The 1990s were an exciting time for cancer research, as scientists genetically engineered the very first chimeric antigen receptor (CAR) T cells. These specialized lymphocytes were intricately designed to recognize and target cancer cells as efficiently as possible. However, the technology wasn’t perfect. Sometimes the CAR T cells responded too strongly, targeting more than just cancer cells and killing more than just tumors. Researchers soon realized that they had to incorporate a regulatory process to keep CAR T cells from doing more harm than good, and now a group from Purdue University seems to have the answer.
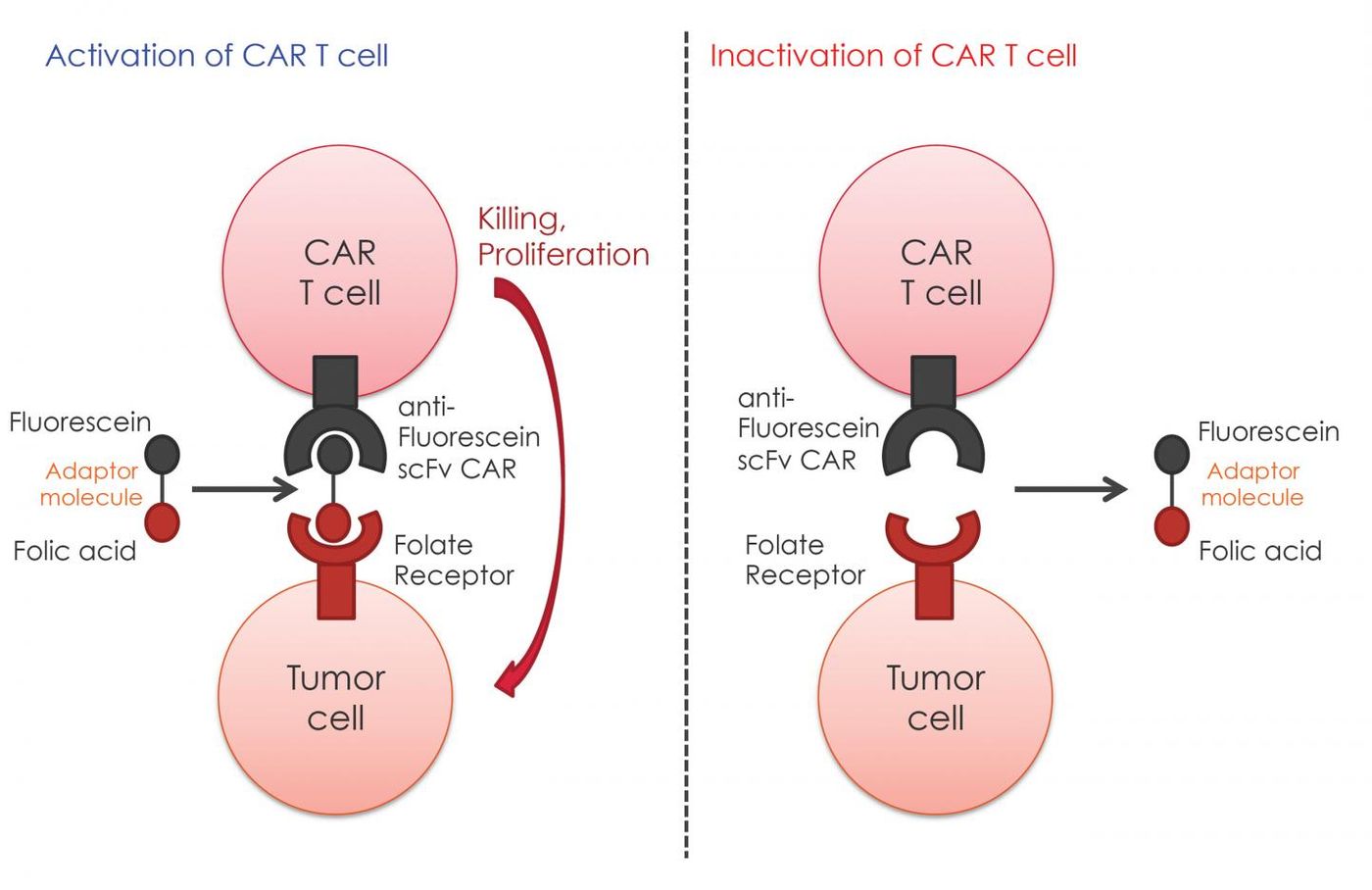
To prevent CAR T cells from “going rogue,” Purdue scientists developed and implemented a system of required activation to have more control over the cells’ cytolytic activity. CAR T cells had a slight tendency to kill the tumor cell so quickly that the host cells responded as if there was a toxin sensed in the body. Then, with the tumor cell population depleted, CAR T cells looked for other, healthy cells with which to hone in their cytolytic capabilities.
The technology developed at Purdue requires activation of CAR T cells by a small molecule adapter before they can kill any cell types. In addition to gaining control of the CAR T cells activity, the researchers also created the cells to be eliminated from the body more quickly than the initial version of CAR T cells, which were known to remain in the body indefinitely.
Researchers tested their new system in animal models, and so far the intended design is confirmed to be an effective way to harness the power of CAR T cells without letting them run rampant.
"By controlling the level of adaptors in the system, we can control the numbers and potencies of active CAR T cells,” said graduate student Yong Gu Lee. “Those that aren't stimulated by an adaptor molecule are blind and do not recognize or target any cells. Eventually, if they remain inactive for a while, they should die and be eliminated from the body."
With the right signal from a specific adaptor molecule, the newly engineered CAR T cells are activated with an anti-tumor mission that is also specific to a cancer subtype. The researchers recognize that most known cases of cancer show mixed populations of tumor cells expressing a plethora of characteristics, and in response they designed the CAR T cells to be responsive to a variety of adapters which signal for specific anti-tumor activity.
“It is far easier to manipulate and swap [adaptor molecules] in and out of it than the T cells,” said Phillip S. Low, director of the Purdue Center for Drug Discovery and leader of the study.
During their animal studies, the Purdue researchers confirmed that anti-tumor activity only occurred when both CAR T cells and adaptor molecules were present. The adaptors are made with a yellow dye called fluorescein isothiocyanate on one end of the molecule, where CAR T cells bind. On the other end of the molecule is a cancer-targeting molecule. Once a CAR T cell binds, activates, and successfully kills the tumor cell types as instructed by the adaptor molecule to which it is bound, the CAR T cell is then free to bind to a new adaptor.
Source:
Purdue University