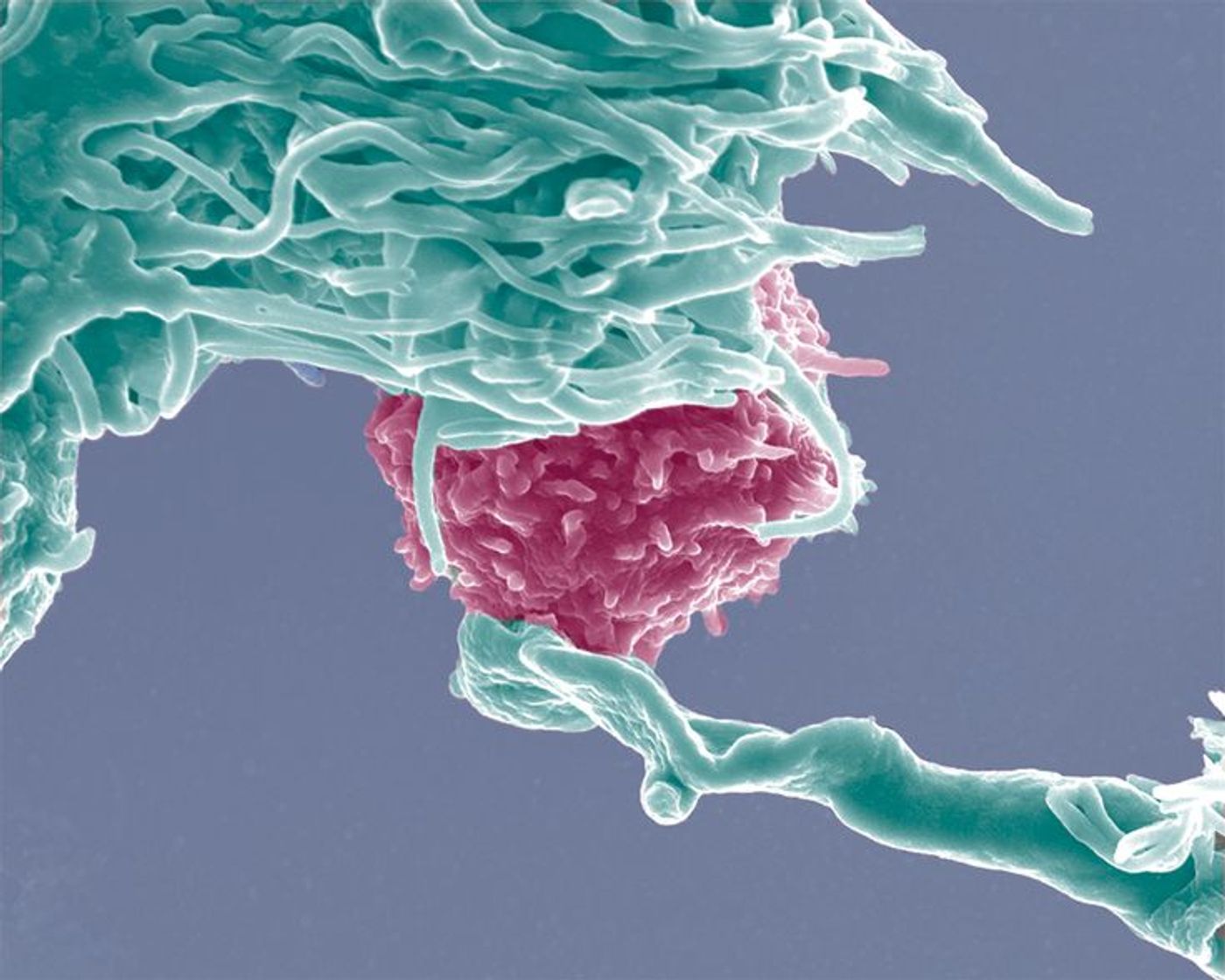
A new study from the Children’s Hospital of Philadelphia (CHOP) provides promising new findings to improve current chemotherapies for pediatric cancer. Together with the Perelman School of Medicine at the University of Pennsylvania, CHOP researchers identified a specific sub-type of T lymphocytes to use for immunotherapy: the youngest cells.
Young T lymphocytes, characterized either as naïve cells or stem central memory cells, both expanded successfully in the lab and proved to be most efficient in attacking cancerous cells. The study was published last month in
Science Translational Medicine.
The team of researchers observed 50 patients; all were either children or teenagers with B cell cancers. 38 of the 50 had ALL and 12 had NHL. By monitoring their T lymphocyte count every month for six months, the researchers were able to see positive change in the new immunotherapy using young T lymphocytes.
The therapy works by first taking out the patient’s T lymphocytes, tuning them to specifically find and kill cancerous B cells, and then returning them to the patient so they can work.
In the words of one of the study leaders, David M. Barrett, MD, PhD, "Collecting and expanding these cells could increase the number of children with cancer who could benefit from this innovative treatment."
Despite the clear success in the younger cells’ ability to kill cancer cells, they were also uniquely susceptible to chemotherapy, much more so than older T lymphocytes. In order to avoid elimination by chemicals from chemotherapy, which is almost always used in conjunction with immunotherapy at some point during cancer treatment, the researchers agreed that the young T lymphocytes would have to be extracted before any chemotherapy is administered.
"We could keep the patient's early-lineage T cells in reserve, in case the patient needs them later,” Barrett said.
Although the immunotherapy with young T lymphocytes showed increased success in treating both ALL and NHL patients, ALL patients saw greater success because they had more young T lymphocytes to collect from than NHL patients. Thus, the fight against B cell cancers is far from over.
Source:
Children’s Hospital of Philadelphia