A Neuropsychiatric Crisis Might Follow COVID-19
Infectious diseases can leave people near the brink of death, and that often comes with neuropsychiatric symptoms. A 2017 publication noted that any physician working in critical care knows that a systemic infection is often accompanied and complicated by delirium. Studies have suggested that viruses, including HIV and influenza can cause a wide variety of psychiatric disorders.
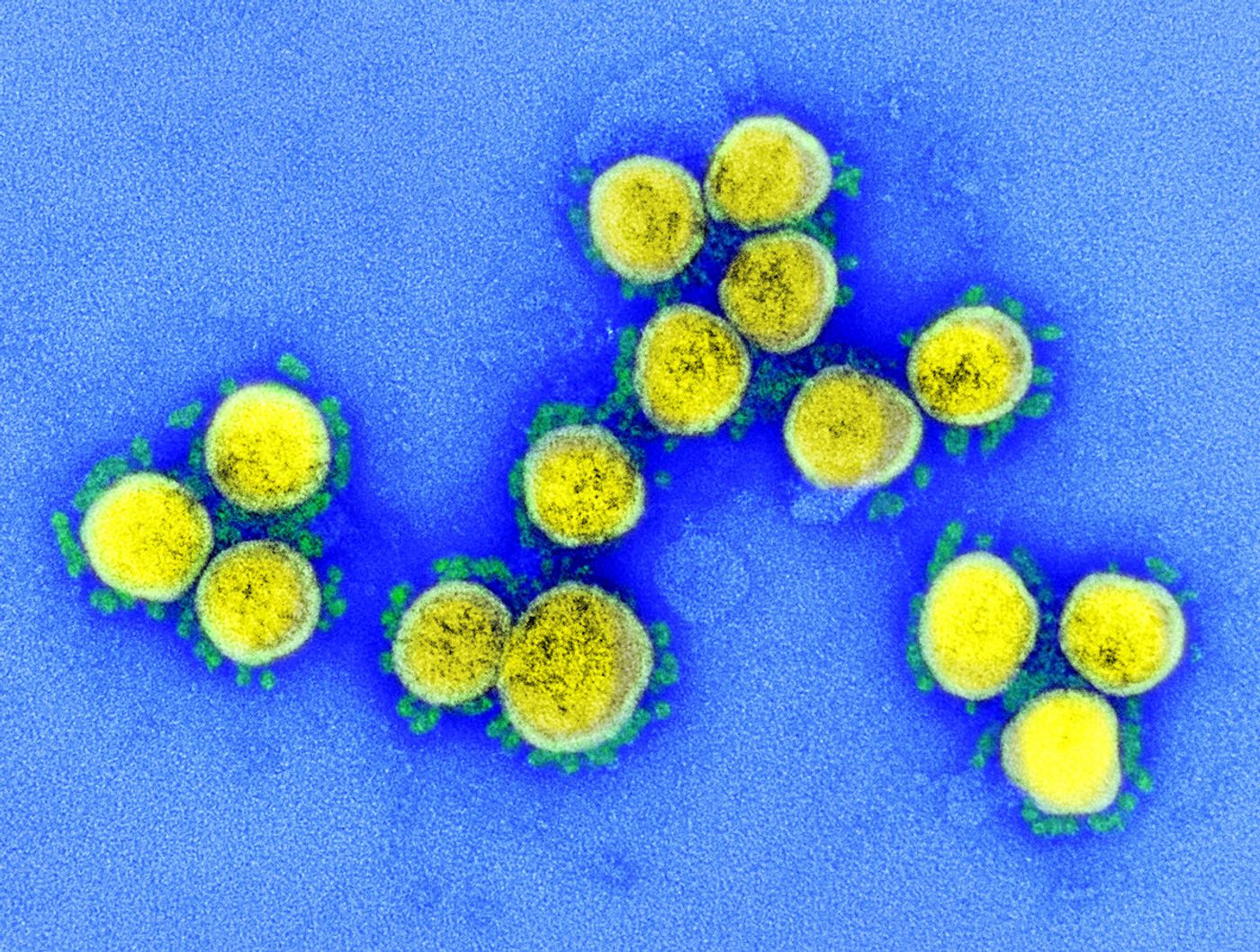
Researchers have now published a report in Brain, Behavior, and Immunity warning of the coming wave of neuropsychiatric disorders caused by the COVID-19 pandemic. Not only is society under stress, which will undoubtedly create more problems for people already dealing with mental health issues, but a host of new challenges may be on the horizon for people recovering from infections.
Their report noted that we've learned from other pandemics that symptoms like psychosis, mood changes, or encephalopathy (a general term for brain damage or malfunction) can arise in patients that have or are recovering from acute viral infection. In some cases it may takes weeks or months for the symptoms to emerge, and the authors stressed that they are not trying to alarm anyone; they want to get help to patients during their recovery.
"Our article seeks to bring the medical community's attention to the need for monitoring and investigations to mitigate such outcomes, not to cause panic among individuals whose lives are already greatly affected by this pandemic," they wrote.
"COVID-19 is a significant psychological stressor, both for individuals and communities," said senior study author Suzi Hong, Ph.D., associate professor in the departments of Psychiatry and Family Medicine and Public Health at UC San Diego School of Medicine. "There are fears of illness, death and uncertainty of the future. This pandemic is a potential source of direct and vicarious traumatization for everyone."
The authors added that society has not paid as much attention to the direct neurological effects the virus may be having. Respiratory pandemics in the 18th and 19th centuries were accompanied by a rise in anxiety, depression, delirium, insomnia, and suicidality. It's worth noting that it has not been established that the virus was responsible for these observations; it may have been caused by something else or been one of many influences that led to those outcomes. However, we know that viruses can invade the brain and may damage the central nervous system, including the brain. Studies have also shown that there is a link between influenza and encephalopathy. It has even been suggested that depression is a kind of infectious disease. It seems that viruses are respponsible for neurological symptoms in at least some patients.
"Reports are already surfacing of acute CNS-associated symptoms in individuals affected by COVID-19," said Hong, including greater incidence of stroke in severely infected patients in Wuhan, China, as well as delirium and the loss of the sense of smell and taste. A recent report in the International Forum of Allergy & Rhinology has shown that two to four weeks after the infection, those senses return.
Although we don't yet know how COVID-19 will impact a patient's mental health, those effects are likely to be significant and last for years, said the authors. The immune status of the neurological system and mental health of anyone that is recovering from the infection should be monitored, they added.
"We will need to do this at different points in their lives, for years to come, to fully appreciate this pandemic's effects on neuropsychiatric outcomes for differing age groups, and how to better prepare for pandemics to come," Hong said.
Sources: AAAS/Eurekalert! via University of California - San Diego; Brain, Behavior, and Immunity