Rodents with Joint Disease Reveal Cartilage-Sustaining Biochemical
A biochemical compound called adenosine is both the cause of osteoarthritis and the subject of promising research for a new joint treatment to prevent millions of joint replacement procedures completed annually as a result of osteoarthritis pain.
Adenosine is made up of equal parts adenine, a nucleotide, and a ribose sugar molecule. The compound is also derived from adenosine triphosphate (ATP), a molecule incorporated by the body to hold on to energy until it’s needed for use by cells. Adenosine’s role in osteoarthritis development comes from its regulation of chondrocyte populations, the specialized cells responsible for both the production and maintenance of a part of cartilage tissue in joints called extracellular matrix, which makes cartilage the stable and flexible tissue that it is.
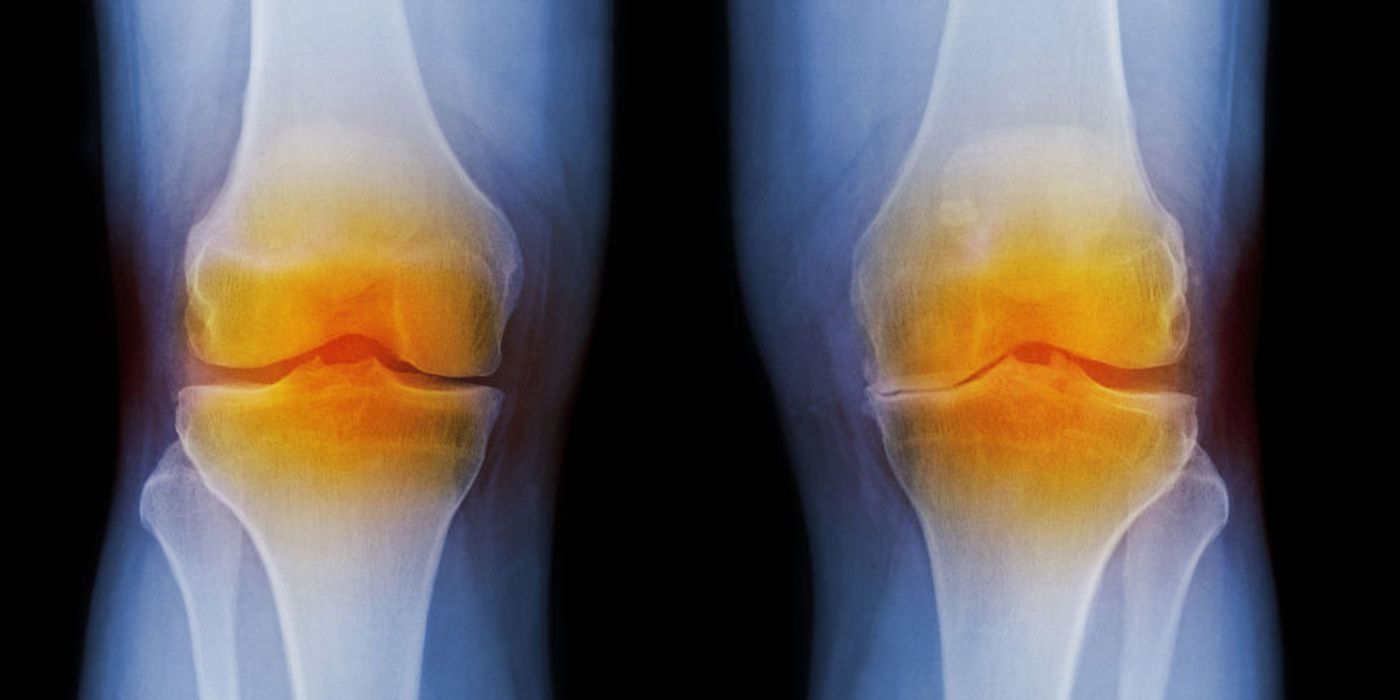
Osteoarthritis, also known as degenerative joint disease, is the most common chronic condition of the joints, causing pain, stiffness, and swelling as a result of the breakdown of cartilage between the joints. Past research indicated that together, inflammation and aging contribute to a reduction in ATP production in chondrocytes. The newest study, from the NYU Langone Medical Center, now links this phenomenon to osteoarthritis.
"We found that if adenosine levels decrease, or if the capacity to respond to adenosine diminishes, cartilage starts to degenerate," explained senior study investigator Bruce Cronstein, MD. "Our study suggests that diminished ATP and adenosine production are likely contributing factors to the development of osteoarthritis in aging individuals.”
Essentially, Cronstein’s study was based off the observation that lower levels of adenosine causing a decrease in the number of cells producing cartilage and lower levels of chondrocyte surface proteins that facilitate adenosine signaling (surface proteins with A2A adenosine receptors bind adenosine; this bondage sustains the cell) contribute to osteoarthritis development.
Cornstein and his team tested their theories in several trials with osteoarthritis-prone rats and mice. First, high levels of adenosine prevented osteoarthritis-prone rats from actually developing any joint problems. If the same holds true in human joints, adenosine replacement therapy could delay or even prevent osteoarthritis altogether.
Next, when treated with IL-1beta, a molecular osteoarthritis promoter, mouse chondrocytes produced significantly less ATP. Additionally, mice with no A2A adenosine receptors had trouble moving, compared to control mice with functioning adenosine receptors. Further tests confirmed that their movement problems were a direct result of osteoarthritis.
Lastly, and most important for future clinical applications, treatment with adenosine for osteoarthritis-prone mice prevented the disease from developing. Further tests, including with human subjects, could confirm these findings and contribute further to the future of adenosine replacement therapy as an alternative to joint replacement procedures for osteoarthritis.
The present study was published in the journal Nature Communications.
Sources: Arthritis Foundation, Bioessays, News Medical Life Sciences, New York University School of Medicine