Researchers Learn How Hantavirus Infects Cells
First identified in 1993, hantavirus infections can cause dangerous and potentially deadly respiratory illnesses. Researchers have now learned how the virus gains entry into cells and found a way to stop it. Reporting in Nature, scientists at Albert Einstein College of Medicine discovered that the virus can use a receptor on the surface of cells called protocadherin-1 (PCDH1) to get inside. When they removed the receptor in a mouse model, the mice became almost totally resistant to infection, indicating that the receptor may be a useful therapeutic target in the treatment of hantavirus pulmonary syndrome (HPS).
This work could become extremely important. While only 728 cases have been reported in the United States so far, that number is likely to rise. "While hantavirus infections are rare, they're expected to increase in the coming decades as temperatures across the globe rise due to climate change. And we're totally unprepared for this possibility," explained one of the study leaders, Kartik Chandran, Ph.D., a professor of microbiology & immunology and Harold and Muriel Block Faculty Scholar in Virology at Einstein.
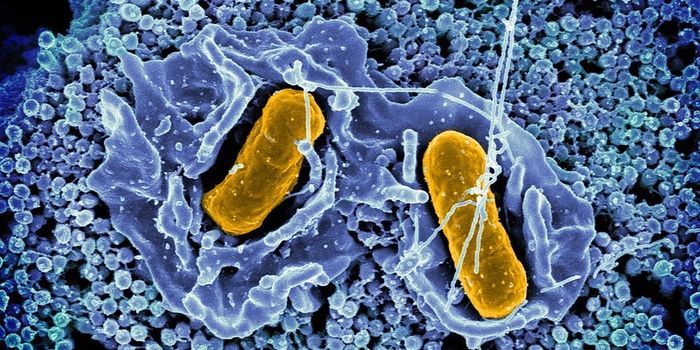
The virus is transmitted from the saliva, urine or feces of infected rodents, to humans who inhale it. Symptoms of HPS can include muscle aches, fatigue, and fever. After about a week, coughing and breathing difficulties set in. According to the Centers for Disease Control and Prevention, HPS kills about 40 percent of infected individuals, and there are no vaccines or treatments currently available. This work may help change that.
“Our work not only provides the final proof that PCDH1 is a cellular receptor for hantavirus to establish infection and cause diseases but also establishes a much-needed animal model for developing anti-hantavirus therapeutics by using PCDH1 as the drug target,” said study co-leader Zhongde Wang, Ph.D., a professor in Utah State University’s Department of Animal, Dairy and Veterinary Sciences.
"Our findings provide new insights into how these infections develop and how they might be prevented or treated," added Chandran.
The researchers used a genetic screen to see if they could block infection by hantavirus by knocking out any genes from cells. The screen identified PCDH1, which has been shown in previous work to have a role in human lung function and disease.
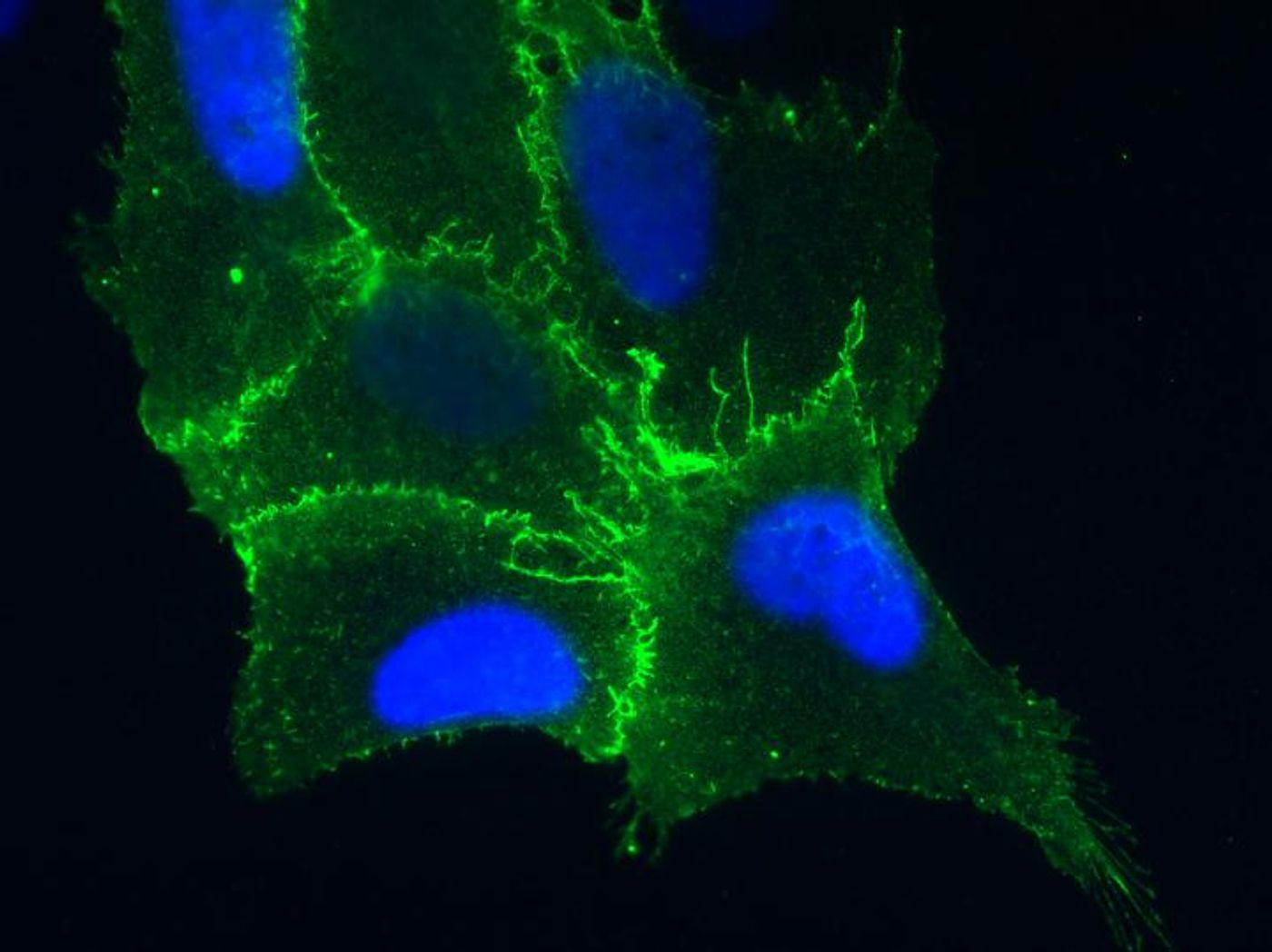
Next, the scientists removed the gene from cells that line human lungs - pulmonary endothelial cells. The cells resisted infection by hantavirus strains found in North and South America, the Sin Nombre virus and Andes virus infections.
In the rodent model of hantavirus, Syrian golden hamsters, animals that lacked the PCDH1 gene resisted infection and injury that are caused by the Andes virus, while animals with the receptor fell victim to the infection.
"Our findings establish a key role for PCDH1 in lung infections caused by hantaviruses in an animal model that captures key features of HPS," said study co-leader John M. Dye Ph.D., chief of viral immunology at USAMRIID.
Their work also revealed the region of the PCDH1 protein that hantaviruses recognize. That primed a target for drug development. The research team created monoclonal antibodies that have a high affinity for that part of PCDH1. When exposed to cells, the antibody protected them from infection from both the Andes and Sin Nombre viruses. Ongoing work will test these antibodies in animal models.
Notably, there’s another group of hantaviruses in Europe, Asia, and sometimes the US that cause severe kidney disease, but don’t need the PCDH1 receptor to infect cells. "These viruses have other ways of invading cells that remain to be discovered," noted the co-first author of the report, Rohit Jangra, Ph.D., research assistant professor at Einstein.
Sources: AAAS/Eurekalert! Via Albert Einstein College of Medicine, USU, CDC, Nature