The Immune System Can Kill HIV with a Helper Molecule
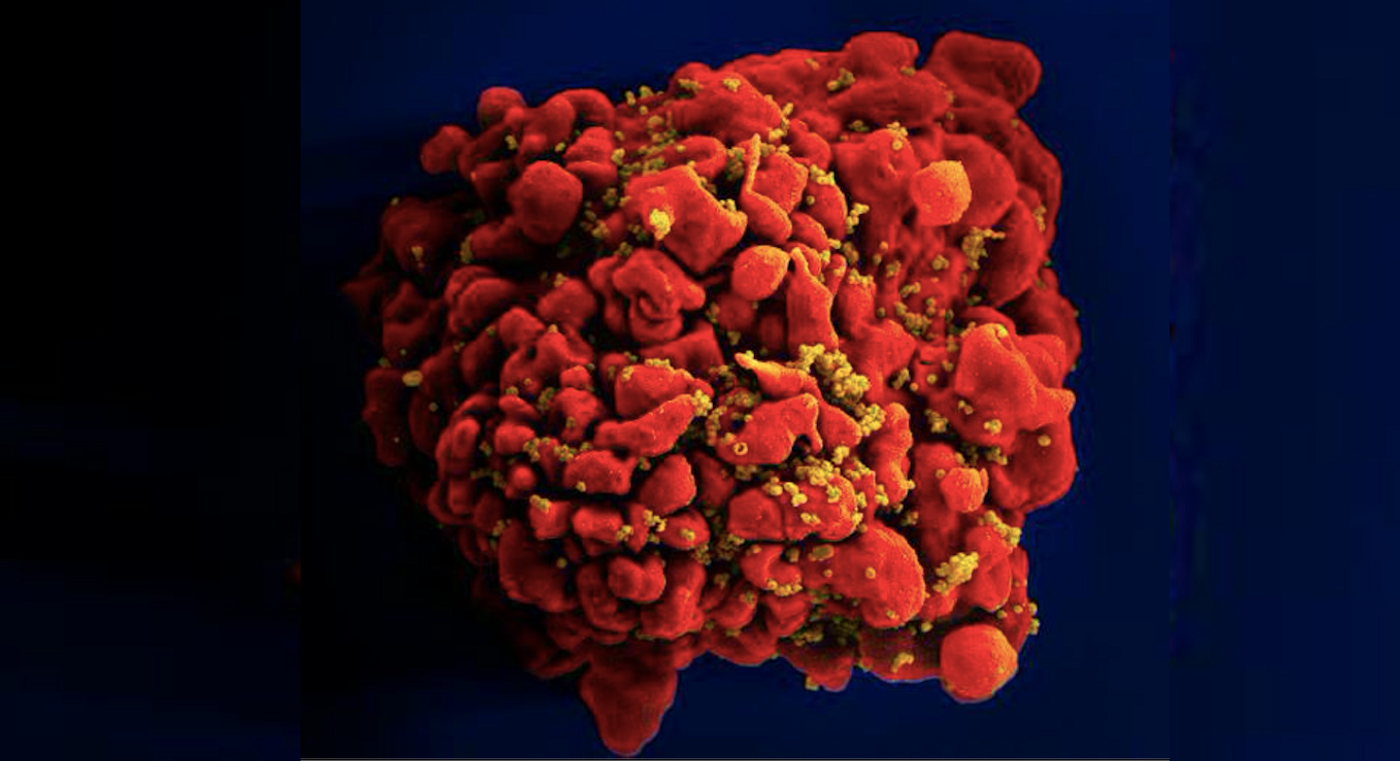
HIV is an insidious virus that has incredible survival abilities. It attacks the human immune system's CD4 cells, a major player in the body's defense against pathogens. While drugs that suppress the virus have been developed, it is still able to hide away in the genome, ready to emerge at any time and cause illness. If a case of HIV is going to be completely cured, those latent viral reservoirs have to be destroyed. Otherwise, HIV patients have to continue to take medications that keep the virus at bay.
"If they ever stop, in short order the virus rebounds and resets at the high levels seen before starting, and that seems to be the case even after decades of therapy," said Mark Painter, Ph.D., a graduate student in the University of Michigan Medical School's department of microbiology and immunology.
Decades ago, researcher Kathleen Collins, M.D., Ph.D., found that HIV can use a protein called Nef to interfere with a cell-surface protein, MHC-1, that would normally tell the immune system that a cell is infected with a pathogen and has to be eliminated. Nef disables MHC-1, and infected cells can keep dividing. Researchers led by Collins wanted to target Nef.
First, they looked for a drug that could target Nef and was already approved. This would theoretically restore the normal action of MHC-1, and the immune system could then use cytotoxic T lymphocytes as it normally would to identify and destroy cells infected with HIV.
"We started out screening a library of 200,000 small molecules and found none inhibited Nef," said Painter. They sought assistance from the lab of David Sherman, Ph.D. of the U-M Life Sciences Institute, where researchers study the biosynthesis of natural products from microbes.
"Often synthetic molecules have quite a low molecular weight, meaning they are fairly small. And if you need to disrupt a large protein surface or interface, such as with Nef, a small molecule won't work well or at all," said Sherman. "A natural products library like the one at the LSI, on the other hand, is going to have molecules with a large range of weights and sizes."
They screened about 30,000 molecules to find a class of antibiotic molecules called pleicomacrolides that could inhibit Nef.
"Pleicomacrolides are widely used in lab experiments when you want to shut down the lysosome. Because of this, they are considered toxic and risky to use as drugs," said Painter.
The cell uses an organelle called the lysosome to break down degraded or unwanted parts. One pleicomacrolide, concanamycin A, can inhibit Nef without inhibiting the lysosome if it's used at the right concentration. In a cell culture model, HIV-infected cells that express Nef were eliminated by cytotoxic T cells after concanamycin A exposure. The findings have been reported in the Proceedings of the National Academy of Sciences.
"As a lead compound for drug development, it's fairly exciting because we can use a very low dose, and inhibit Nef without short-term toxicity to the cells," said Painter.
"It's been extremely gratifying for this project, which began in my lab over a decade ago to finally come to fruition. I had hoped we would find something that worked as well as this compound does but it was never a guarantee that we would actually be successful. This type of research is risky but extremely important because of the potential reward," said Collins. She cautioned that the drug is not ready for use in patients yet. "More research will be needed to optimize the compound. We will need to further separate the potent Nef inhibitory activity from the more toxic effect on lysosomal function to make it a viable therapy."
Sources: AAAS/Eurekalert! via Michigan Medicine, Proceedings of the National Academy of Sciences