Fecal Transplants Recommended for Recurrent C. diff Infections
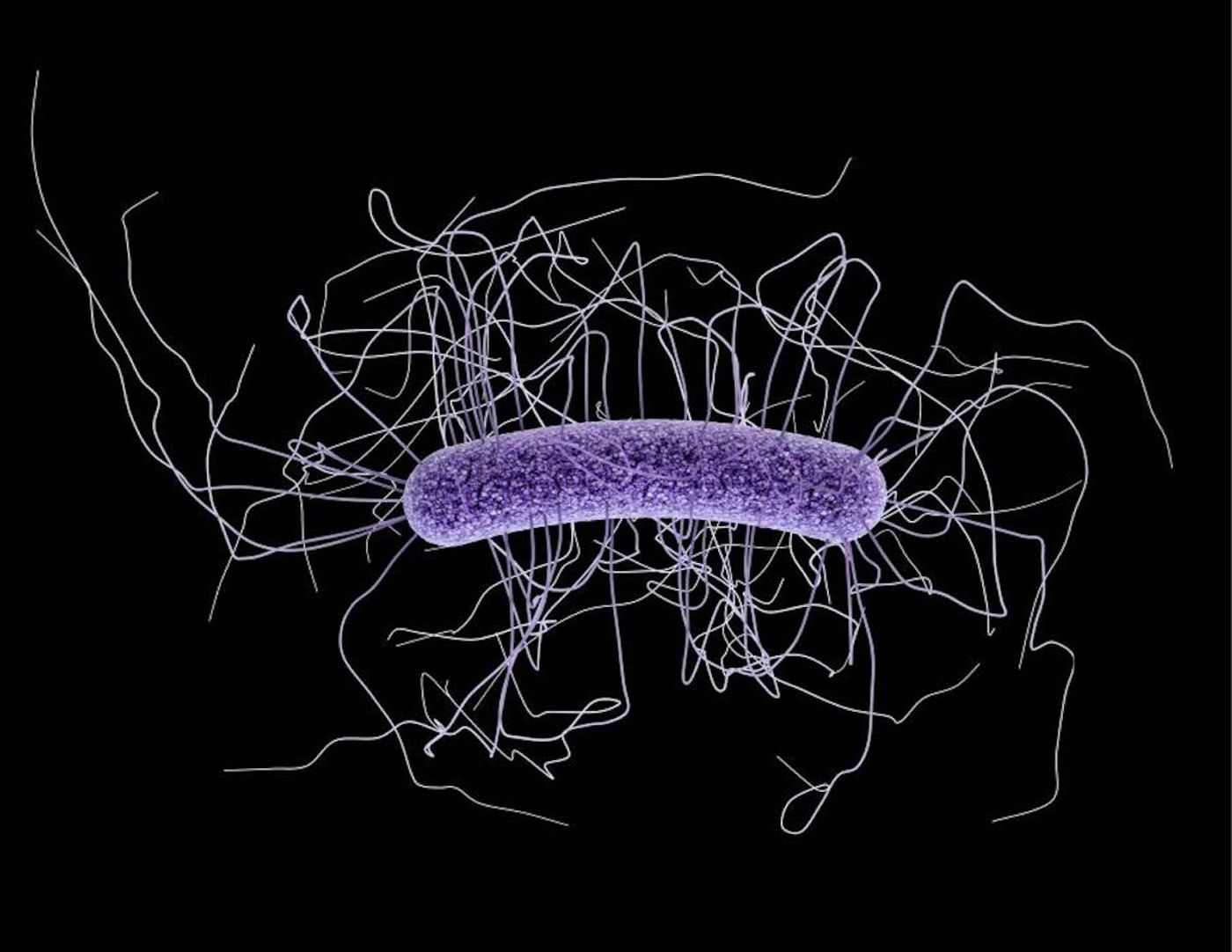
While hospitals are intended to be places of healing, people can acquire nasty infections with drug-resistant bacteria during a stay there. The bacterium Clostridioides difficile (C. diff) is relatively common in public spaces, and most healthy people won’t get an infection from it. However, it’s the most common cause of infections acquired in US hospitals. People with weak immune systems, such as the elderly or people receiving chemotherapy, are most at risk. According to the Centers for Disease Control and Prevention (CDC), C. diff sickens around 500,000 people every year. For almost one-third of them, it becomes a recurrent problem that can cause sepsis and death if it goes untreated.
"Twenty five years ago C. diff infections were easier to manage and often resolved with discontinuation of the initiating antibiotic," said Robert Orenstein, DO, an infectious disease specialist at Mayo Clinic. "However, these infections have become increasingly common and pernicious."
Orenstein is lead author on a new report in the Journal of the American Osteopathic Association, which recommends that transplantation of fecal microbiota from a healthy donor may be the best way to treat C. diff infections that antibiotics can’t tackle.
Our bodies host a vast community of microorganisms, and the microbes in the gut have been shown to have a powerful influence on our health. Imbalances in that microbiome can have serious implications for our immune system. According to the CDC, a study showed that nearly 50 percent of antibiotics that hospitals prescribed were either incorrect or unnecessary. Those broad-spectrum antibiotics can ruin the healthy microbiome, leaving the gut susceptible to opportunistic C. diff infections. The CDC noted that "a 30 percent decrease in the use of antibiotics linked to C. difficile infections in hospitals could reduce the deadly infections by more than 25 percent in hospitalized and recently discharged patients."
Although the oral drug vancomycin is approved by the FDA as a standard treatment for C. diff infections, the antibiotic can also destroy the beneficial microbes that live in the gut. There are new therapeutics that selectively target C. diff, however, they are often prohibitively expensive, noted Orenstein.
"Think of your gut as a forest and C. diff as a weed. In a thriving forest, weeds barely get a foothold. But if you burn the forest down, the weeds are going to flourish," explained Orenstein. Learn more about research performed at the Mayo Clinic on fecal transplants and C. diff infections from the video.
Instead of using an antibiotic to kill bacteria, fecal transplants work by adding a varied mixture of healthy microbes to an infected gut. These new microbes can help stop the spores of C. diff from growing and causing disease by releasing toxins. Fecal transplants can be easily ingested in a capsule, inserted in an enema, or directly instilled, to regenerate a diverse gut microbiome and improve health.
Although fecal transplants have been shown to work for patients with recurrent C. diff infections, they are still considered an experimental therapy. Several companies, noted Orenstein, have products currently in Phase 3 clinical trials, and they may be available as soon as 2020. He stressed that clinicians with patients experiencing recurrent C. diff infections should direct those patients to such trials. The FDA currently recommends that people receive a fecal transplant only after the third time they get a C. diff infection.
While fecal transplants are a good option, Orenstein added that clinicians must be more proactive about preventing infection and reducing the overuse of antibiotics.
"One of the most effective things physicians can do is become more responsible with antibiotic prescriptions," said Orenstein. "That means only prescribing when they are clearly indicated, not for colds or viral sinus infections. We also must be especially judicious with elderly patients."
Sources: AAAS/Eurekalert! via American Osteopathic Association, CDC, Journal of the American Osteopathic Association