Germs are Gaining Resistance to Hand Sanitizers
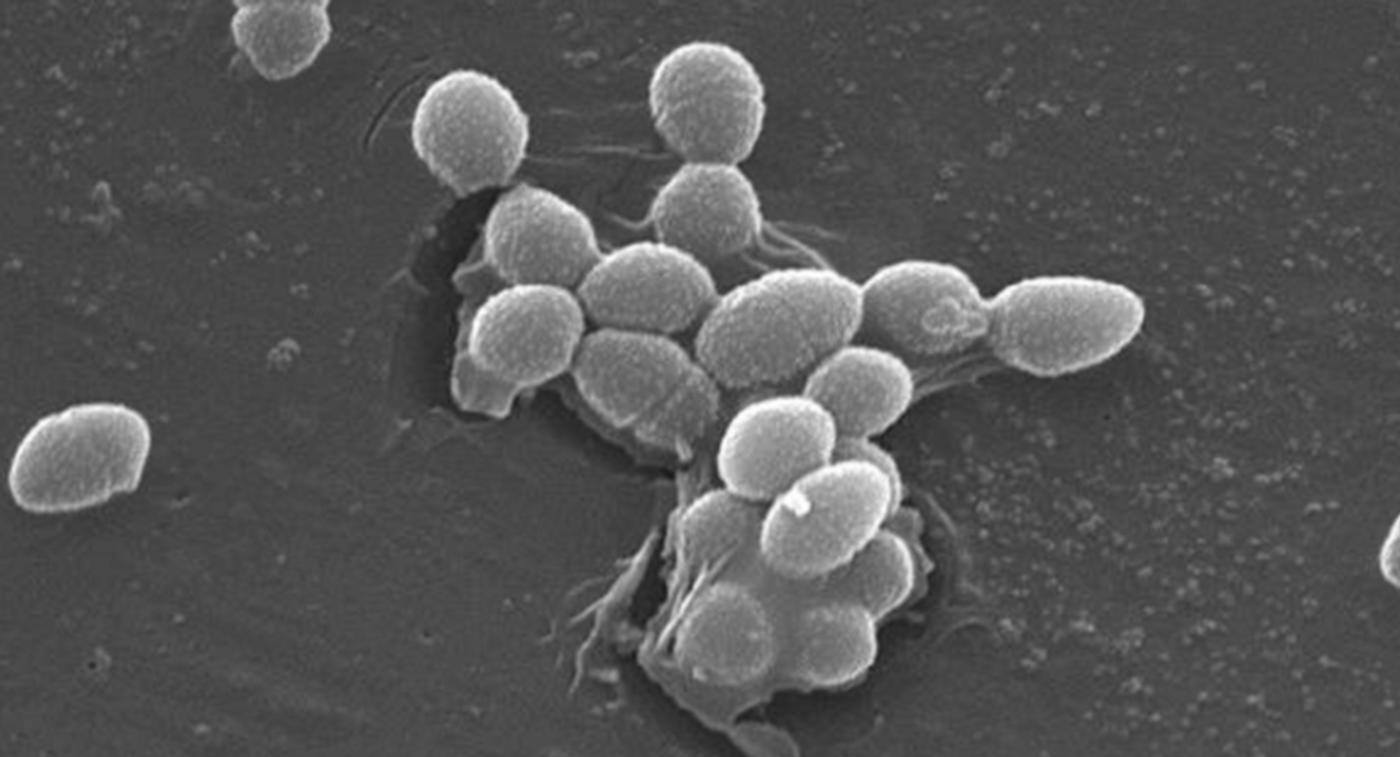
Since people learned to fight off bacteria, our health has improved dramatically. But bacteria have been getting better at finding ways to avoid our protective measures. Antibiotic-resistant microbes are expected to pose a significant threat to public health in the coming decades. It seems that germs are also getting the upper hand on hand sanitizers. New research by scientists at the Peter Doherty Institute for Infection and Immunity and Austin Health has shown that certain strains of a microbe called Enterococcus faecium, which causes many infections in hospitalized patients, has become ten times more resistant to alcohol-based hand sanitizers compared to older strains.
This work, reported in Science Translational Medicine, suggested that hand sanitizers may have helped contribute to the rise in resistance. Many hospitals instituted a regimen of hand-washing followed by sanitizer to combat MRSA, a deadly S. aureus pathogen. Professor Tim Stinear of the Doherty Institute, who led this work, noted that the program was successful - at controlling staph.
“That’s been highly effective at getting rid of golden staph. Rates of golden staph infection have been decreasing for the last 15 years,” said Stinear.
Co-lead author Professor Paul Johnson, Director of Research at Austin Health noticed that E. faecium infection rates were rising. When he told others he thought the sanitizers might be related to the problem, there was a lot of skepticism. “It’s a broad-spectrum disinfectant – it gets into the bacterial membranes and blows them apart. It’s a general annihilator of cells,” said Stinear.
E. faecium normally lives in the gut and isn’t usually a health problem. They are becoming more problematic, however, and causing more tenacious infections. Enterococci bacteria that develop resistance to vancomycin, considered an antibiotic of last resort, are particularly problematic; they are called vancomycin-resistant enterococci (VRE).
Patients that take antibiotics or get therapeutics like chemo are especially vulnerable to VRE infection. “When your natural gut bacteria are disturbed you can become prone to VRE, in the context of a health-care institution,” Stinear explained.
After exposing 139 E. faecium strains to an alcohol solution, the team found “the new isolates were more tolerant to alcohol exposure than the older isolates,” said Stinear.
“Alcohol use in hospitals has gone from hundreds of liters a month to thousands of liters a month of these alcohol-based disinfectants. Anywhere we repeat a procedure over and over and over again, whether it’s in a hospital or at home or anywhere else, you’re giving bacteria an opportunity to adapt, because that’s what they do, they mutate. The ones that survive the new environment better then go on to thrive.” That risk also goes up when guidelines are ignored.
The researchers uncovered evidence of resistance to alcohol resistance in the bacterial genomes. “We looked for signatures in the genome of the bacteria of adaptation, and we found them,” said Professor Stinear. “We could see that there were genes that looked to be under evolutionary selection and those genes, when we mutated them, changed the alcohol tolerance of the bacteria.”
For now, its still business as usual in the hospital hand-washing department. “This isn’t the end of hospital hand hygiene, that’s been one of the most effective infection control procedures that we’ve introduced worldwide,” said Stinear. “The WHO recommends it. But we can’t rely solely on alcohol-based disinfectants, and for some bacteria, like VRE, we’re going to need additional procedures and policies in place. For hospital[s] this will be super-cleaning regimens, which include alternative disinfectants, maybe chlorine-based. An extra level of infection control that doesn’t just rely on alcohol-based disinfectants is required.”
Sources: Pursuit at University of Melbourne, Science Translational Medicine