Finding a New Way to Combat Viruses
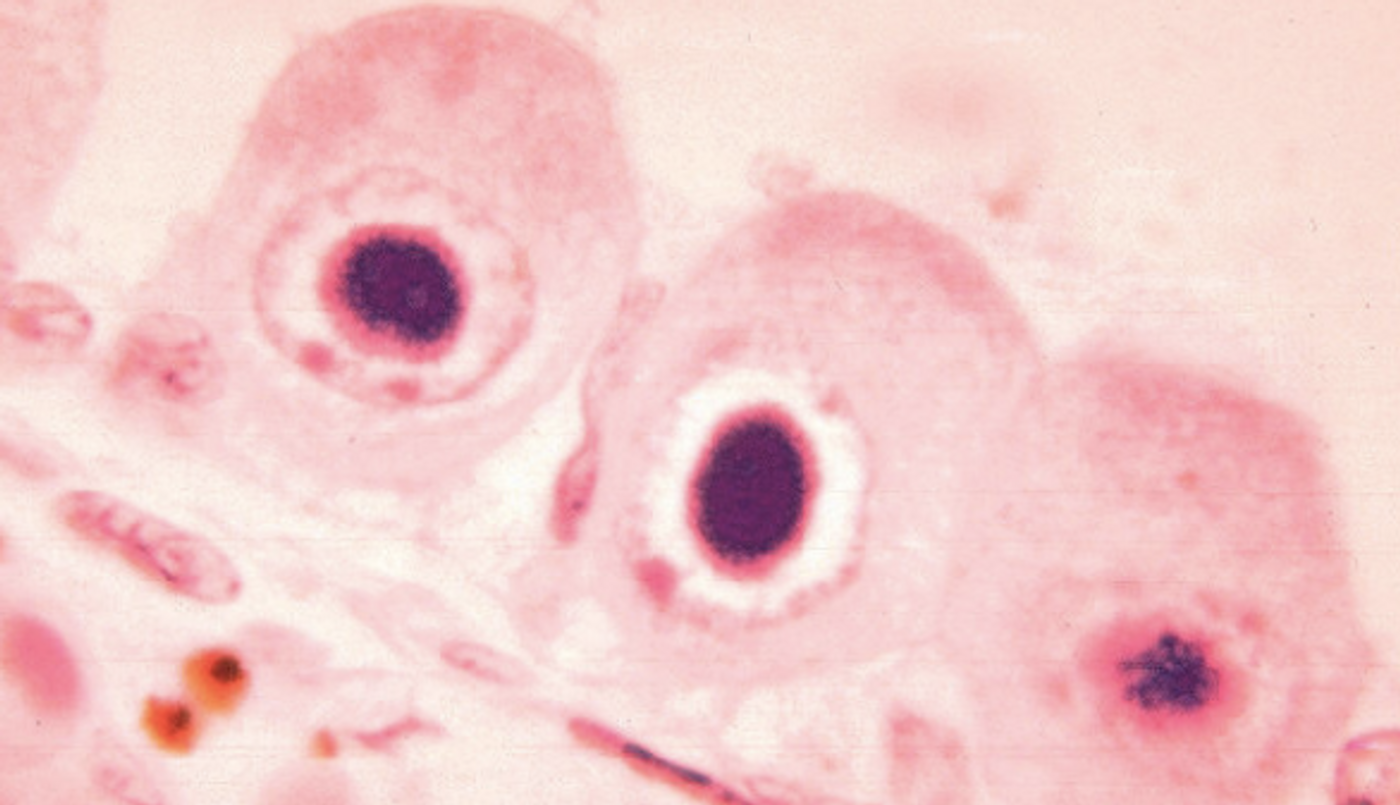
A leading cause of birth defects and a common complication of transplants is the human cytomegalovirus. The virus has evolved to get around the natural defenses of the immune system, and the mechanism the virus uses to do so was a mystery. Researchers led by Leor S. Weinberger, Ph.D., the William and Ute Bowes Distinguished Professor and director of the Gladstone-UCSF Center for Cell Circuitry have now identified the mechanism that cytomegalovirus uses to replicate, which can be used as a drug target for both cytomegalovirus and other viruses.
"The way the virus operates is pretty cool, but it also presents a problem we couldn't solve," said Noam Vardi, Ph.D., postdoctoral scholar in Weinberger's laboratory and first author of the new study, which was reported in the Proceedings of the National Academy of Sciences.
Typically, a virus invades a host cell and the call acts to put brakes on the viral DNA so it can’t get further. To evade that system, cytomegalovirus uses a protein called PP71 to accompany viral DNA that gets injected into a host cell. After getting inside, the PP71 proteins are released and the viral DNA can get to reproducing and then spreading the infection.
"The PP71 proteins are needed for the virus to replicate. But they actually die after a few hours, while it takes days to create new virus,” noted Vardi. “So how can the virus successfully multiply even after these proteins are gone?"
It turns out that PP71 has another job when it gets into the cell; it activates another protein, called IE1. That protein takes over when PP71 dies off, and new viral particles are continually generated.
The team wanted to verify their findings, so they made a synthetic virus which enabled the researchers to manipulate the level of IE1 proteins. They were then able to control how quickly IE1 was broken down.
"We noticed that when the IE1 protein degrades slowly, as it normally does, the virus can replicate very efficiently," revealed Vardi. "But if the protein breaks down faster, the virus can't multiply as well. So, we confirmed that the virus needs the IE1 protein to successfully replicate."
It’s known that cells have to specialize to perform their intended function. They start out as a kind of blank slate, a stem cell; then it goes down a path to become a specific cell type. But scientists did not know why cells remained specialized even after the proteins that sent them down that path had disappeared. This work may help us learn more about that.
"The issue is similar for the virus," explained Weinberger, a professor of pharmaceutical chemistry at UC San Francisco. "It was not clear what mechanisms allowed the virus to continue replicating long after the initial signal from the PP71 had decayed to a whisper. Our findings uncover a circuit encoded by the virus that controls its fate and indicate that such circuits may be quite common in viruses."
This study may also aid in the development of therapeutics for other viruses, such as Epstein-Barr and herpes simplex virus 1 and 2.
The talk above features Weinberger discussing novel approaches to targeting viruses.
Sources: AAAS/Eurekalert! Via Gladstone Institute, PNAS